Case report : pineal metastasis from lung cancer
First Published 17th June 2005
Dr. K.W. Lam1 MRCS ,
Dr F C Cheung 2FRCS , FHKAM ,
Dr K M Ko 1 FRCS , FHKAM
Department of Cardiothoracic Surgery1 ,
Department of Neurosurgery 2,
Queen Elizabeth Hospital,
30 Gascoigne Road, Hong Kong.
Correspondence : Dr K.W. Lam , fax : 00852- 2958-5673 ,
email : pkwlam1@yahoo.com
Department of Cardiothoracic Surgery,
Queen Elizabeth Hospital ,
30 Gascoigne Road, Kowloon, Hong Kong
Running Title
Metastasis to the pineal gland from carcinoma of lung are rare.2 This is a case report of a 57 year old lady presented with progressive diplopia, nausea and headache. CT brain revealed pineal metastasis from lung cancer with evidence of hydrocephalus. PET scan reviewed primary lung tumor in the right hilar region and presence of diffuse metastasis in multiple lymph node and bone. 5 year survival in patients with lung cancer stage M1 disease, according to International System for Staging Lung Cancer 7, was expected to be around 1%. Glucorticoid and external whole brain radiotherapy increased the median survival from one month up to six months.10
Abstract
Metastasis to the pineal gland from carcinoma of lung are rare.2 This is a case report of a 57 year old lady with multinodular goiter, presented with 2 months' history of progressive diplopia, nausea and headache. CT brain revealed pineal metastasis from lung cancer with evidence of hydrocephalus. Emergency CSF diversion surgery (ventriculoperitoneal shunt, VPS) had been carried out to relieve the hydrocephalus. Debulking of the tumor by stereotactic surgery (X-knife) was, subsequently performed. Metastastic adenocarcinoma was confirmed histologically by endoscopic ultrasound guided aspiration of her supra-clavicular lymph node. PET scan reviewed primary lung tumor in the right hilar region and the presence of diffuse metastasis in multiple lymph node and bone. She received external whole brain radiotherapy , WRBT (53.4 Gy) and was followed up in out-patient clinic.
5 year survival in patients with lung cancer stage M1 disease, according to International System for Staging Lung Cancer 7, was expected to be around 1%. Glucorticoid and external whole brain radiotherapy increased the median survival from one month up to six months.10
Keywords : lung cancer, pineal metastasis, staging, survival
Introduction
Pineal region tumors make up 0.4-1.0% of intracranial tumors in adults.3Central nervous system metastases occur in less than 3% of all asymptomatic lung cancer patients. 2 Metastasis from carcinoma of lung to the pineal gland are rare.2
When present, the features of diplopia associated with headache, nausea and vomiting and papilloedema (on fundal examination), one should point to the diagnosis of increase intracranial pressure. Brain masses (eg tumor, metastasis) should be part of the differential diagnosis. If left untreated, aqueductal compression with hydrocephalus may progressed to lethargy, obtundation, and death.4
There had been relatively few reports on this type of metastasis offering discussion of diagnosis and treatment modalities. 4
Case report
A 57 year old lady has history of multinodular goiter, presented with 2 months history of dizziness, headache and vomiting. A month later, she complained of progressive worsening of diplopia.
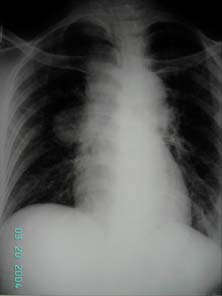
Figure 1 CXR showing right hilar
s
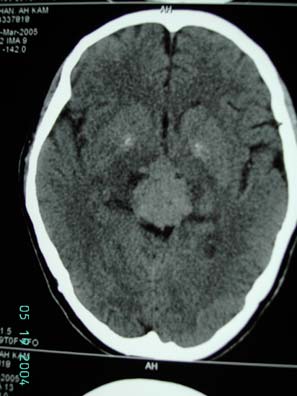
Figure 2 CT scan showed 32x28x26 mm hyperdense mass homogenous contrast enhancing solid mass over midline above mi dlin e causi ng obstructive hydrocephalu
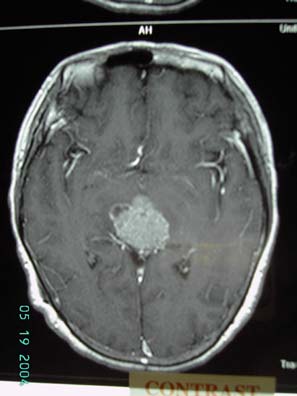
Figure 3 MRI scan showing mass in pineal region enhanced in T2 images with mass effect
On examination, pupil size were unequal, 3mm (right) and 2mm (left) and fundal examination revealed bilateral papilloedema. Multiple cervical lymph nodes were palpable on the right side. Neurological examination were otherwise unremarkable. Glascow coma scale was 15/15. Tumor markers including serum human chorionic gondaotrophin (ßHCG), alpha-fetoprotein (AFP), carcino-embrogenic antigen (CEA) were within normal ranges. Chest XR showed right hilar mass.(figure 1) CT scan of brain showed a 32 x28 x 26 mm hyperdense homogenous contrast enhancing solid mass crossing over the midline causing obstructive hydrocephalus. There was no evidence of tumor invasion into third ventricle or cerebellar vermis. (figure 2)
Emergency ventriculo-peritoneal (VP) shunting for CSF diversion and relief of hydrocephalus was carried out.
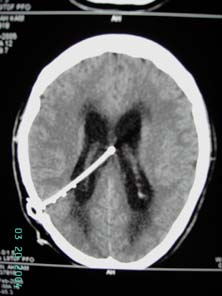
Figure 4 post-op CT brain showing decompression of ventricules with ventriculo-peritoneal shunt in situ
Endoscopic ultrasound guided aspiration to supraclavicular lymph node confirmed metastatic adenocarcinoma, spread from her primary lung cancer. Her visual symptoms persisted post-operatively. Stereotactic surgery (X-knife) was performed for debulking of the tumor mass.
18-FDG Whole body PET scan showed increase FDG uptake in multiple areas including the pineal area (SUVmax 9.4), soft tissue mass in the right hilar (SUVmax 10.8), several enlarged lymph nodes right paratracheal, precarinal (both with SUVmax 9), right supraclavicular fossa (SUVmax 5) and subcarinal area (SUVmax 4.7). A 9mm lytic lesion is noted at S2 vertebral body with increase FDG uptake, features suspicious of bony secondary.
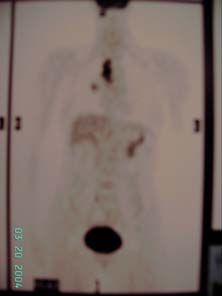
figure 5

figure 6
Figure 5 and 6, F18-FDG whole body PET scan report : hyperdense mass with increased FDG activitiy seen at the pineal area is suggestive of primary or secondary brain tumor. In the chest, with marked FDG uptake is compatible with primary malignant lung tumor. Multiple lymph node metastases including right paratracheal, precarinal and right supraclavicular lymph nodes. Suspicious of bony secondary to S2 vertebral body
No curative nor palliative surgery had been offered by the cardiothoracic surgical team, as stage IV (distant metastases) disease are considered inoperable.9. She subsequently undergone WBRT (53.4Gy) and was followed up in out-patient clinic.
Discussion
Metastatic brain tumors occur more frequently than primary brain tumors 10 but metastasis from lung carcinoma to pineal gland are rare.2,11
18 FDG-PET offers a rapid method for whole-body imaging that identifies systemic metastatic disease effectively and in assisting those who are suitable for curative surgery, also used for radiotherapy planning. 5 Negative PET scans can exclude metastatic disease suggested by CT scans with a reported 1% false negative rate. 2
However, because of the high metabolic rate of normal brain tissue, PET is extremely poor at detecting cerebral metastases, with a sensitivity of only 60%. 2 High - resolution MRI with gadolinium is necessary in the evaluation of pineal region lesions. Tumor characteristics (eg. size, vascularity, and homogeneity) and its anatomic relationship with surrounding structures, can be assessed. 4
"Synchronous" brain metastasis had been defined as lesions detected within 2 months of the primary diagnosis of related cancer and those with an unknown primary or newly diagnosed brain tumor with which the primary was unknown. This had been associated with a poor prognosis with a survival of 9 14 months. 6
According to International System for Staging Lung Cancer 7 ,this patient has (cT2, tumor status) with tumor size greater than 3cm in the greatest dimension, N3 (nodal status) with evidence of supra-clavicular lymph node metastasis and M1 (metastasis status) with the presence of distant metastasis (S2 vertebrae). 5 year survival in these patients with M1 were were expected to be around 1%.
The main treatment goals for patients with brain metastases in this region include relief of neurological symptoms, as in our case, with CSF diversion for relief of hydrocephalus, and long-term control of the tumor.
Although there have been no prospective randomized studiescomparing stereotactic surgery (SRS) and external beam whole brain radiation therapy (WBRT) to WBRT alone, there have been numerous large retrospective series reporting a significant survival benefit from SRS. Glucocorticoids and WBRT comprise the current standard of care and increase median survival from one month to three to six months. 10
However, the presence of VPS is believed to facilitate extraneural metastasis of the intracranial metastasis. 13 Re-irradiation and chemotherapy may have a limited role in patients with multiple recurrent metastases. 12
References :
1) DeAngleis LM, Posner JB, Neurological complications of cancer , Chp 143 pp2251-70
2) Kent MS, Jeffrey LP et al , Current state of imaging for lung cancer staging, Thoracic Surgical Clinic 14 (2004) 1 13
3) Jeffrey Bruce, Pineal Tumors, eMedicine Specialties, Neurosurgery, Kakita A, Kobayashi K, Aoki N, Eguchi I, Morita T, Takahashi H. Neuropathology. 2003 Mar; 23(1):57-60. Lung carcinoma metastasis presenting as a pineal region tumor
4) Jeffrey Bruce, MD, Pineal Tumors, eMedicine Specialties > Neurosurgery , section 1-11
5) Goldsmith SJ et al, Journal of Thoracic Surgical clinic 14 (2004) 95 112
6) Thomas AJ, Rock JP et al, Survival of patients with synchronous brain metastases: an epidemiological study in southeastern Michigan, Neurosurg Focus Preview: J Neurosurg 93:December 2000
7) CF Mountain, Revision in International System for Staging Lung Cancer, Chest Vol 111, 1710-17, 1997
8) Kavitha Vadde, MD, Alan J. Fischman, MD PhD, Whole Body FDG PET andStaging of Non-Small-Cell Lung Cancer, Joint Program in Nuclear Medicine, January 18, 2000
9) G J M Herder et al , Practice, efficacy and cost of staging suspected non-small cell lung cancer: a retrospective study in two Dutch hospitals, Thorax 2002;57:11-14
10) Official Title: A Prospective, Randomized Trial Comparing Surgery Versus Radiosurgery for the Treatment of Metastatic Brain Tumors, National Institute of Neurological Disorders and Stroke (NINDS)
11) Keyaki A et al, Pineal metastatic tumor from lung cancer initially caused by neurological abnormalities of pineal body tumor Curr Treat Options Oncol. 2000 Dec;1(5):447-58
12) Wen PY, Loeffler, Brain metastases. JS.Rev Neurol (Paris).1992;148(6-7):477-87
13) Poon TK et al, Extraneural metastasis of pineal germinoma via VP shunt, Ann Coll Surg HK (2004) 8, 153-5
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages copyright ©Priory Lodge Education Ltd 1994-

