Browse through our Journals...
Scalp dissecting cellulitis
Kendall Lane MD, LT, MC, USN
A 27 year-old Caucasian male presented with tender progressing fluctuant nodules and alopecia on his scalp for seven years. The lesions often oozed a serosanguinous discharge and bled occasionally. All cultures of the discharge were negative. He had been treated with courses of doxycycline, isotretinoin, and intralesional kenalog without significant improvement. A trial of oral steroids relieved the tenderness and reduced the discharge temporarily. Past medical history was significant for scarring acne on the face, multiple pilonidal cysts, and hidradenitis suppurativa. Family history was negative for any similar skin conditions. He was not taking any medications or supplements.
On examination, flesh-colored tender fluctuant nodules with scarring alopecia were noted on the scalp (Figure 1). The nodules formed intercommunicating sinuses that expressed a serosanguinous discharge when palpated. Deep pitting scars were seen on the face. Scars were noted in bilateral axillae and adjacent to the gluteal cleft from prior surgical incisions. Lymphadenopathy was absent. The remainder of the physical exam was unremarkable.
Figure 1
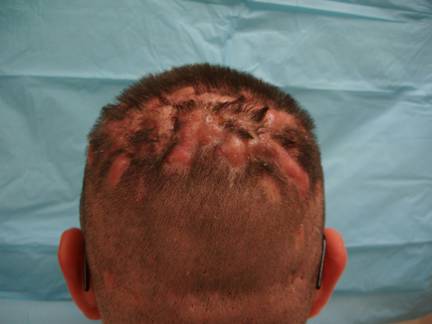
Diagnosis
Dissecting cellulitis as part of the follicular occlusion tetrad
About the condition
Dissecting cellulitis, also referred to as perifolliculitis capitis abscedens et suffodiens (PCAS) or Hoffman Disease, is a progressive chronic suppurative condition most commonly affecting African American males between the ages of 18 and 40 years old.1 Although less common, females and children can be affected.2, 3 The specific etiology of this uncommon condition is unknown, but the mechanism is thought to be due to follicular blockage or occlusion.1 Sebaceous material accumulates and causes dilation and rupture of the follicle resulting in a localized neutrophilic and granulomatous response. Secondary bacterial infection can occur, but it is not the primary cause.
The condition begins with simple folliculitis on the scalp progressing to perifollicular pustules, fluctuant nodules, and sinus tract formation. Alopecia initially begins as telogen effluvium secondary to inflammation and then progresses to patchy scarring alopecia. Regional lymphadenopathy is characteristically absent, unless a secondary infection is present. Serosanguinous or seropurulent fluid may be expressed from the nodules. Culture of the discharge is typically negative.
Although spondyloarthorpathy has been reported, most patients do not have systemic symptoms or disease. Osteomyelitis of the skull and squamous cell carcinoma can rarely occur in patients with dissecting cellulitis.
On histological examination, early lesions will show dense neutrophilic, lymphocytic, histiocytic, and plasma cell infiltrates. Abscesses may be seen in the dermis and subcutaneous tissue. Granulomas, foreign body giant cells, scarring, and fibrosis may be seen later in the disease process.
Dissecting cellulitis is considered to be a part of a follicular occlusion tetrad. Patients with the tetrad present with scarring acne conblogata, pilonidal cysts, hidradenitis suppurativa, and dissecting cellulitis. This patient had all four components of the tetrad.
Clinically, dissecting cellulitis can mimic acne keloidalis nuchae, pseudopelade of Brocq, tinea capitis, tufted folliculitis, and discoid lupus erythematous. Table 1 lists the differential diagnosis for dissecting cellulitis with the defining clinical characteristics and treatments included.
Condition |
Characteristics |
Treatment |
Dissecting cellulitis |
Tender nodules and sinus tracts on scalp Serosanguinous drainage LAD absent KOH negative Culture negative for bacterial or fungal Elements May be seen as part of follicular occlusion tetrad |
Isotretinoin Antibiotics Oral steroids Surgery Laser |
Tinea Capitis Kerion |
Tender nodules with drainage KOH positive Culture positive fungal elements LAD present Fever? Elevated WBC? |
Oral antifungals |
Folliculitis |
Pustules involving hair follicle with Surrounding erythema |
Oral antibiotics |
Acne keloidalis nuchae |
Papules and nodules on nape of neck Secondary to acne Young black males |
Oral antibiotics Topical retinoids |
Discoid lupus erythematosus |
Flat-topped firm scaly plaques Follicular plugging females |
Sunscreen Topical or Intralesional kenalog antimalarials Immunosupressive agents |
Pseudopelade of Brocq |
Scarring alopecia Minimal inflammation Dermal atrophy causing "footprints in the snow” sign mild erythema and slight perifollicular scaling
|
No treatment |
Tufted hair folliculitis |
Rare progressive scarring alopecia 10-15 hairs emerging from a single follicular opening |
Tar shampoo Oral antibiotics |
Table 1: Differential Diagnosis
Dissecting cellulitis is a difficult condition to treat. Medical therapies include antibiotic soaps (chlorohexidine and benzoyl peroxide), dapsone, intralesional kenalog, zinc supplements,8 topical and oral isotretinoin, oral antibiotics (tetracycline and doxycycline), and oral steroids.1,4 Of these, an extended course of oral isotretinoin appears to be the most effective therapy.1 CO2, 800nm, long-pulse non-Q-switched ruby, and long-pulsed Nd:YAG lasers have been used with variable success.9-12 Although reported as being effective, x-ray therapy is not routinely used because of undesirable side effects including skin cancer.1,4 However, in 2005, Chinnaiyan et al reported the use of modern external beam radiation to successfully treat refractory dissecting cellulitis without long-term complications.13 More commonly, surgical methods are used for severe and intractable cases. Simple incision and drainage and wide excision with split-thickness skin grafting have been used to treat severe cases. Medical therapy is usually used first. If not responsive, the patient may benefit from more aggressive destructive or surgical therapies. Patients with dissecting cellulitis typically benefit from early dermatology consultation.
The patient described above is currently awaiting dermatology evaluation for surgical treatment. He has failed multiple medical therapies.
In addition to sending these patients to dermatology, the primary care provider should evaluate the lesions for secondary bacterial or fungal infections with culture and KOH preparation. Although rare, if osteomyelitis is suspected, a CT scan should be considered. A careful skin examination of the affected site should be preformed to identify squamous cell carcinomas, especially if previously treated with x-ray therapy.
Bibliography
Skibinska M, Schwartz R. Perifolliculitis capitis abscedens et suffodiens. Accessed July 16, 2007 at: http://www.emedicine.com/derm/topic625.htm.
Ramesh V. Dissecting cellulitis of the scalp in 2 girls. Dermatologica 1990;180:48-50.
Unal S, Unal S, Kuyucu S, Kuyucu N. Dissecting cellulitis of the scalp: A case report. International Pediatrics 2004;19(2):203-5.
Scheinfeld NS. A case of dissecting cellulitis and a review of the literature. Dermatol Online J 2003;9(1):8.
Salim A, David J, Holder J. Dissecting cellulitis of the scalp with associated spondylarthropathy: case report and review. J Eur Acad Dermatol Venereol 2003;17(6):689–691.
Ramasastry ss, Granick MS, Boyd JB, Furrell JW. Severe perifolliculitis capitis with osteomyelitis. Ann Plat Surg 1987;18:241-244.
Curry SS, Gaither DH, King EL. Squamous cell carcinoma arising in dissecting cellulitis of the scalp: a case report and review of secondary squamous cell carcinomas. J Am Acad Dermatol 1981;4:673-678.
Kobayashi H, Aiba S, Tagami H. Successful treatment of dissecting cellulitis and acne conglobata with oral zinc. Br J Dermatol 1999;141:1137-8.
Glass LF, Berman B, Laub D. Treatment of perifolliculitis capitis abscedens et suffodiens with the carbon dioxide laser. J Dermatol Surg Oncol 1989; 15:673-676.
Boyd A, Binhlam J. Use of an 800-nm pulsed-diode laser in the treatment recalcitrant dissecting cellulitis of the scalp. Arch Dermatol 2002;138(10):1291-3.
Chui CT, Berger TG, Price VH, Zachary CB. Recalcitrant scarring follicular disorders treated by laser-assisted hair removal: a preliminary report. Dermatol Surg 1999;25(1):34-7.
Krasner B, Hamzavi F, Murakawa G, Hamzavi I. Dissecting cellulitis treated with the long-pulsed Nd:YAG laser. Dermatol Surg 2006;32(8):1039–44.
Chinnaiyan P, Tena L, Brenner M, Welsh J. Modern external beam radiation therapy for refractory dissecting cellulitis of the scalp. Br J of Dermatol 2005:152(4):777-9.
Callen J. Lupus Erythematosus, discoid. Accessed July 21, 2007 at: http://www.emedicine.com/DERM/topic247.htm.
Sperling L. Pseudopelade, Brocq. Accessed July 21, 2007 at: http://www.emedicine.com/derm/topic357.htm.
Hughes C. Tufted hair follicultis. Accessed July 21, 2007 at: http://www.emedicine.com/derm/topic439.htm.
Affiliations:
LT Lane is a physician in the United States Navy.
The views expressed in this article are those of the author and do not reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.
Copyright ©Priory Lodge Education Limited 2007
First Published August 2007
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


