Post-Partum management of women with Gestational Diabetes: an audit in a District General Hospital in the UK
Authors: (1) Indrajit Talapatra (MRCP): Speciality Doctor in Diabetes/Medicine, Royal Albert Edward Infirmary, Wigan WN12NN, UK
(2) Jane McAllister: Diabetes Specialist Nurse, Royal Albert Edward Infirmary, Wigan WN12NN, UK
(3) Ian Patrick Michael O’Connell (FRCP): Consultant in Diabetes/Medicine, Royal Albert Edward Infirmary, Wigan WN12NN, UK
Email Dr I Talapatra: indra_tala@hotmail.com
Introduction: Gestational diabetes (GDM) is defined as diabetes or any degree of glucose intolerance diagnosed or recognized for the first time in pregnancy. The criteria according to various guidelines following oral glucose tolerance test (OGTT) are summarized below:
Table1: Criteria for Gestational Diabetes (OGTT is undertaken between 24-28 weeks)
NICE (National Institute of Clinical Excellence) 2008 |
IADPSG (International Association of Diabetes and Pregnancy Study Group) 2010 |
SIGN (Scottish Intercollegiate Network) 2010 |
Fasting >7 mmol/l or 2 hour >11.1 mmol/l |
Fasting >5.1 mmol/l, 1 hour >10mmol/l or 2 hour > 8.5 mmol/l |
Fasting >5.1mmol/l, 1 hour >10 mmol/l or 2 hour > 8.5 mmol/l |
There is worsening of insulin resistance during gestation. Although Glucose tolerance returns to normal in the majority of women with gestational diabetes shortly after delivery, many studies have shown that there is an increased risk of developing diabetes in later life. One study from Denmark, which followed women for a median of six years, showed 34.4% women with GDM had abnormal glucose tolerance compared to 5.3% control women (1). A further study showed 32.8% women with GDM had glucose intolerance or diabetes at 3 months after delivery compared to 3.2% in a control group (2).
Gestational diabetes can have significant health impacts on mother and child, including a higher risk for pre-eclampsia and miscarriage in mothers and shoulder dystocia, large for gestational age and macrosomia in babies and an increased risk of type 2 diabetes in mothers and children. In fact, women with gestational diabetes have a 35-60% chance of getting type 2 diabetes within 10-20 years post-partum (3). Despite these alarming statistics, a 2011 study published in Obstetrics and Gynaecology showed that only 68% of pregnant women got screened for gestational diabetes and only 19% of women diagnosed with GDM got screened post-partum (3). A federal task force recently issued a recommendation that all pregnant women get screened for GDM, regardless of risk factors, consistent with ACOG (American Clinical Obstetrics and Gynaecology guidelines).
The Risk Factors for development of diabetes in later life in women with gestational diabetes are summarized below (4)
Antepartum factors |
Postpartum factors |
High fasting glucose |
High fasting glucose on postpartum OGTT |
High glucose post-carbohydrate |
High glucose at 2 hours on postpartum OGTT |
Early Gestational age at diagnosis of GDM |
Increasing maternal age |
High maternal BMI at booking |
Maternal weight gain following pregnancy |
Previous history of GDM |
Additional pregnancy |
Insulin treatment during pregnancy |
|
|
|
Aim of the audit : To find out if women who had gestational diabetes were managed appropriately postpartum.
Methods: Case notes of the patients with gestational diabetes who were supposed to attend for OGTT and the postpartum clinic between 1st January 2014 and 31st March 2014 were studied
Criteria : Guidelines of NICE(National Institute of Clinical Excellence), Diabetes Prevention Programme Research Group and those outlined in Diabetes in Pregnancy, Oxford Diabetes Library, 2012 were taken into account:
NICE GUIDELINES, March 2008 (5):
- Women who have been diagnosed with gestational diabetes should discontinue hypoglycaemic treatment immediately after birth
- Women who were diagnosed with gestational diabetes should have their blood glucose tested to exclude persisting hyperglycaemia before they are transferred to community care.
- Women who were diagnosed with gestational diabetes should be reminded of the symptoms of hyperglycaemia.
- Women who were diagnosed with gestational diabetes should be offered lifestyle advice (including weight control, diet and exercise) and offered a fasting plasma glucose measurement (but not an OGTT) at the 6-week post natal check and annually thereafter.
- Women who were diagnosed with gestational diabetes (including those with ongoing impaired glucose regulation) should be informed about the risks of gestational diabetes in future
Criteria used for the audit:
- Stop insulin following delivery
- Check occasional blood glucose
- If pre-meal blood glucose is > 8 mmol/l consider metformin (6)
- Support and encourage breastfeeding. Education regarding breastfeeding should be given before delivery and support following the birth to facilitate breastfeeding. Breast feeding is associated with reduced risk of childhood obesity (7). Also in women it reduces future rates of diabetes (8, 9)
- Advised woman of increased risk of later diabetes
- Advice regarding diet and exercise
- Advice regarding planning of future pregnancy and have glucose test before conception. Women should be advised about the importance of planning future pregnancies, maintaining good glycaemic control in early pregnancy, using folic acid supplements, avoiding potentially teratogenic agents and weight management. Women with GDM should be advised to have a glucose assessment before conception
- Discuss options for effective contraception. It should be mentioned that there is no risk of later diabetes with the use of combined oral contraceptive agents in women with previous GDM women (10). However, those who are parous, older and at risk of endometrial cancer may benefit from Mirena IUD.
- Arrange OGTT or FPG at 6 weeks NICE guidelines recommend measurement of fasting plasma glucose at 6 weeks and then annually to exclude glucose intolerance or diabetes (5). However, studies have shown measurement of FPG alone rather than an OGTT would miss 38-72% of cases of glucose intolerance in women with GDM (11, 12)
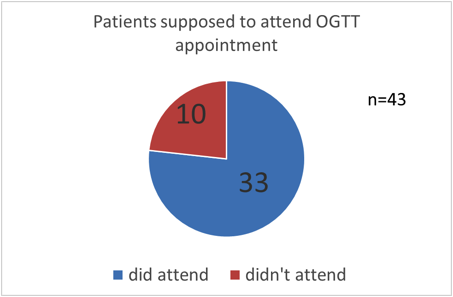
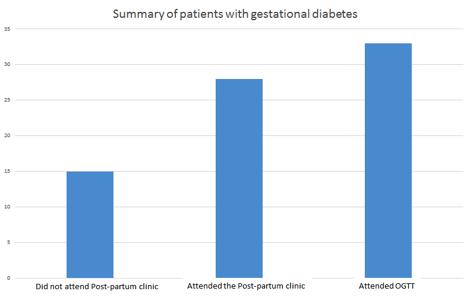
Results: (1) No. of patients with gestational diabetes who were supposed to attend for OGTT between 1st January 2014 and March 31stMarch 2014: 43
(2) No of patients who actually attended the OGTT appointments (6 weeks after delivery): 33
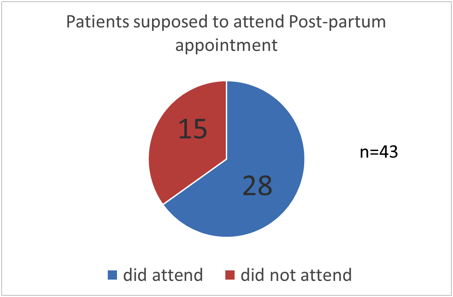
(3) No of patients who attended the Post-partum clinic 1 week after OGTT: 28
Reasons: In 3 patients reasons were not known, 1 patient had no follow up appointment made and in 1 patient there was delay in follow up appointment (required clinical review prior to this)
(4) For the patients who had not attended, whether a letter of suggestions for glucose surveillance was generated to the GP (General Practitioner) with a letter also to the patient outlining: (1) need for post natal check, (11) need for annual surveillance; the patients were asked to take the initiative and access GPs for it, (111) access to diabetes team in future pregnancy, (1V) access to pre-conception clinic should diabetes develop in the interim.
Results (April 2014): 7 outstanding GP letters from DNAs (one of which was a ‘lost’ patient and in another patient there was delay in post natal OGTT);
3 outstanding patient letters from DNAs (those who did not attend).
Results for those who attended the post natal clinic (28 out of 43 or 64%):
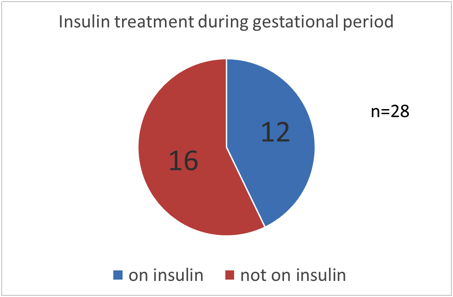
No of patients on insulin and has the insulin been stopped?
|
12 out of 28 (43%); insulin discarded following delivery in all 12 patients (100%) |
Has the glucose been tested a few times following delivery?
|
None The advice to patients to routinely do capillary blood glucose a few times following delivery is not given in our Trust. Only if they get the signs and symptoms of hyperglycaemia, they are asked to do the test |
How many had pre-meal glucose >8.0 mmol/l and of them how many were again put on metformin?
|
Nil recorded |
Whether breast feeding was encouraged
|
100%; also it is our hospital policy to strongly encourage and support breast feeding |
Whether advice was given regarding diet and exercise
|
100% Referral was done to dietician in pregnancy and again advice was given at post natal review |
Advice on contraception
|
100% |
Advice given to plan future pregnancy and have glucose test before conception
|
Advised annual surveillance with the GPs-100%. The patients are asked to approach the GPs themselves. (However this does not always happen, as we had seen patients in the past presenting with gestational diabetes during subsequent pregnancies but had no annual surveillance with their GPs despite having gestational diabetes in their former pregnancies) |
OGTT / FPG (fasting plasma glucose) and HbA1c (Glycosylated haemoglobin) advised again in a year
|
OGTT advised (or FPG with HbA1c)- 100% Annual FPG and HbA1c advised as alternate, if indicated by the patients’ original OGTT in pregnancy and their blood sugar pattern – i.e. if the patients had positive OGTT on the fasting value only and their pattern of home blood glucose monitoring showed high pre- breakfast blood glucose only on day to day tests then a FPG/HbA1c may be the recommended in a year’s time |
Advice on increased risk of diabetes in later life |
100% |
Summary:
- More than 1/3 of patients with gestational diabetes did not attend the post natal clinic
- All patients who were put on insulin during gestation stopped their insulin following delivery
- Patients did not check their capillary blood glucose routinely following delivery as they were not advised
- Advice with regard to diet, exercise, breast feeding and contraception were given in all patients
- Advice with regard to annual surveillance was given to all patients. However this does not always happen
- All patients were made aware of the increased risk of future diabetes
- OGTT (or FPG with HbA1c) after 1 year were advised in all patients
Suggestions:
- Patients with gestational diabetes should all be properly motivated to have OGTT after 6 weeks and attend post natal clinic 1 week thereafter
- All patients who do not attend their post natal appointment should be sent letters immediately
- All patients should ideally be advised to check their capillary blood glucose a few times after delivery
- Patients should be properly motivated to have their annual surveillance with their GPs and the GPs should be informed accordingly
- Instead of just fasting blood glucose (as recommended in NICE Guidelines) we should possibly continue to do OGTT 6 weeks post natal and OGTT (or FPG with HbA1c) after 1 year as we have been doing now.
Conclusions:
We aim to carry on doing ourselves or asking the GPs to do OGTT 6 weeks postpartum and OGTT or fasting plasma glucose with HbA1c 1 year thereafter to detect in future more cases of impaired glucose tolerance or diabetes.
The only goal of post-natal surveillance is not just to diagnose postnatal diabetes but will be to highlight to well-motivated women who have recent experience of a heritable tendency to diabetes that they can influence their own glucose metabolism, and that of their fledgling families. By highlighting IGT in the substantial proportion of women to whom this pertains, we hand them the power and responsibility to alter their own life style, activity levels and diet and of their families as well to prevent onset of future diabetes.
References:
- Damm P, Kuhl P, Bertelsel A, Molsted-Pedersen L (1992). Predictive factors for the development of diabetes in women with previous gestational diabetes. Am J Obstet Gynecol. 167, 607-616
- Retnakaran R, Qi Y, Sermer M, Connelly PW, Hanley AJ, Zinman B (2008). Glucose intolerance in pregnancy and future risk of pre-diabetes or diabetes. Diabetes Care. 31, 2026-2031
- Support the Gestational Diabetes Act of 2013. The American Congress of Obstetricians and Gynaecologists (March 2014); https://www.acog.org/~/media/Departments/Government%20Relations%20and%20Outreach/2014CLCGEDIAsk.pdf?dmc=1&ts=20140226T0950278506
- Temple R, 2012. In: Robert S. Lindsay ed. Risk factors for development of diabetes in later life in women with gestational diabetes. Oxford Diabetes Library. Diabetes in Pregnancy. UK: Oxford University Press, 78
- NICE Guidelines, Sec 1.6 (2008). Diabetes in pregnancy: Management of diabetes and its complications from pre-conception to the postnatal period; http://www.nice.org.uk/guidance/cg63/chapter/guidance
- Temple R, 2012. In: Robert S. Lindsay ed. Postpartum management of women with gestational diabetes. Oxford Diabetes Library. Diabetes in Pregnancy. UK: Oxford University Press, 74
- Hummel S, Pfluger M, Kreichauf S, Hummel M, Ziegler AG (2009). Predictors of overweight during childhood in offspring of parents with type 1 diabetes. Diabetes Care. 32, 921-925
- Steube AM, Richard-Edwards JW, Willett WC, Manson J, Michels KB (2005). Duration of lactation and incidence of type 2 diabetes. JAMA, 2601-2610
- Steube AM, Michels KB, Willett WC, Manson JE, Rexrode K, Rich-Edwards JW (2009). Duration of lactation and incidence of myocardial infarction in middle to late adulthood Am J Obstet Gynecol . 200, 138e1-138e8.
- Kjos SL, Shoupe D, Douyan S, Freidman RL, Bernstein GS, Mestman JH, Mishell DR Jr ((1998). Contraception and the risk of type 2 diabetes mellitus in Latin women with prior gestational diabetes. Am J Med Assoc. 280, 533-538
- Kwong S, Mitchell RS, Senior PA, Chick CL (2009). Postpartum diabetes screening: adherence rate and the performance of fasting glucose versus oral glucose tolerance test. Diabetes Care. 32, 2242-2244
- Ferrara A, Peng T, Kim C (2009). Trends in Postpartum diabetes screening and subsequent diabetes and impaired fasting glucose among women with histories of gestational diabetes mellitus: A report from the Translating Research into Action for Diabetes (TRIAD) study. Diabetes Care 32, 269-274
Declaration: This article is not under consideration for publication in any other journal. All the three authors contributed towards the preparation of the audit.
Conflict of Interests: None
We did not receive any grant from any Medical Company for preparation of the audit.
Copyright Priory Lodge Education Liited 2014 -
First Published August 2014
All pages copyright ©Priory Lodge Education Ltd 1994-


