|
|
Modified Dilatational
Tracheostomy |
K. Karvandian1, Z.
Hosainkhan1, S. A. Tabatabaee1, S. H. Abtahi1 & S.Nikou.
Department of Anesthesia and
Intensive Care Unit, Tehran University of Medical Science (TUMS), Tehran Iran
(Email:kassramail@yahoo.com)
Abstract
Traditional surgical tracheostomy has its
own risks, and complications, i.e. hemorrhage, directional deviation, tracheal
rupture, pneumothorax, hypoxia and death. The other method for tracheostomy-
Tracheostomy through skin- has contraindications agreed on by all specialists
as well. Difficulty in reaching to tracheal cartilages in ilatational tracheostomy deviation of tracheal direction and previous
manipulation due to tracheostomy are the reasons for not using the so-called
percutaneous tracheostomy method, as mentioned by several case reports. Keeping
in mind the difficulties and risks of the former method, a new method titled as Modified
Dilatational Tracheostomy has been applied by this team on four groups of patients whenever relative
contra-indications for percutaneous tracheostomy were the obstacle.
Introduction
“Percutaneous Dilatational Tracheostomy”
in spite of its vast application, faces usage limitations in some patients. 6
patients admitted In Intensive Care Unit (ICU) of Imam Khomeini teaching
Hospital, who were not suitable cases for usual percutaneous tracheostomy
method, beard a new method of tracheostomy to benefit from its advantages.
Relative counter-indications of percutaneous tracheostomy, present in these selected
patients, were as follows:
A- Having large
thyroid gland
B- Having short
neck
C- Limitation
of neck movement
D- Bearing
previous tracheostomy
In this new method, the patients were
anesthetized and given neuromuscular blockage in operation room, or in Intensive
Care Unit (ICU). After incision and exploration of soft tissue, cartilages were
reached and passed by, by the guide wire, instead of being incised as done in
the usual method. The tracheal tube was inserted after dilatation thereafter.
Case 1
The first patient was a 29-year old man,
with brain damage, in vegetative state. Three years ago, he had beard
tracheostomy in such condition (Figure 1). After relative improvement and
closure of the site of the previous tracheostomy, he had been discharged from
the hospital and received care at home. Pneumonia, respiratory distress and
homodynamic problems had lead him back to ICU for the second time. Critical
condition of the patient and prolonged intubation raised the need for
tracheostomy again, where a percutaneous one was contraindicated.
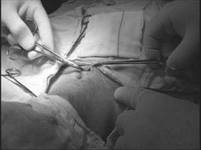
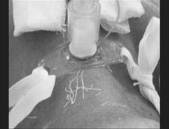
So, based on the new method, the soft
tissue in neck area, inferior to the site of previous tracheostomy, was opened
via a minimal skin incision. After reaching to the tracheal cartilages by use
of needle and dilator, the conductor wire was passed and dilatation was
performed by Griggs forceps (Figure 2). Then, a No.8 trcheostomy tube was
inserted in the trachea, with least hemorrhage. In mentioned procedure,
tracheal tube was pushed through the space between cartilages No.4 and 5 with minimal damage to the soft tissue and no damage to tracheal cartilages. That is to
say, this method bears the advantages of percutaneous tracheostomy such as
minimal hemorrhage, preservation of tracheal cartilages, rapidity, small size
of incision and high accuracy.
In subsequent follow-up by bronchoscope,
tracheal condition was investigated. After three days, the patient was
separated from ventilator. He was discharged after treatment of Pneumonia in a
good general condition.
Case 2
Our second patient was a 24-year old man
with a large thyroid gland; another relative contraindication for percutaneous
tracheostomy (Figure 3).He had undergone craniotomy due to brain hernia &
was a candidate for tracheostomy, on account of prolonged intubation and
decreased level of consciousness.
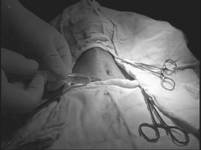
After incising the skin between cartilages
No. 2 & 3, the tracheal cartilages were reached by passing of conductor
wire. Dilatation by Griggs forceps was performed and a No.8 tracheostomy tube
was inserted (figure 4). After
relative improvement, the patient was discharged from ICU.
Case 3
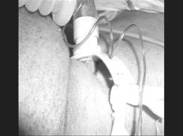
The third patient was a 29-year old man, a
case of multiple-trauma, with suspected cervical fracture, another relative
contraindication for percutaneous tracheostomy. He was also a candidate for
tracheostomy due to prolonged intubation and mechanical ventilation (Figure 5).
Using the modified tracheostomy method, after incision and definite access to
tracheal cartilage, the conductor wire was passed via the space between
cartilage No.2 & 3.Dilatation by Griggs forceps and insertion of a tracheal
tube No. 9 were the final steps.
Case 4
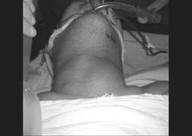
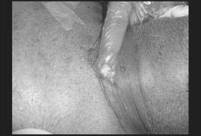
And our last patient was a 65-year old
man, with chronic bronchitis, broncho-esophageal fistula, and a short
neck. He beard general anesthesia
in operating room (Figure 6).
After bronchoscopic confirmation of
bronchial patency and bronchoesophegeal fistula, the patient was transferred to
ICU, but on the next day he died.
In post tracheostomy tracheal investigation, the cause of death was
found to be aspiration-induced acute respiratory failure. This patient's
condition was one of the relative contra indications of percutaneouse tracheostomy.
Discussion
The tracheostomy by surgical method which
has been used for so many years in ENT, Thorax surgery and Neurosurgery
Departments for treatment and training purposes, has covered a wide range of
patients with small modifications (9). It has also covered the sever cases as
well as usual ones, in a way that nearly no patient has been deprived from this
method (10).
Tracheostomy through skin was done by Ciaglia,in 1985 , not
welcomed then(11). In 1990,
Griggs dilatational tracheostomy method was initiated by Mr. Griggs and applied
worldwide, along with his self-designed forceps that is called after him.
(8).Nowadays, different methods of dilatational tracheostomy through skin
_including Griggs (1), Ciaglia(2), and Fantony(3)_ are being practiced for many
years by using advanced tools rather than the surgical method in many centers
around the world(Portex Co)(4). The main reasons to put forward the tracheostomy through skin in all
above mentioned methods are rapidity, precision and lesser complications in
both short and long terms (5). The methods have been compared to each other.
Among different methods of dilatational tracheostomy, some have advantages in
comparison to the others, considering the skill of specialists as the most
important factor (6). There are some limitations in this method, in spite of
presented advantages however. Some are as follows: ages less than 12 15 years, emergency setting,
hyperthyroidism, previous tracheosthomy, invasion of tumors to trachea and
neck, short neck, sever limitation of neck movements and neck injuries (7).
Dilatational tracheostomy through skin in
IRAN was performed first in Tehran University of medical science (TUMS) during
2005-2006 with cooperation of specialists from Turin University of medical
science _Maria Victoria Hospital, Turin ITALY _and representative of Portex Co
in IRAN (12). Along with the registration of this method, came the
responsibility of training the target groups throughout the country by
conducting different workshops in Imam Khomeini Hospital (12). In time, it was
beard in mind that there were groups _such as those with previous surgery in
the neck area, none-suitable anatomy or pathologies of the neck _who would
benefit from the mentioned method in case it could be performed on them as well. Not only were the conditions of these
groups, but also the two methods of tracheostomy assessed precisely by our
research team.The result was a new method, applicable to the mentioned groups.
Fortunately, the new method was practiced
successfully by our group with minimal complications.
In long term follow-up of the patients
with dilatational tracheostomy through skin, it was found that, the injuries to
tracheal cartilages were far less than the surgical tracheostomy; reason for
which is preserving the tracheal cartilages in this method by using the spaces
between tracheal cartilages.
For more precise assessment of the airways
in case of deviations, narrowing, previous tracheostomy, tracheomalacia and
stenosis, the fiber optic bronchoscope can be used. it will also be of help in
tracheal deviation due to hyperthyroidism and tracheal stenosis.
Even the malignant invasion to upper can
be excluded.
References
1-Griggs WM, Worthley
LIG,Gilligan JE, ThomasPD, Myburg JA:A simple percutaneous tracheostomy
technique. Surg Gynaecol Obstet 1990; 170:543-545.
2-Ciaglia P, Graniero KD. Percutaneous
dilatational tracheostomy. Chest. 1992;101:464–467
3-Fantoni A, Ripamonti D: Anon-derivative,
non-surgical tracheostomy:the translaryngeal method. Intensive Care Med
1997;23:386-392.
4.Leonard RC, Lewis RH, Singh B, van
Heerden PV: Late outcome from percutaneous tracheostomy using the Portex kit.
Chest 1999 Apr; 115(4): 1070-5
5. Cheng E, Fee WE Jr. Dilatational versus
standard tracheostomy: a meta-analysis. Ann Otol Rhinol Laryngol. 2000;109:803-807.
6.Current Opinion in Otolaryngology &
Head & Neck Surgery. 7(3):144, June 1999
7.Print ISSN: 0263-9319 Volume: 22 |
Issue: 8 Head and Neck Cover date: August 2004 Page(s): 194-195
8.Paran H, Butnaru G, Hass I, Afanasyv A,
Gutman M. Evaluation of a modified percutaneous tracheostomy technique without bronchoscopic guidance. Chest. 2004;126:868-871.
9.Tracheostomy in the intensive care unit.
Part 1: Indications, technique, management. Chest 1986;90:269-73.
10. Medical indications for tracheotomy.
Chest 1989;96:186-90.
11.Ciaglia P,
Firsching R, Syniec C. Elective percutaneous dilatational tracheostomy: a new
simple bedside procedure; preliminary report. Chest 1985; 87:715-719
12. Bulletin of Tehran University
of Medical Science.No.78.ISSN:1682-9212:51
.
 |
Click
on these buttons to visit our journals |
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |
Psychiatry
On-Line |
Dentistry
On-Line |
Vet
On-Line |
Chest
Medicine
On-Line |
GP
On-Line |
Pharmacy
On-Line |
Anaesthesia
On-Line |
Medicine
On-Line |
Family
Medical
Practice On-Line |
All pages copyright ©Priory
Lodge Education Ltd 1994-2006.
First Published November 2006





