Browse through our Medical Journals...
Validation of Malay Version of Geriatric Depression Scale among Elderly Inpatients
Ewe Eow Teh and Che Ismail Hasanah
Penang Hospital and School of Medical Sciences, Universiti Sains Malaysia
E-MAIL:eeteh2000@yahoo.com
EWE EOW TEH
PSYCHIATRIC DEPT.
PENANG HOSPITAL
RESIDENSI ROAD
10990 PENANG
MALAYSIA
ABSTRACT
Aims: This study aimed to validate the Malay version of GDS among physically ill elderly inpatients.
Methods: Sixty elderly inpatients were categorized into major depression, minor depression and non-depression group, based on psychiatric clinical interview. All subjects completed the back-translated Malay version of GDS-15 and were rated by MADRS. Fifty subjects were retested with the GDS. Reliability and validity of the M-GDS were analyzed.
Results: The item-9 from Malay version-GDS-15 had no discriminatory value in differentiating cases and non-cases and poorly correlated with the total corrected item score. By omitting the item-9, the newly formed scale, M-GDS-14, had satisfactory reliability (Cronbach's alpha 0.84, test-retest reliability 0.84) and concurrent validity with MADRS (Spearman's rho 0.68). At the cut off point of 5/6, the M-GDS-14 detected all clinically significant depression with 95.5% sensitivity and 84.2% specificity, while at 7/8 it had 100% sensitivity and 92.0% specificity in detecting major depression.
Conclusion: The abbreviated version of GDS with 15 items when validated in Malaysian population results in 14 items with discriminatory values. This new Malay GDS-14 has satisfactory reliability and validity.
Introduction
The Geriatric Depression Scale (GDS) is widely used in screening depression among the elderly population. The original version (GDS-30) consisted of 30 questions in the form of yes / no and was designed for self-administration (Yesavage et al, 1983). The shorter 15 questions version (GDS-15) was later developed for easier use and better acceptability (Sheikh & Yesavage, 1986, Alden et al, 1989, D'Ath et al, 1994). Both versions (GDS-30, GDS-15) have been validated across different clinical setting, culture and language (Koenig et al, 1988, Lesher & Berryhill, 1994, Abas et al, 1998, Liu et al, 1998, Ganguli et al, 1999, Fountoulakis et al, 1999, de Craen, 2003).
There were increasing evidence that depression among the elderly is associated with higher risks of mortality and health service utilization (Koenig et al, 1989, Covinsky et al, 1999, Penninx et al, 1999). In some studies, GDS has been demonstrated to detect depression better than medical and nursing staffs (Rapp et al, 1988, Jackson & Baldwin, 1993).
Malaysia is a developing country with growing elderly population (Karim, 1997). Some local studies had looked into the mental health, including of depression among the elderly population (Chen et al, 1986, Krishnaswamy, 1997). The need to validate an easy to use screening scale for depression among our local elderly population for the future research as well as clinical practice is robust.
Aims
The primary aim of this study is to validate the Malay version Geriatric Depression Scale among the elderly inpatients hospitalized for physical illness. The optimum cut off points of the scale in detecting major depression and all clinically significant depression would be determined from the study. This study would also examine whether male and female patients respond differently to the scale, as this question had been raised in a previous report (Allen-Burge et al, 1994).
Methods
Study sample
The subjects were 60 inpatients aged 60 years and above from medical, surgical and orthopedic department at Universiti Sains Malaysia Hospital (HUSM, a 733 bedded multi discipline teaching hospital for the undergraduates and postgraduates, located at East Coast of Malaysia Peninsular). Exclusion criteria were having significant cognitive impairment (Mini-Mental State Examination, MMSE score < 24/30), history or presence of psychotic or bipolar mood disorder.
Translation of GDS
The GDS-30 and the GDS-15 was translated into Malay language (denoted as M-GDS-30, M-GDS-15 below respectively) using translation and back translation method by different bilingual medical doctors. Both the original and the back-translated English version were compared to determine the accuracy of the translation, with advice from The Centre for Languages and Translation of Universiti Sains Malaysia.
Procedure
The study protocol was approved by the Research & Ethics Committee, School of Medical Sciences, Universiti Sains Malaysia. Written informed consent was obtained from all participants after explaining the nature of the study.
A single researcher, who was trained in psychiatric interview and examination, interviewed all the subjects individually. Subjects' cognitive function was assessed using MMSE and only subjects with scores 24/30 and above were recruited. Subjects were assigned clinical diagnosis as major depression, minor depression or no depression. Diagnosis of major depression was made if subjects' clinical features met for DSM-IV criteria of major depressive episode. Diagnosis of minor depression was given if subjects were clinically significant depressed but did not met the DSM-IV criteria of major depressive episode; this included conditions met for DSM-IV diagnostic criteria of dysthymic disorder, research criteria for minor depressive disorder, recurrent brief depressive disorder. Major depression and minor depression were grouped together as all clinically significant depression. The researcher also rated the subjects depressive symptoms by using Montgomery-Asberg Depression Rating Scale (MADRS), based on the findings during the same interview. The interviewer was blind to the subjects' GDS score, which they completed later, when assigning clinical diagnosis to the individual subject.
All the 60 subjects completed the translated M-GDS-15. For those subjects who were unable to complete the self-rating scale without assistance, a research assistant read the questions orally, elicited answers from the subject and recorded his or her response. Thirty of the subjects also completed the M-GDS-30. Fifty subjects were given M-GDS-15 for second administration 2 to 3 days after the first test.
Data Analysis
Reliability
The internal consistency of the M-GDS-15 was assessed using corrected item-total correlation and Cronbach's alpha coefficient. Correlation between the total scores of first and second administration of M-GDS-15 was computed for test-retest reliability.
Validity
The clinical diagnosis made was the gold standard in classifying subjects into no depression, minor depression or major depression. Individual item validity was tested against the clinical diagnoses using Chi square test (or Fisher's exact Test). To test the hypothesis that the total score of the scale as a valid indices of depression, Kruskal-Wallis test was used in which the classification variable served as a between-subjects factor while the subjects' total scores on the M-GDS-15 served as the dependent measure.
The correlation between the score on the M-GDS-15 and MADRS was used to indicate concurrent validity. The correlation between total scores on the M-GDS-15 and M-GDS-30 was determined to check M-GDS-15 adequacy to substitute the full scale of 30 items.
The optimum M-GDS-15 cut-off score for major depression (versus non-major depression) and clinically significant depression (versus no depression) would be determined by the Receiver Operating Characteristic (ROC) curves separately. The sensitivity, specificity, positive and negative predictive value was computed for the respective optimum cut-off scores.
Mann-Whitney U test was used to examine the difference between the GDS scores by the two different gender; ROC curves were also plotted separately for male and female subjects to determine the optimum cut off points for each gender.
Results
Subject characteristics
The participants' age range from 60 to 83 years, with the mean of 67.3 years (S.D. 6.2 years). Among the 60 participants, 22 were clinically significantly depressed; 10 were major depression and 12 minor depression (Table 1).
Table 1. Demographic characteristics of the different clinical depression groups
Characteristics |
Major Depression |
Minor Depression |
All Clinically Significant Depression |
No Depression |
Gender: |
|
|
|
|
Male |
6 (17.6%) |
7 (20.6%) |
13 (38.2%) |
21 (61.8%) |
Female |
4 (15.4%) |
5 (19.2%) |
9 (34.6%) |
17 (65.4%) |
Age group: |
|
|
|
|
60 – 64 yrs |
3 (12.5%) |
5 (20.8%) |
8 (33.3%) |
16 (66.7%) |
65 – 69 yrs |
4 (21.1%) |
2 (10.5%) |
6 (31.6%) |
13 (68.4%) |
70 yrs & above |
3 (17.6%) |
5 (29.4%) |
8 (47.1%) |
9 (52.9%) |
Reliability and validity analysis
M-GDS-15, M-GDS-14
Item 9 of the M-GDS-15: "Do you prefer to stay at home, rather than going out and doing new things?" was poorly correlated with corrected item total score and had no discriminatory value against clinical diagnosis of both major depression and all clinically significant depression (Table 2, 3). Thus, a new scale was suggested by omitting the item 9 of M-GDS-15, leaving the other 14 items to form M-GDS-14. Further validity analyses were on the M-GDS-14.
Table 2. Internal Consistency & Test-retest Reliability for M-GDS-15 & M-GDS-14
|
M-GDS-15 |
M-GDS-14 |
||
|
Corrected Item-Total Correlation |
Alpha if Item Deleted |
Corrected Item-Total Correlation |
Alpha if Item Deleted |
Q1 |
0.36 |
0.83 |
0.37 |
0.84 |
Q2 |
0.29 |
0.83 |
0.30 |
0.84 |
Q3 |
0.54 |
0.81 |
0.53 |
0.83 |
Q4 |
0.63 |
0.81 |
0.64 |
0.82 |
Q5 |
0.50 |
0.82 |
0.49 |
0.83 |
Q6 |
0.42 |
0.82 |
0.44 |
0.84 |
Q7 |
0.57 |
0.81 |
0.59 |
0.83 |
Q8 |
0.42 |
0.82 |
0.41 |
0.84 |
Q9 |
0.09 |
0.84 |
- |
- |
Q10 |
0.63 |
0.80 |
0.64 |
0.82 |
Q11 |
0.45 |
0.82 |
0.45 |
0.84 |
Q12 |
0.57 |
0.82 |
0.54 |
0.83 |
Q13 |
0.53 |
0.82 |
0.54 |
0.83 |
Q14 |
0.40 |
0.82 |
0.42 |
0.84 |
Q15 |
0.41 |
0.82 |
0.42 |
0.84 |
Cronbach’s alpha |
0.83 |
0.84 |
||
Test-retest Reliability |
0.85* |
0.84* |
||
*Spearmen’s rho, correlation is significant at the 0.01 level (2 tailed)
Table 3. Percentage of positive responses on the individual items of the M-GDS-15
|
Major Depression |
All Clinically Significant Depression |
||||
Item |
Control (%) |
Cases (%) |
p value |
Control (%) |
Cases (%) |
p value |
1 |
6 |
40 |
0.01* |
3 |
27 |
0.008* |
2 |
58 |
100 |
0.01* |
53 |
86 |
0.008 |
3 |
26 |
80 |
0.002* |
16 |
68 |
<0.0005 |
4 |
14 |
80 |
<0.0005* |
8 |
55 |
<0.0005 |
5 |
20 |
80 |
0.001* |
16 |
55 |
0.002 |
6 |
44 |
100 |
0.001* |
37 |
82 |
0.001 |
7 |
28 |
100 |
<0.0005* |
21 |
73 |
<0.0005 |
8 |
52 |
100 |
0.004* |
42 |
91 |
<0.0005 |
9 |
66 |
80 |
0.5* (N.S.) |
71 |
64 |
0.6 (N.S.) |
10 |
32 |
90 |
0.001* |
21 |
77 |
<0.0005 |
11 |
4 |
40 |
0.005* |
3 |
23 |
0.02* |
12 |
28 |
90 |
<0.0005* |
21 |
68 |
<0.0005 |
13 |
44 |
100 |
0.001* |
32 |
91 |
<0.0005 |
14 |
14 |
70 |
0.001* |
13 |
41 |
0.01 |
15 |
46 |
80 |
0.08* (M.S.) |
37 |
77 |
0.003 |
Reliability
After omitting item 9 from M-GDS-15, all items in the newly formed scale, M-GDS-14, had satisfactory corrected item-total correlation, with Cronbach's alpha coefficient of 0.84 and test-retest reliability Spearman's Correlation Coefficient of 0.84 (Table 2).
Validity
Individual item versus clinical diagnosis
Positive response on item-15 (of M-GDS-15): "Do you think that most people are better off than you are?" was only marginally significantly associated with major depression, but significantly associated with all clinically significant depression (Table 3). All other items of the M-GDS-14 were significantly associated with both major depression and all clinically significant depression.
Total score of M-GDS-14 versus Clinical Diagnosis
The mean score of the M-GDS-14 in the non-depressed group, minor depression group and major depression group was 3.3 (SEM 0.3), 7.2 (SEM 0.5) and 11.0 (SEM 0.7) respectively. The difference of score mean between clinical depression groups was significant by Kruskal-Wallis test (H=38.38, p < 0.0005). Pairwise comparisons using Mann-Whitney U test showed that the subjects in major depression group and minor depression group both had significantly higher M-GDS-14 scores than the non-depressed group ( p < 0.0005 for both); the subjects in major depression group also had significant higher M-GDS-14 scores than the minor depression group ( p = 0.001). These findings supported M-GDS-14 as a valid measure of severity of depression.
Concurrent validity
The scores on M-GDS-14 and MADRS showed a good correlation, with Spearman's rho correlation coefficient of 0.68, significant at the level of 0.01 (2-tailed). Thirty subjects also administered the 30-items scale; their scores on the 30-items scale were also highly correlated with M-GDS-14, Spearman's rho 0.91, significant at the level of 0.01 (2-tailed). This indicated that the shorter version of scale is adequate substitute for the longer version.
The optimum cut off point
The optimum cut off points for major depression and all clinically significant depression was 7/8 and 5/6 respectively for M-GDS-14, as determined by the coordinates of the receiver operating characteristic curve. At the cut off point of 7/8, the M-GDS-14 has 100% sensitivity, 92.0% specificity, positive predictive value of 71.4% and negative predictive value of 100% in detecting major depression; and 95.5% sensitivity, 84.2% specificity, positive predictive value of 77.8% and negative predictive value of 97.0% at the cut off point of 5/6 in detecting all clinically significant depression (Figure 1, 2).
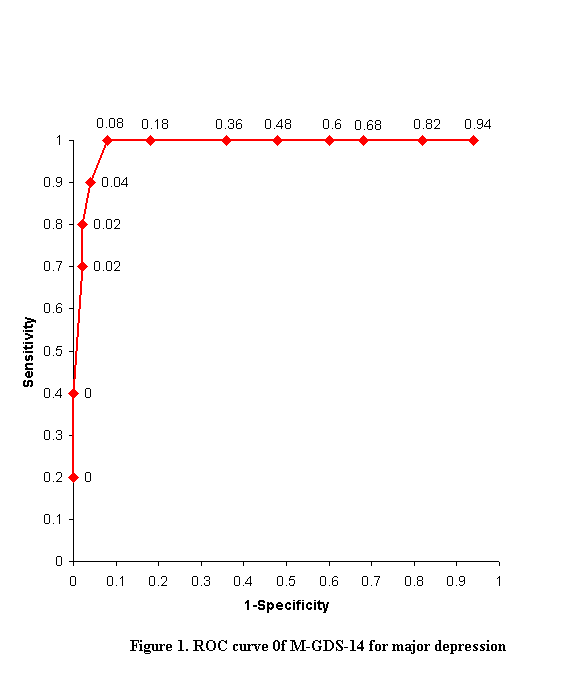
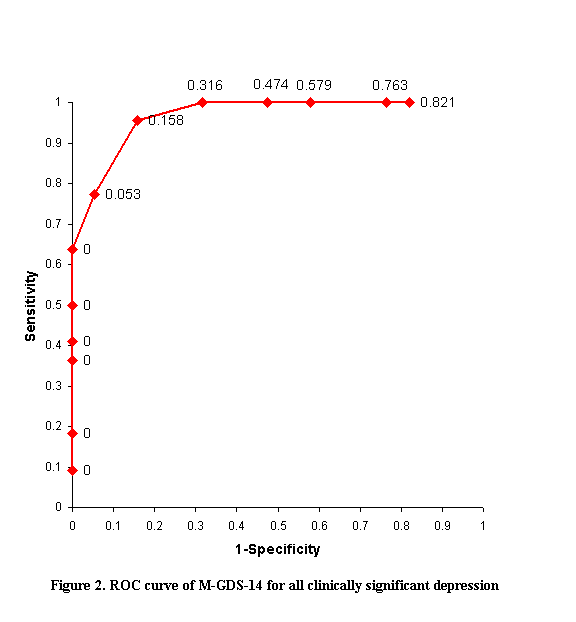
Do different genders score differently on M-GDS-14?
Thirty four males and 26 females participated in this validation study. There were no significant different in the score on M-GDS-14 by male or female subjects (Mann-Whitney U test: z = - 0.35, p = 0.73). There were also no difference in cut off points for both major depression and all clinically significant depression between male and female gender.
Discussion
This validation study found that the item-9 of GDS-15 ("Do you prefer to stay at home, rather than going out and doing new things?") had no discriminatory value in differentiating cases and non-cases of depression in our local context. This finding is probably due to the difference between the local cultures from the Western. The local cultures are relatively introvert and emphasis on family living than individual lifestyle. Thus, under the local culture, people has higher tendency to give positive response to the item, despite their depressive state. This is consistent with the findings of another local psychometric scale validation study, where Maniam found that the item-5 of General Health Questionnaire-30 ("Have you recently been getting out of house as much as usual?"), which shared the same theme with the item-9 of GDS-15, did not at all distinguish between cases and non-cases (Maniam, 1996).
By omitting the item-9, the newly form scale, M-GDS-14, has satisfactory reliability and validity as a screening scale for depression among physically ill elderly inpatients. The same cut-off point is applicable to both genders.
Although the great majority of subjects required someone to read out the scale items to them, during the administration (not fully self-administered), this is generally acceptable. In Cannon et al (2002), they reported a significant correlation between oral and written administrations of GDS among the higher cognitive functioning participants.
It should be noted that major depression was defined followed the DSM-IV criteria of Major Depressive Episode, instead of Major Depressive Disorder in this study. In such a way, if patients were in partial remission of the course of Major Depressive Disorder, they would not be classified as major depression, but probably minor depression.
Although 60 subjects had participated in the validation study and 22 were clinically significantly depressed, only 10 (16.7%) were major depression. This small number of positive case for major depression, thus the narrow variation of scores may have counted for the unexpected 100% sensitivity in detecting major depression at its optimum cut-off point.
Conclusion
The abbreviated version of GDS with 15 items when validated in Malaysian population results in 14 items with discriminatory values. This new Malay GDS-14 is as reliable and valid as its original 30 or 15 items versions.
Acknowledgements
This study was conducted with Short-term Intensification of Research in Priority Areas Grant from Universiti Sains Malaysia.
References:
Abas, M A, Philips, C, Carter, J, Walter, J, Banerjee, S, Levy, R. (1998) Culturally sensitive validation of screening questionnaires for depression in older African-Caribbean people living in south London. British Journal of Psychiatry. 173, 249 - 254.
Alden, D, Austin, C, Sturgeon, R. (1989) A correlation between the Geriatric Depression Scale long and short forms. Journal of Gerontology. 44, 124 - 125.
Allen-Burge, R, Storandt, M, Kinscherf, D A, Rubin, E H. (1994) Sex differences in the sensitivity of two self-report depressive scales in older depressed inpatients. Psychology & Aging. 9, 443 - 445.
Cannon, B J, Thaler, T, Roos, S. (2002) Oral versus written administration of the Geriatric Depression Scale. Aging & Mental Health. 6, 418 - 422.
Chen, P C Y, Andrews, G R, Josef, R, Chan, K E, Arokiasamy, J T. (1986) Health and aging in Malaysia - a study sponsored by the World Health Organization. Department of Social and Preventive Medicine, Faculty of Medicine, University of Malaya.
Covinsky, K E, Kahana, E, Chin, M H, Palmer, R M, Fortinsky R H, Landefeld, C S. (1999) Depressive symptoms and 3-year mortality in older hospitalized medical patients. Annals of Internal Medicine. 130, 563 - 569.
de Craen, A J, Heeren, T J, Gussekloo, J. (2003) Accuracy of the 15-item geriatric depression scale (GDS-15) in a community sample of the oldest old. International Journal of Geriatric Psychiatry. 18, 63 - 66.
D'Ath, P, Katona, P, Mullan, E, Evans, S, Katona, C. (1994) Screening, detection and management of depression in elderly primary care attenders I: The acceptability and performance of the 15 item Geriatric Depression Scale (GDS15) and the development of short versions. Family Practice. 11, 260 - 266.
Fountoulakis, K N, Tsolaki, M, Iacovides, A, Yesavage, J, O'Hara, R, Kazis, A, Ierodiakonou, C. (1999) The validation of the short form of the geriatric Depression Scale (GDS) in Greece. Aging-Clinical & Experimental Research. 11, 367 - 372.
Ganguli, M, Dube, S, Johnston, J M, Pandav, R, Chandra, V, Dodge, H H. (1999) Depressive symptoms, cognitive impairment and functional impairment in a rural elderly population in India: a Hindi version of the geriatric depression scale (GDS-H). International Journal of Geriatric Psychiatry. 14, 807 - 820.
Jackson, R, Baldwin, B. (1993) Detecting depression in elderly medically ill patients: the use of the GDS compared with medical and nursing observations. Age & Aging. 22, 319 - 353.
Karim, H A. (1997) The elderly in Malaysia: demographic trends. The Medical Journal of Malaysia. 52, 206 - 212.
Koenig, H G, Meador, K G, Cohen, H J, Blazer, D G. (1988) Self-rated depression scales and screening for major depression in the older hospitalized patient with medical illness. Journal of the American Geriatric Society. 36, 699 - 706.
Koenig, H G, Shelp, F, Goli V. (1989) Survival and health care utilization in elderly medical inpatients. Journal of the American Geriatric Society. 37, 599 - 606.
Krishnaswamy, S. (1997) Psychiatric problems among the elderly in Malaysia. The Medical Journal of Malaysia. 52, 222 - 225.
Lesher, E L, Berryhill, J S. (1994) Validation of the Geriatric depression Scale - short form among inpatients. Journal of Clinical Psychology. 50, 256 - 260.
Liu, C Y, Lu, C H, Yu, S, Yang, Y Y. (1998) Correlations between scores on Chinese versions of long and short forms of the Geriatric Depression Scale among elderly Chinese. Psychological Reports. 82, 211 - 214.
Maniam, T. (1996) Validation of the General Health Questionnaire (GHQ-30) for a Malaysian population. Malaysian Journal of Psychiatry. 4, 25 - 32.
Penninx, B W J H, Geerlings, S W, Deeg, D J H, van Ejik, J T M, van Tilburg, W, Beekman, A T M. (1999) Minor and major depression and the risk of death in older persons. Archives of General Psychiatry. 56, 889 - 895.
Rapp, S R, Walsh, D A, Parisi, S A, Wallace, C E. (1988) Detecting depression in elderly medical inpatients. Journal of Consulting and Clinical Psychology. 56, 509 - 513.
Sheikh, J A, Yesavage, J A. (1986) Geriatric Depression Scale (GDS): recent findings and development of a shorter version. In: Brink, T L. (ed.) Clinical Gerontology: A guide to assessment and intervention. New York, Howarth Press.
Yesavage, J A, Brink, T L, Rose, T L, Lum, O, Huang, V, Adey, M, Leirer, V O. (1983) Development and validation of a geriatric depression screening scale: a preliminary report. Journal of Psychiatric Research. 17, 37 - 49.
First Published September 2004
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


