Browse through our Journals...
The Decline of NHS Inpatient Psychiatry in England
Professor Ben Green, Consultant Psychiatrist Cheadle Royal Hospital, Visiting Professor of Psychiatry, University of Chester and Honorary Senior Lecturer University of Liverpool, FRCPsych FHEA MB ChB
Abstract
Background
Historically the NHS has reduced mental health bed numbers since the 1950s. This paper looks at whether NHS psychiatry bed numbers have further declined in the last decade and how this has affected admissions in England for various ICD-10 diagnoses in recent years.
Aims
To examine the fall in NHS bed numbers for mental health in the last decade and the effect on annual admissions and bed days for various ICD-10 diagnoses from 2002-2007.
Method
Government statistics for NHS bed numbers and admissions by diagnosis were commissioned from a Department of Health agency and obtained from the HSEOnline website. The analysis focused on the 15-59 age range. These were statistically analysed by logistic regression methods using the SAS statistical package. Bed figures for the Independent sector were compared descriptively.
Results
In the last ten years there has been a highly significant fall in the number of NHS mental health beds. This is associated with a highly significant reduction in the annual admissions for schizophrenia, depression, bipolar disorder, depression, and stress and anxiety related disorders in England. There has been no fall in admissions for eating disorders. There has been a significant increase in NHS admissions for alcohol related disorders. There has been an increase in the numbers of NHS psychiatric patients admitted to independent sector psychiatric beds.
Conclusions
There has been a highly significant recent decline in the number of NHS provided mental health beds and a corresponding fall in psychiatric admissions for a variety of diagnoses.
Declaration of Interest
BG is a consultant psychiatrist works at Cheadle Royal Hospital, an Independent sector hospital
Introduction
Historically the NHS has always contained many thousands of inpatient psychiatric beds.
At its inception in 1948 over half the inpatient beds in the NHS belonged to psychiatry. The rise in public psychiatry beds occurred well before the NHS however as Figure 1 shows. This represents a substantial county asylum building program. Shortly after the inception of the NHS there was a peak provision in 1955 of some 150,000 mental health beds. In conjunction with the development of effective antipsychotic medication the number of NHS mental illness beds began to fall.

Figure One: Public Mental health Bed Numbers 1850-2007 (NB Population in 1850- 17 million, Population in 2007 61 million). The peak is in 1955.
In Sir David Goldberg’s recent paper in the BJPsych he noted an incremental reduction in mental health beds in recent years (mainly in acute mental health) along with an increased investment in community teams1.
This paper considers whether the decline has continued in recent years and seeks to analyse overall bed numbers, admission rates for various psychiatric ICD-10 diagnoses, bed days for various conditions and also considers what figures are available for the Independent sector, which has grown during this same period.
Method
NHS bed figures are published annually by the Department of Health and can be accessed online. These are available by speciality and were obtained for each year for mental health from 1997-20072.
Databases of NHS admission figures are available online for episodes of illness though Health Episode Statistics (HESONLINE) from 2002-20063. These databases can be interrogated for admissions for various physical conditions according to ICD-10 categories. Data area further available for bed days attributed to various conditions and can be further analysed by sex and age groups (0-14, 15-59, 60-74, 75+ and unknown). The data can further be analysed by provider Trust or ‘NHS organisation’. This paper considers data for several main ICD-10 diagnostic groups across England, by sex, across all ages, and specifically in the main provided ‘adult’ group of 15-56). The paper focuses on Schizophrenia (F20 - all types combined), Bipolar Affective Disorder (F31 - all types combined), Depression (both Depressive Disorder F32 and Recurrent Depressive Disorder F33), Eating Disorders (F50- all types combined), Alcohol Disorders (Mental and behavioural disorders due to use of alcohol F10 - all types combined) and as a possible indicator of anxiety or neurotic disorders the ICD-10 category F43 (Reaction to stress and adjustment disorders – all types combined). Outpatient data for 2003-2007 are also available online, but were outside the scope of this paper.
Data for 2007 were obtained through commissioning a separate analysis from the HES team at the Department of Health specifically for this paper - ahead of routine annual publication in December.
The numbers of NHS beds, admission numbers and bed days for various years and diagnoses were compared across years using a log-linear model for non-ordered categorical variables by the method of maximum likelihood4 using the Statistical Analysis System (SAS)5 .
Finally a literature search of MEDLINE, PSYCInfo, CINAHL, the Cochrane Library, Biomed , PsycARTICLES, Intute, Scopus and Science Direct databases was conducted to detect recent relevant papers on NHS mental health bed numbers. The HANSARD database was also consulted for any recent parliamentary questions and answers on mental health bed numbers.
Results
Data from the Department of Health bed availability data and UK Parliamentary Written Answers yield figures demonstrating an inexorable decline in NHS mental health beds in England in the last decade, (Figure 2) 2,6.

Figure 2: NHS English Mental illness beds 1997-2007
In early 2007 there were about 28,800 mental health beds in all specialities including acute, rehabilitation, old age, child and so on. Later the same year however the figure had fallen to about to 27,914 beds and the NHS provision is currently declining by about 1,000 beds per year. At some point this may plateau, but there is no sign of this as of yet. If the rate of decline continues trend forecasting would project a figure of 26121 beds in 2010 and 17205 beds in 2020.
The continuing fall in NHS mental health beds from 1997 onwards (Figure 4) was analysed statistically using logistic regression. The decline in all years was statistically significant (p<.0001) and compared relative to 2007 figures the odd ratios of having a mental health bed in each previous year varied from 1.06 for 2006 to 1.36 for 1997.
Government occupancy figures for various PCT’s across the country indicate for mental health beds that the occupancy rate is about 90%, but independent surveys have topped 120% in some inner city areas7.
Schizophrenia
Male and female admissions for all F20 diagnoses of schizophrenia (including paranoid, hebephrenic, catatonic, residual etc.) were considered for the years from 2002-2007 and the number of admissions across all ages, admissions for the age range 15-59 and total bed days across the year obtained (Table One).
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
14391 |
13968 |
14677 |
13558 |
9835 |
Female Total |
7262 |
7169 |
7434 |
6776 |
4913 |
15-59 Male |
13321 |
12886 |
13549 |
12413 |
8950 |
15-59 Female |
5655 |
5562 |
5755 |
5228 |
3835 |
Bed days Male |
1165034 |
1202816 |
1422572 |
1285701 |
850943 |
Bed days Female |
1729972 |
1788078 |
2068333 |
1870301 |
335752 |
Table One: Admissions for Schizophrenia (F20) in the NHS for England 2002-2007
The figures for the approximately adult working age range (15-59) are presented graphically in figure five. These show a gradual fall in the number of admissions. Most admissions are for males with a marked fall in bed days for males and a 75% decrease in bed days for females in 2006-2007.
Schizophrenia admissions (F20) for 2002-2007 (Table 1) were analysed using logistic regression and declined in a statistically significant way (p<.0001) , with odds ratios for admission in 2005/2006 relative to 2006/2007 being 1.39 and 2002/2003 relative to 2006/2007 being 1.49. That is to say relative t 2006/2007 all previous years patients with schizophrenia had a higher likelihood of being admitted. There was no significant difference in the decline for males and females. Bed days for schizophrenia also decrease significantly as the years went by (p<0.0001, with odds ratios for past years relative to 2006/2007 varying between 1.37 and 1.52). There is a significant difference in the decline in bed days for males and females (p<0.0001 with odds ratios varying between 3.68 and 3.76). A Wald chi-square text on the effect of the overall bed number reduction on admission figures for schizophrenia showed a significant effect (Wald chi-square 13.0658, df=4, prob =0.01).
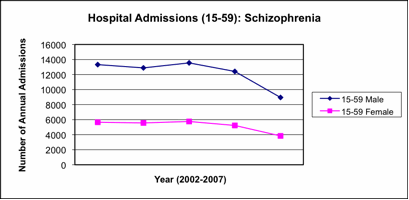
Figure Three: English NHS Admissions for Schizophrenia amongst 15-59 year olds 2002-2007

Figure Four: NHS Bed Days for Schizophrenia 2002-2007
Affective Disorders
Male and female admissions for all F31 diagnoses of bipolar affective disorder were considered for the years from 2002-2007 and the number of admissions across all ages, admissions for the age range 15-59 and total bed days across the year obtained (Table Two). The usual length of stay was between 50 and 60 days. The data for bipolar affective admissions for the 15-59 age range are presented graphically in Figure Seven.
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
4998 |
4618 |
4929 |
4510 |
3780 |
Female Total |
8046 |
8491 |
7588 |
7085 |
5672 |
15-59 Male |
4027 |
3771 |
3944 |
3577 |
2952 |
15-59 Female |
5851 |
6182 |
5430 |
5012 |
3984 |
Bed days Male |
257869 |
249711 |
279299 |
259814 |
159022 |
Bed days Female |
416575 |
437177 |
429272 |
396104 |
208547 |
Table Two: Admissions for Bipolar Affective Disorder (F31) in the NHS for England 2002-2007
Admissions for bipolar disorder (F31) for 2002-2007 were analysed using logistic regression and declined in a statistically significant way (p<.0001) , with odds ratios for being admitted in 2005/2006 relative to 2006/2007 being 1.21 and 2002/2003 being 1.36.
There was no consistently significant difference in the decline in admission numbers for males and females.
Bed days for bipolar disorder also decrease significantly as the years go by (p<0.0001 with odds ratios varying between 1.57 and 1.75) and there is a significant difference in the decline for males and females (p<0.0001 with odds ratios varying between 1.16 and 1.33). The number of available beds did not have a statistically significant effect on admissions for bipolar disorder.

Figure Five: NHS Admissions for Bipolar Affective Disorder 2002-2007
Male and female admissions for both F32 and F33 diagnoses of depressive disorder (F32 being depressive episodes of varying severity and F33 being recurrent depressive disorder) were considered for the years from 2002-2007 and the number of admissions across all ages, admissions for the age range 15-59 and total bed days across the year obtained (Tables Three and Four). The usual length of stay for depressive episodes was between 30 and 40 days, and this shows no particular trend downwards. The data for depressed admissions for the 15-59 age range are presented graphically in Figures Six and Seven.
Admissions for depressive episodes for 2002-2007 were analysed using logistic regression and these declined in a statistically significant way (p<0.0001) , with odds ratios of being admitted for 2005/2006 (relative to 2006/2007) being 1.17 and 2002/2003 being 1.29.
There were significant differences in the decline in admission numbers for males and females in most years, but not all (2005-2006 being an exception).
Bed days for depressive episodes also decrease significantly as the years go by (p<0.0001with odds ratios varying between 1.1 and 1.36) and there is a significant difference in the decline for males and females (p<0.0001 with odds ratios varying between 1.04 and 1.08).
A Wald chi-square text on the effect of the overall bed number reduction on admission figures for depressive episodes showed a significant effect (Wald chi-square 1184.89, df=4, prob =0.0001).
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
9280 |
8958 |
8695 |
8190 |
6648 |
Female Total |
14489 |
13365 |
12533 |
11330 |
10922 |
15-59 Male |
6257 |
6174 |
5960 |
5672 |
4817 |
15-59 Female |
8650 |
8082 |
7861 |
6787 |
5611 |
Bed days Male |
309036 |
292939 |
290992 |
250033 |
226640 |
Bed days Female |
551200 |
518342 |
499458 |
439465 |
372348 |
Table Three: Admissions for F32 depressive episodes in the NHS for England 2002-2007
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
2418 |
2195 |
2240 |
1924 |
1581 |
Female Total |
5576 |
4957 |
4817 |
4294 |
3310 |
15-59 Male |
1494 |
1350 |
1217 |
1041 |
869 |
15-59 Female |
3205 |
2709 |
2606 |
2219 |
1660 |
Bed days Male |
52224 |
44789 |
45276 |
39853 |
30831 |
Bed days Female |
263800 |
103578 |
103011 |
80168 |
57852 |
Table Four: Admissions for F33 (Recurrent depression) in the NHS for England 2002-2007
Admissions for Recurrent Depression (F33) for 2002-2007 were analysed using logistic regression and declined in a statistically significant way (p<.0001) , with odds ratios for 2005 being 1.19 and 2002 being 1.71.
There were no significant differences in the decline in admission numbers for males and females.
Bed days for depressive episodes also decrease significantly as the years go by (p<0.0001with odds ratios varying between 1.29 and 1.69) and there is a significant difference in the decline for males and females (p<0.0001 with odds ratios varying between 1.07 and 2.69).

Figure Six: NHS Admissions for F32 Depressive Episodes 2002-2007

Figure Seven: NHS Admissions for F33 Recurrent Depressive Disorder 2002-2007
Most NHS admissions for affective disorder are for females [comment on epidemiology here]. In both F32 and F33 diagnostic categories there has been a consistent and marked decline in the number of admissions for both males and females between 2002-2007.
In 2002-2003 there were in total some 31,763 adult admissions for depressive disorders F32 and F33, but the number of admissions fell to a total of 22,461 in 2006-2007. This represents a fall of 9,002 admissions across England and in percentage terms this is a 28% reduction in five years.
Eating Disorders
Figures for admissions are presented in Table Four and presented graphically for the 15-59 age group in Figure Eight.
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
136 |
122 |
154 |
200 |
193 |
Female Total |
1397 |
1373 |
1497 |
1682 |
1452 |
15-59 Male |
81 |
70 |
89 |
128 |
109 |
15-59 Female |
1113 |
1102 |
1214 |
1365 |
1190 |
Bed days Male |
5317 |
5689 |
4909 |
7479 |
4112 |
Bed days Female |
71588 |
74503 |
81719 |
82261 |
58414 |
Table Five: Admissions for F50 Eating Disorders in the NHS for England 2002-2007

Figure Eight: NHS Admissions for F50 Eating Disorders (15-59) 2002-2007
Admissions for Eating Disorders (F50) were analysed using logistic regression. There was no statistically significant change in overall admissions, but a significant change was found in bed days (p<0.0001 with odd ratios varying from 1.29 in 2002-2003 to 1.82 in 2005-2006). A Wald chi-square text on the effect of the overall bed number reduction on admission figures for eating disorder showed no significant effect.
Stress and Anxiety Related Disorders (F43)
The data for anxiety disorders reveals that despite a pressure on overall bed numbers there are still admissions with primary diagnosis of anxiety disorder (Table Six). The overall trend though is downward (Figure Nine).
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
2964 |
2714 |
2662 |
2152 |
1904 |
Female Total |
2979 |
2759 |
2525 |
2180 |
1849 |
15-59 Male |
2734 |
2471 |
2384 |
1867 |
1671 |
15-59 Female |
2653 |
2429 |
2194 |
1860 |
1562 |
Bed days Male |
40793 |
45991 |
45331 |
39108 |
28340 |
Bed days Female |
50040 |
54316 |
52575 |
45255 |
26548 |
Table Six: Admissions for F43 Stress and Anxiety Related Disorders in the NHS for England 2002-2007

Figure Nine: NHS Admissions for F43 Stress and Anxiety Related Disorders (15-59) 2002-2007
Admissions for Anxiety Related Disorders for 2002-2007 were analysed using logistic regression and declined in a statistically significant way (p= less than or equal to .001), with odds ratios for 2005/2006 being 1.12 and 2002/2003 being 1.63.
There were no significant differences in the decline in admission numbers for males and females.
Bed days for anxiety also decrease significantly as the years go by (p<0.0001with odds ratios varying between 1.38 and 1.62) and there is a significant difference in the decline for males and females (p<0.0001 with odds ratios varying between 1.23 and 1.30).
A Wald chi-square text on the effect of the overall bed number reduction on admission figures for stress and anxiety related disorders showed a significant effect (Wald chi-square 147.13, df=4, prob =0.0001).
Alcohol related disorders (F10)
The F10 category is a broad one encompassing acute intoxication, delirium tremens and dependence. All of these present quite differently and require differing inpatient service responses. It is unlikely that all these admissions were to adult mental health inpatient beds, but that a fair proportion were instead to accident and emergency and medical beds. The main point is to observe the very rapid recent acceleration of admissions to the NHS related to alcohol. This increasing trend is most likely to continue.
Admissions |
2002-2003 |
2003-2004 |
2004-2005 |
2005-2006 |
2006-2007 |
Male Total |
19528 |
21794 |
24769 |
27116 |
27841 |
Female Total |
10335 |
10204 |
11577 |
12747 |
12212 |
15-59 Male |
16389 |
18119 |
20871 |
22759 |
23527 |
15-59 Female |
5851 |
7777 |
9084 |
10123 |
9762 |
Bed days Male |
158026 |
161181 |
169031 |
149194 |
135847 |
Bed days Female |
71088 |
73035 |
74215 |
71806 |
57203 |
Table Seven: Admissions for F10 Alcohol Related Admissions in the NHS for England 2002-2007

Figure Ten: Admissions for F10- alcohol related disorders
Admissions for Alcohol Related Disorders for 2002-2007 were analysed using logistic regression and increased in a statistically significant way (p= less than or equal to 0.001), with odds ratios for 2005/2006 relative to being admitted with an alcohol related disorder in 2006/2007 being 0.96 and 2002/2003 being 0.69.
Bed days for anxiety also change significantly as the years go by (p<0.0001with odds ratios varying between 1.09 and 1.24) and there is a significant difference in the change for males and females (p<0.0001 with odds ratios varying between 1.06 and 1.14).
Independent Sector
The turnover of independent mental health hospitals in 2006 was estimated by Laing & Buisson at £845 million, compared to the NHS in-house supply cost of inpatient, outpatient and community services of £9.5 billion for the UK8. The independent sector’s share of the mental healthcare sector is thus about 8%. The majority (85%) of independent mental health hospital beds are funded by the NHS. The data for the Independent sector are not collated in a directly comparable way to the NHS HSE data. Over 50% of independent sector beds are probably for patients detained under the Mental Health Act. Medium secure beds accounts for 24% of the total capacity and acute psychiatry for about 20%. Brain injury rehabilitation accounts for 7% of bed provision. Over fifty percent of the Independent Sector beds are provided by four groups: Partnerships in care, Priory Healthcare, St Andrews Group and Care Principles. Table Eight shows that bed numbers are steadily increasing. Independent Sector mental health hospital revenues have been growing at between 16% and 20% annually in recent years.
Numbers of Hospitals/Units |
Numbers of Beds |
|
2003 |
168 |
6212 |
2004 |
175 |
6370 |
2005 |
213 |
6942 |
2006 |
227 |
7616 |
2007 |
229 |
8030 |
Table Eight: Numbers of Independent Sector Mental Health Units and Beds 2003-2007 (Laing & Buisson)

Figure 11: Independent Sector Psychiatric Beds 2003-2007 (Laing & Buisson)

Figure 12: Independent Sector Psychiatric Units / Hospitals 2003-2007 (Laing & Buisson)
In 1998 Laing & Buisson estimated that 9% of all acute psychiatric beds were provided by the independent sector with a third of these being NHS funded 9.
Outpatient Activity
HESOnline data also includes some statistics regarding NHS outpatient activity in England3. The activity shows an increase in recent years, but the meaning of the increase is unclear as the nature of the contacts and with whom depends on interpretation of the definitions concerned. For instance ‘first attendance’ appointments for F20 Paranoid Schizophrenia rose from 304 in 2003/2004 to 2493 in 2006/2007. ‘All attendances’ for appointments for F20 Paranoid Schizophrenia rose from 2713 in 2003/2004 to 14665 in 2006/2007.
Discussion
Doctor Pangloss was a character in Voltaire’s satire Candide who espoused a particularly flawed, but admirably optimistic philosophy. Essentially Panglossian philosophy was that all was for the best. Typical Panglossian logic is exemplified by this quote:
‘It is demonstrable, ‘ said he, ‘that things cannot be otherwise than as they are; for as all things have been created for the best end. Observe for instance, the nose is formed for spectacles, therefore we wear spectacles’.
The received political wisdom is that the massive investment in home treatment teams for ‘severe and enduring mental illness’ including assertive outreach, early intervention and crisis intervention teams has allowed a reduction in hospital admissions and thereby prompting mental health beds to be further reduced.
This political stance has been echoed by research papers noting the coincidence of increasing community team expenditure (e.g. on crisis resolution teams) and the fall in inpatient admissions and assuming a causal relationship 10, 11. This in itself may be an example of Panglossian reasoning. Glover et al‘s 2006 paper for instance fails to take account of a simultaneous and dramatic fall in capacity on admission rates or an increase in use of independent sector beds11. A fall in capacity and permanently high occupancy levels (sometimes reportedly above 100%) of those beds form a distinct barrier to inpatient admissions. Added to this are the increasingly unpleasant nature of remaining inpatient beds and the increasing use of Mental Health Act compulsion to admit people to these beds 12. Acute admission wards in 2006 were characterised as being poorly designed, poorly maintained and with a lack of therapeutic and leisure activities leading to boredom, aggression and violence, with a resulting concentration of a more challenging group of patients 13.
Over the last decade the Mental Health Act Commission has regularly been reporting occupancy rates of over 100% on some 40% or so of adult acute wards visited by the Commission. Inpatient beds are thus less refuge or ‘asylum’ than themselves a source of stress and less than intrinsically therapeutic. According to a 2008 Health Care Commission survey of all 69 trusts providing acute mental healthcare – involving some 554 wards. 23% of wards were deemed ‘weak’ on a range of factors with nearly 20% were deemed weak for safety 14.
Perhaps these negative features of acute wards and their diminishing numbers of beds are more linked to a fall in admissions for depression than any potential benefits of home treatment. For the in-patient beds that remain the ward atmosphere may no longer be therapeutic or conducive to recovery for depressed patients. Incidents on such wards have the capacity to be damaging to staff as well 15. Bowers and Nijman have estimated the risk of physical injury to inpatient nursing staff to occur to 1 in 10 nurses per year 16.
The reduction in beds and organisation of community teams is largely based on philosophical ideas 17. The physical alteration to services of bed closures is thus conducted on a philosophically weighted and relatively evidence-light basis. This could be characterised as a brave, uncontrolled experiment, but one conducted without the involvement of a research ethics committee, and the absence of any patient consent. The overall intentions may be laudable, and the eventual outcome could be good, but there is seemingly no will to co-ordinate measurement of the effects of the experiment before and after the intervention. The reduction in beds is, for now, seemingly irreversible and for the next decade at least the mentally ill patents of the NHS must make do mainly with community care. Even so, the jury on community care is still out. Evaluative papers on community care even now stress their preliminary nature 18, but the policy has already been implemented in the UK.
The most recent Cochrane review of crisis intervention for severe mental illness concluded that there were few studies that met their inclusion criteria and that although home treatment and crisis intervention were possible management strategies some 45% of patients eventually required admission 19. Crisis intervention is unsuited to un-cooperative patients and patients at risk of self neglect 20. The Cochrane team concluded to that ‘If this approach is to be widely implemented it would seem that more evaluative studies are still needed’ 19.
The most recent Cochrane review of early intervention for psychosis also found it difficult to locate sufficient high quality studies 21. They included seven studies, but noted that all these all adopted different interventions and as they were unable to identify sufficient trials they were unable to draw any definitive conclusions and proposed a ‘concerted international programme of research to address key unanswered questions’. If we conceptualise, just for a moment, ‘crisis resolution’ and ‘early intervention’ to be drug treatments for an individual patient the Cochrane reviews hardly seem to be ringing endorsements as the basis for prescription. Nevertheless these newer modes of management have been rolled out across the country and previous methods of management swiftly jettisoned. The previous status quo of standard inpatient/outpatient psychiatry had its problems undoubtedly, but now, after the event, can we really justify or rationalise the physical change in our services on the basis of solid evidence? In the longer term the proponents of community care and the destruction of inpatient psychiatry could be judged correct, but the decisions to visit changes on services were not made on adequate biomedical evidence.
Government Ministers have used suicide rates to suggest that mental health policies are effective in inpatient and community settings. In 2008 the Care Services minister described a reduction in total numbers of suicides among mental health in-patients as ‘encouraging’, but failed to factor in a declining number of inpatient beds. A comparison of the ratio of suicides to mental health beds makes a less impressive statistic. In 1998 there were some 187 inpatient suicides 22 in the context of 38,000 beds and in 2005 the Minister was noting 157 suicides in 2004 in the context of 32252 beds. The ratio is comparable.
Hospitalisation has often been vaunted as an outcome measure for various interventions23 . The fall in inpatient capacity and associated barriers to admission would indicate that hospitalisation rates should not necessarily be seen as reliable outcome measures unless this decline in beds is controlled for.
Discussion on particular diagnostic categories
The data show a decline in admissions and bed days for schizophrenia with a steeper decline for females with schizophrenia. The decline is statistically linked to a pre-existing and continuing fall in overall mental health bed numbers. Although there has been a significant fall in admissions for bipolar disorder, this decline is less affected by the overall decline. This may reflect the dramatic nature of presentations with bipolar disorder and a relatively higher pressure to admit to a diminishing supply of NHS beds than with other diagnoses.
Admissions for depression and stress and anxiety related disorders also declined significantly with significantly more reduction in female admissions. This could reflect a more troubling or threatening ward environment in mixed acute wards, which makes them less conducive to female admissions. It would be interesting to analyse the above figures for various diagnoses with annual data on the proportion of admissions for males and females under the Mental Health Act to see whether there may be pressure against voluntary admissions, particularly for females.
There was a highly significant association between overall mental health bed reductions and declining depressive episode admissions, perhaps suggesting particular barriers to admission for patients with depression. There is an urgent need to study this area further as previously depression and anxiety were the most common reasons (29.6%) for admission in 1999/2000 24. Particularly needed are studies that measure the levels of distress in patients with depression in community settings, whether they are in contact with services, whether they are receiving evidence based treatments from adequately trained practitioners, suicide rates in this particular diagnostic grouping and the associated quality of experience of patients and relatives coping in the community.
Surprisingly against a trend of reducing adult mental health beds and discernible pressure against admissions for depression and schizophrenia there has been no reduction in admissions for eating disorders. This could reflect an increase in the numbers of cases presenting with eating disorders or the relative severity of presentations to the NHS has increased over these years. Further research is warranted.
Against a fall in bed numbers for psychiatry and admissions for schizophrenia and depression there has been a significant expansion in NHS admissions for alcohol related disorders. It is not easy to glean from the figures whether these are admissions to general and/or mental health NHS beds. There could be future pressure from general units to reduce these admissions by suggesting transfer to psychiatric management. Psychiatric inpatient capacity probably no longer exists for inpatient alcohol detoxification and dependence. Existing psychiatric outpatient services may not be able to take on board the risk of safely monitoring severely dependent alcohol patients who may have a higher mortality during detoxification. Pressure may arise for a return to district alcohol inpatient units.
Although there is reluctance in the public (and insurance sectors) to pay for inpatient detoxification and dependence services, this situation may have to change to cope with severe effects (physical and psychiatric) on population health associated with alcohol misuse. The increase in admissions so far is a signal for a potential change and may represent an opportunity to plan for new services – both outpatient and inpatient in nature.
Discussion on Future Mental Health policy
Given the relatively permanent nature of the changes wrought by the political strategy (reduction in bed capacity through closure of beds and employment of teams - with intrinsic cost barriers to any redeployment or termination) there is considerable impediment now to any change in direction. Inpatient beds once closed are not easily reopened, inpatient teams are not easily recruited and trained, outpatient teams are not easily redeployed and contracts not easily cancelled.
It is inevitable that psychiatric training will be impacted if NHS opportunities to admit and manage are reduced. If certain types of patients are increasingly being fed into independent sector beds and trainees are focussed purely in the NHS then trainees will never gain the skills necessary to manage these types of patients. Training implications need to be managed, especially if the changes described above are to be permanent.
Should any change of heart occur with regard to inpatient mental health due to media controversy about the state of inpatient facilities or adverse consequences due to failure to admit then the clear strategy of running down inpatient NHS care will be very difficult to halt, let alone reverse.
If a change of heart did occur then parallels could then be drawn to the analogous situation in the 1800s where political will was there to create inpatient settings for the mentally ill, but the public sector could not gear itself up quickly enough. After the County Asylums Act of 1808, the first institution opened its doors in 1811. By 1827, there were still only nine county institutions open, and many patients were being held in jails and treated as prisoners and criminals instead of like mentally ill patients.
There was thus an initial reliance on the independent sector with some attendant media controversy (e.g. the Haydock Lodge scandal of c.1845 where patient mortality was high and legislators, commissioners and providers were one and the same). The role of the independent sector today in providing current spare capacity has been criticised by NHS staff 25. Nevertheless, as the NHS inpatient rundown continues unabated, if there is any change of heart, there must first be a halt in the process. This is not yet apparent. The decline in NHS capacity will therefore continue until any change of Governmental heart occurs, perhaps in response to media controversy. At this point NHS re-gearing will be difficult to achieve quickly enough and probably the Independent sector will be engaged to provide acute inpatient psychiatry for the NHS.
Recent concern expressed by the Royal College of Psychiatrists was intended as a wake-up call for British psychiatry 26 (Craddock et al, 2008). The inexorable and continuing decline in English inpatient mental health indicates that the wake up call has yet to be heard by anybody in charge of the rundown of inpatient psychiatry.
Conclusions
There has been a highly significant reduction in NHS mental health beds in the last decade. This has been associated with a decline in the numbers of admissions of and bed days for a variety of ICD-10 mental disorders. For schizophrenia and depression there has been more marked decline in bed days for female rather than male admissions. The reduction in admissions for schizophrenia, depression and anxiety related disorder were statistically associated with the decline in bed numbers, highly so for depressive episodes and anxiety related disorders.
Admissions for eating disorders seem not to be reducing, perhaps suggesting a change in the epidemiology or detection of eating disorders, and offering an opportunity for further research. The NHS saw significantly increased numbers of admissions for alcohol related disorders, which may have profound implications for the use of a diminishing supply of mental health beds.
If the independent sector growth rate is an expansion rate of 100% per decade then the apparent NHS bed closure may actually represent which there is a switch of inpatient beds directly provided by the NHS to those provided by a smaller independent sector.
The political claim that increased spending on community teams has resulted in a fall in inpatient admissions is probably only partially correct. Barriers to admission and the switch to the independent sector need to be factored in. The overall situation is far more complex and worthy of further epidemiological investigation; particularly before the planned loss of any more NHS inpatient beds.
Professor Ben Green, Consultant Psychiatrist Cheadle Royal Hospital, Visiting Professor of Psychiatry, University of Chester and Honorary Senior Lecturer University of Liverpool, FRCPsych FHEA MB ChB
Declaration of Interest
Professor Green’s clinical base is Cheadle Royal Hospital, an independent hospital since 1766. The vast majority of Cheadle Royal admissions are funded by the public sector.
Acknowledgements
I am grateful to the staff of HESOnline for helping to compile the figures for 2006-2007 and to Miss E Green for her advice on early drafts of this paper.
References
1. Goldberg D.(2008) Improved investment in mental health services: value for money? Br J Psychiatry 200; 192(2) :88-91.
2. Department of Health. Hospital Activity Statistics. Accessed at various times during 2008. http://www.performance.doh.gov.uk/hospitalactivity/data_requests/index.htm
3. Health Episode Statistics Online (HESOnline). Database consulted at various times during 2008. http://hesonline.org.uk
4. Agresti, A. An Introduction to Categorical Data Analysis, 2nd edn. New York: Wiley & Sons, 1996.
5. Statistical Analysis System (SAS, SAS Inst., Inc., Cary, NC).
6. Hansard. The United Kingdom Parliament. Written Answers for 14th December 2006. Accessed August 2008. http://www.parliament.the-stationery-office.co.uk/pa/cm200607/cmhansrd/cm06214/text/61214w0027.htm
7. Desai S & Kinton M. Who’s been sleeping in my bed? The incidence and impact of bed over-occupancy in the mental health acute sector. Findings of the Mental Health Act Commission’s Bed Occupancy Survey. Mental Health Act Commission, 2006.
8. Laing & Buisson. Mental Health Services. Chapter in Laing’s Healthcare Market Review 2007-2008, 2007.
9. Select Committee on Health, Minutes of Evidence. Memorandum by Independent Healthcare Association, 1999. Accessed August 2008. http://www.publications.parliament.uk/pa/cm199899/cmselect/cmhealth/281/9032505.htm
10. Jones, A. Assertive Community Treatment: development of the team, selection of clients, and impact on length of hospital stay. Journal of Psychiatric & Mental Health Nursing 2002; 9 (3):261-270.
11. Glover, G, Arts, G, Babu KS. Crisis resolution / home treatment teams and psychiatric admission rates in England. Br J Psychiatry 2006; 189, 441-445.
12. Lelliot, P, and Audini, B. Trends in the use of Part II of the Mental Health Act 1983 in seven English local authority areas. Brit. J. Psychiatry. 2003; 182; 68-70.
13. Lelliott, P. Acute inpatient psychiatry in England. An old problem and a new priority. Epidemiologia e Psichiatria Sociale 2006; 15(2); 91-94.
14. Santry C. Inpatient mental health slammed as commissioners neglect services. Health Service Journal 2008. Accessed August 2008. http://www.hsj.co.uk
15 Bowers, L, Simpson A, Eyres, S, Nijman, H, Hall, C, Grange, A, Phillips, L. Serious untoward incidents and their aftermath in acute inpatient psychiatry: the Tompkins Acute Ward Study. International Journal of Mental health Nursing. 2006; 15(4); 226-234.
16. Bowers L, Nijman H. Aggressive behaviour on acute psychiatric wards: prevalence, severity and management. Journal of Advanced Nursing. 2007; 58(2); 140-149.
17. Wright, N, Bartlett, P, Callaghan, P. A review of the literature on the historical development of community mental health services in the United Kingdom. Journal of Psychiatric and Mental Health Nursing. 2008; 15(3); 229-237.
18. Monzani, E, Erlicher A, Lora A, Lovaglio P, Vittadini, G. Does community care work? A model to evaluate the effectveness of mental health services. International Journal of Mental Health Systems 2008; 2:10. Accessed September 2008. http://www.ijmhs.com/content/2/1/10
19. Joy CB, Adams, CE, Rice K. Crisis intervention for people with severe mental illnesses. Cochrane Database of Systematic Reviews. 2006; Issue 4. Art. No.: CD001087.
20. Cotton MA, Johnson, S, Bindman J, Sandor A, White IA, Thornicroft G, Nolan, F, Pilling S, Hoult J, McKenzie N, Bebbington P. An investigation of factors associated with psychiatric hospital admission despite the presence of crisis resolution teams. BMC Psychiatry; 2007; 7:52. Accessed September 2008. http://www.biomedcentral.com/1471-244X/7/52
21. Marshall. M and Rathbone, J. Early Intervention for psychosis. Cochrane Database of Systematic Reviews. 2006; Issue 4. Art. No.: CD004718.
22. Kapur, N, Hunt I, Webb, R, Bickley, H, Windfuhr K, Shaw, J, Appleby, L. Suicide in psychiatric in-patients in England 1997-2003. Psychological Medicine. 2006; 36 (10); 1485-1492.
23. Burns, T. Hospitalisation as an outcome measure in schizophrenia. Br J. Psychiatry. 2007; 197; suppl 50; 37-41.
24. Thompson, A Shaw, M, Harrison G, Verne, J, Davidson, H, Gunnell, D. Patterns of hospital admission for adult psychiatric illness in England. Analysis of Hospital Episode Statistics Data. Brit. J Psychiatry. 2004; 185(4), 334-341.
25. Poole, R, Ryan, T, Pearsall A. The NHS, the private sector, and the virtual asylum. BMJ 2002; 325: 349-350.
26. Craddock, N , Antebi, D, Attenburrow, MJ et al. Wake-up call for British psychiatry. Br J Psychiatry 2008; 193, 6-9.
Copyright Priory Lodge Education Limited 2009
First Published March 2009
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


