Cigarette Smoking and Weight Loss in Nursing Home Residents
Margaret-Mary G. Wilson, MD,MRCP
Assistant Professor
Division of Geriatric Medicine,
Saint Louis University
Shahnaz Habib MBBS,
Clinical research assistant
Division of Geriatric Medicine,
Saint Louis University
Carolyn Philpot CGNP
Clinical Nurse Practitioner
Division of Geriatric Medicine,
Saint Louis University
Corresponding Author:
Margaret-Mary G. Wilson MD, MRCP
Division of Geriatric Medicine,
St Louis University Health Sciences Center,
1402, S. Grand Blvd, Rm M238,
St. Louis, MO 63104.
Tel No.: (314) 577-8462.
Fax No: (314) 771-8575.
E-mail: wilsonmg@slu.edu
Key words: Smoking, weight loss, aging, Long-term care
OBJECTIVE:
To evaluate body weight trends of elderly smokers following admission into a Long Term Care Facility.
STUDY DESIGN AND POPULATION:
Cross-sectional survey of 88 nursing home residents with six month follow-up.
MAIN OUTCOME MEASURES:
Fifty-one of 88 residents were included in the study.
Body weight, height, body mass index (BMI) and serum albumin were documented
on admission into the nursing home. Data collection was repeated at monthly
intervals over a six-month period.
RESULTS: The study population comprised 17(8M, 9F) smokers and 34(19M, 15F)
non-smokers. Smokers had a lower body mass index on admission compared with
non-smokers (24.2"3 and 27.4"9 respectively; p=0.04; Odds ratio [95%
CI] for smokers versus non-smokers = 1.629 [0.498 to 5.32] ).Twelve (71%) smokers
and 20 (59%) non-smokers gained weight (p=0.2). Four (24%) smokers and 12 (35%)
non-smokers lost weight (p=0.3). Smokers who lost weight did so at a faster
rate than non-smokers (13.3 "3.8 lbs and 7.8"2.4 lbs respectively
over six months; p=0.02). Similarly, weight gain occurred at a slower rate in
smokers compared with non-smokers (5.6"1.3lbs and 8.2lbs respectively over
six months; p=0.004)
CONCLUSIONS:
Weight loss in cigarette smokers may occur at a more rapid in residents who smoke compared with non-smokers. Similarly, weight gain occurs at a slower rate in smokers. Smoking cessation should be encouraged as a critical adjunct to nutritional intervention in nursing home residents with nicotine dependence and weight problems.
Introduction
Intensive public health education has led to a decline in cigarette smoking
over the past four decades. Increasingly, organizations and institutions are
adopting non-smoking policies 1,2. Within long-term care (LTC), residents' rights
to autonomy and self-determination preclude the enforcement of mandatory non-smoking
policies 3. Epidemiological studies show that cigarette smoking is associated
with progressive weight loss 4,5,6. However, although weight loss is an index
of poor outcomes and increased mortality in nursing home residents, smoking
cessation strategies are excluded from most nutritional and weight management
LTC pathways 7,8. 9,10.
Our study was designed to examine the relationship between cigarette smoking
and body weight of residents admitted to a long-term care facility over a six-month
period. Non- smokers were compared with smokers.
Methods
The study was conducted in a long-term care geriatric facility affiliated with
Saint Louis University. All residents of the facility were screened for the
study. Exclusion criteria included congestive cardiac failure, malabsorption
syndrome, chronic diarrhea, chronic obstructive airway disease, cor pulmonale,
liver cirrhosis, or chronic renal failure. Residents with a Mini-mental State
Examination score < 18 or a Geriatric Depression score > were also excluded
11,12. Enteral tube feeding and life expectancy less than six months were additional
exclusion criteria.
Data collated included admission weight and monthly weights for six months following
admission into the facility. The height and body mass index (BMI) on admission
and monthly thereafter for six months were also obtained. Serum albumin levels
within one month of admission and within one month of termination of the study
were obtained. Residents were identified as smokers or non-smokers. Smokers
were defined as residents who had smoked 10 cigarettes daily for at least ten
years. Non-smokers were defined as residents who had not smoked any cigarettes
over the preceding ten years. Residents who fell into neither category were
excluded from the study. Data obtained from non-smokers were compared with data
obtained from smokers. Significant differences between groups was evaluated
using Sato's method to determine odds ratios (OR) and 95% confidence intervals
(CI) and the Student's t-test with two-tailed tests of significance for continuous
variables 13. A p value of less than 0.05 was considered significant. Informed
consent was obtained from all subjects. The study was approved by the Institution
Review Board of the Saint Louis University and the Executive Board of the Long
Term Care facility.
Results
Eighty-eight residents were screened for the study. Fifty-one residents were
eligible for inclusion, comprising 17 (8M, 9F) residents who smoked and 34 (19M,
15F) residents who were non-smokers. Eight (7M, 1F) smokers were admitted with
body mass indices (BMI) less than 22, compared with 12 (7M, 5F) non-smokers
(OR [95% CI] for smokers versus non-smokers = 1.629[0.498 to 5.32] ).
Table 1 shows the admission data for both smokers and non-smokers.
Fig 1 shows the trend of weight change over the six-month study period among
smokers and non-smokers. Among the subset of residents that gained weight the
mean weight gain among smokers was 5.6 "1.3lbs compared with 8.2"2.4lbs
among non-smokers (p=0.004). Among the subset of residents that lost weight
over the study period, the mean weight lost among smokers was 13.3"3.8lbs
compared with 7.8"2.4lbs among non-smokers (p=0.02).
Discussion
Approximately 25% of nursing home residents smoke cigarettes 10, 14. Available
evidence indicates that smoking cessation strategies are less successful within
the long-term care setting. Studies show that adults who continue to smoke into
late life are less likely to cease smoking out of concern for long-term health
effects. Some older smokers erroneously believe that the passage of time has
proven that they are no longer susceptible to the adverse health consequences
of smoking. Likewise, older adults who suffer from smoking related illness often
consider the damage permanent and irreversible and are therefore difficult to
convince of the benefits of smoking cessation 15. Within the nursing home environment,
low levels of perceived self-efficacy, the presence of other smokers and the
reluctance of some health professionals to aggressively educate residents regarding
the dangers of smoking pose additional obstacles to smoking cessation 16.
Currently, in most long-term care facilities in the United States, the institutional
smoking policy is driven mainly by fire and safety concerns 17,18. Thus, residents
are more likely to perceive smoking cessation policies as intrusive legislation
rather than as an integral component of effective health maintenance. Development
of more comprehensive smoking policies that highlight specific adverse health
effects relevant to nursing home residents may be more successful in encouraging
smoking cessation.
Body weight is a critical parameter of care and outcomes determinant within
the nursing home setting. Convincing evidence indicates increased mortality
in long term care residents with weight loss 19,20,21. Our data showed that
smokers admitted into long term care had a BMI compared with non-smokers possibly
as a result of the long-term effect of smoking on suppressing weight gain 5,8,22.
In addition, although the prevalence of weight loss was not significantly different
between smokers and non-smokers, smokers who lost weight in the nursing home,
did so at a faster rate than non-smokers (Fig 1). Our study also showed that
nursing home residents who smoked gained weight at a slower rate, compared with
their non-smoking counterparts. It is conceivable that negative effects of smoking
on food intake, such as anorexia and reduced olfactory and gustatory receptor
sensitivity, may have a synergistic effect in the presence of other adverse
nutritional risk factors, thereby accelerating weight loss 23,24,25, 26.
Cytokine-mediated weight loss is an attractive hypothesis to explain smoking
related weight loss. However, available data is controversial. Cancer related
cachexia is driven by increased elaboration of pro-inflammatory cytokines. The
resultant metabolic abnormalities have been thought to account for the failure
of conventional nutritional supplementation to maintain weight in affected cancer
patients 27. Similar studies in smokers have failed to reveal a consistent alteration
in cytokine levels 28,29. However, evidence indicates that smoking reduces baseline
levels of soluble IL-1 receptor antagonist serum levels thereby resulting in
reduced antagonism of pro-inflammatory interleukins 30. Weight loss in smokers
may therefore result from a dual mechanism involving increased catabolism and
reduced energy consumption.
Applications
These findings justify a more aggressive approach to nutritional support in
smokers with low body weight or significant weight loss. Effective strategies
include the administration of fortified meals and frequent nutritional supplementation
with energy dense food supplements. Additionally, flavor-enhanced foods may
be effective in increasing energy intake in older smokers as enhanced gustatory
stimulation may combat the hypoageusia associated with both smoking and aging
31.
In smokers who continue to lose weight despite aggressive nutritional supplementation,
orexigenic agents, such as megesterol acetate and dronabinol, may be helpful.
Recent evidence indicates that megesterol acetate may enhance weight gain in
nursing home residents. However, the absence of relevant data mandates cautious
use of megesterol in smokers to avoid the possibility of a synergistic or additive
increase in the risk of thrombo-embolic events. Dronabinol (delta-9-tetrahydrocannabinol)
is the active ingredient of Cannabis sativa, approved for use by the Food and
Drug Administration (FDA) as an orexigenic agent in Acquired Immune Deficiency
Syndrome (AIDS). Recent evidence indicates that Dronabinol induces weight gain
in older persons with dementia. However, it remains unclear whether weight gain
in such patients is due to a direct orexigenic effect or a reduction in physical
energy expenditure. Further research is needed to determine the precise role
of Dronabinol as an orexigenic agent in older persons 32,33,34.
Effective weight loss intervention programs in long term care must incorporate
parallel smoking cessation strategies. Clinical Practice Guidelines, such as
those issued by the United States Department of Health and Human Services offer
practical templates for such strategies 35,36, 37. In addition, emphasis should
be placed on the immediate benefits of discontinuing smoking, such as enhanced
taste, increased appetite, weight gain and an increased feeling of well-being.
Residents with weight loss who opt to participate in a smoking cessation program
may benefit from a structured support group directed toward both smoking cessation
and weight maintenance.
The role of medication in LTC residents with weight loss is unclear. Nicotine
replacement therapy may not be appropriate, as animal studies have shown that
nicotine administration reduces food consumption and decreases body weight 38.
Data in humans is lacking. However, residents who lose weight on nicotine replacement
therapy may benefit from a trial of Bupropion in the absence of a history of
seizures or co-existent antidepressant therapy.
Limitations of this study include lack body weight measurements prior to admission,
small sample size and the imbalance in numbers between smokers and non-smokers.
Larger prospective studies may prove helpful.
Conclusion
Smokers in long-term care facilities lost weight more rapidly than non-smokers.
Similarly, weight was regained more slowly in smokers. Long term care health
professionals must be cognizant of the role of smoking in perpetuating weight
loss. Interdisciplinary programs that integrate nutritional support and smoking
cessation strategies should be an integral component of resident care in LTC
facilities that permit smoking.
Acknowledgements: The authors gratefully acknowledge the valuable editorial assistance of Janice D. Hicks.
References
1. Escobedo LG, Peddicord JP. Smoking
Prevalence in US birth cohorts: the influence of gender and education. Am J
Public Health. 1996;86:231-236
2. Conway TL, Hurtado SL, Woodruff MA. Tobacco use: Prevention and cessation
programs in the US Navy. Public Health Reports 1993;108:105-115
3. Omnibus Budget Reconciliation Act of 1987, Public Law 100-203, Sections 4201(a),
4211(a). Washington, DC: Centers for Disease Control.
4. French SA, Jeffrey RW. Weight concerns and smoking: a literature review.
Ann Behav Med 1995; 17:234-244
5. Klesges RC, Klesges LM, Meyers AW. Relationship of smoking status, energy
balance, and body weight analysis of the second Health and Nutrition Examination
Survey. J Consult Clin Psychol 1991;59:899-905
6. Williamson DF, Madans J, Anda RF et al. Smoking cessation and severity of
weight gain in a national cohort. N Engl J Med 1991;324:739-745
7. Ryan C, Bryant E, Eleazar P et al. Unintentional weight loss in long term
care: predictor of mortality in the elderly. Southern Medical Journal 1995;88(7):721-724.
8. . Tayback M, Kumanyika S, Chee E. Body weight as a risk factor in the elderly.
Arch Intern Med 1990;150:1065-1072
9. Adler G, Greeman M, Rickers S, Kuskowski M. Smoking in Nursing Homes: Conflicts
and Challenges. Soc Work Health Care 1997;25(4):67- 81.
10. Kochersberger G, Clipp EC. Resident smoking in long-care facilities - Policies
and Ethics. Public Health Reports. 1996;111:66-70
11. Folstein MF, Folstein SE, McHugh PR. " Mini-mental state." A practical
method for grading the cognitive state of patients for the clinician. J Psychiatr
Res. 1975; 12:189-198.
12. Yesavage JA, Brink TL, Rose TL et al. Development and validation of a geriatric
depression screening scale: A preliminary report. J Psychiatr Res 1982;17:189-198
13. Sato T. Confidence limits for the common odds ratio based on the asymptotic
distribution of the Mantel-Haenszel estimator. Biometrics 1990;46:71-80
14. Max W. The financial impact of smoking on health related costs: a review
of the literature. Am J Health Promotion. 2001; 15(5): 321-331
15. Sullivan LW. The health benefits of smoking cessation. DHSS publication
No. 90-8416. 1990. Washington, DC: Department of Health and Human Services
16. Cox JL. Smoking cessation in the elderly patient. Clinics in Chest Medicine.
1993;14(3):423-428
17. Kochersberger G, Clipp EC. Resident smoking in long-term care facilities
- policies and ethics. Public Health Reports. 1996;111(1): 66-70
18. Barker JC, Lewis DE Jr. Smoking policy in long term care: a survey of administrators
in San Fransisco. Journal of Health and Social Policy. 1998;10(1):81-100.
19. Ryan C, Bryant E, Eleazar P et al. Unintentional weight loss in long term
care: predictor of mortality in he elderly. South Med J 1995;88(7):721-724.
20. Klesges RC, Klesges LM. Cigarette smoking as a dieting strategy in a university
population. Int J Eating Disord. 1988;7:413-419
21. Weekley CKIII, Klesges RC, Reylea G. Smoking as weight control strategy
and its relationship to smoking status. Addict Behav. 1992;17:259-271.
22. Moffat RG, Owens SG. Cessation from cigarette smoking: change in body weight,
body composition, resting metabolism and energy consumption. Metabolism 1991;40:465-470.
23. Klesges RC, Ward KD, Ray JW et al. The prospective relationships between
smoking and weight in a young biracial cohort: The Coronary Artery Risk Development
in Young Adults Study J Consult Clin Psychol. 1998;66:987-993.
24. French SA, Jeffrey RW, Forster JL et al. Predictors of weight change over
two years among a population of working class adults: the Healthy Worker Project.
Int J Obesity1994;18:145-154.
25. Colditz GA, Segal MR, Myers AH et al. Weight change in relation to smoking
cessation among women. J Smoking Relat Disord 1992;3:145-153.
26. Winkler S, Garg AK, Mekayarajjananonth T et al. Depressed taste and smell
in geriatric patients. J Am Dent Assoc 1999;130(12):1759-1765.
27. Barber MD, Ross JA, Fearon KC. Cancer Cachexia. Surgical Oncology. 1999;8(3):133-141
28. Sher ME, Bank S, Greenberg R et al. The influence of cigarette smoking on
cytokine levels in patients with inflammatory bowel disease. Inflammatory Bowel
Diseases 1999;5(2)73-78
29. Satoh T, Tolterud DJ, Guevarra L et al. Chemiluminescence assays for cytokines
in serum: influence of age, smoking, and race in healthy subjects. Arerugi 1995;44(7):661-669
30. Hofbauer LC, Muhlberg T, Konig A et al. Soluble IL-1 receptor antagonist
levels in smokers and non-smokers with Graves Opthalmopathy undergoing orbital
radiotherapy. J Clin Endocrinol Metab 1997;82(7):2244-2247.
31. Mathey MAM, Siebelink E, de Graaf C, Van Staveren WA. Flavor enhancement
of food improves dietary intake and nutritional status of nursing home elderly.
J Gerontol Med Sci 2001;56A:M200-M205
32. MacIntosh C, Morley JE, Chapman I. The anorexia of aging. Nutrition 2000;16:983
- 995
33. Voth EA, Schwartz RH. Medicinal applications of delta-9-tetrahydrocannabinol
and marijuana. Ann Intern Med 1997;126:791-798.
34. Volicer L, Stelly M, Morris J et al. Effects of Dronabinol on anorexia and
disturbed behavior in patients with Alzheimers disease. Int J Geriat Psychiatry
1997;12:913-919
35. Fiore MC, Bailey WC, Cohen SJ et al. Treating tobacco use and dependence
: Clinical Practice Guideline. Rockville, MD, U.S. Department of Health and
Human Services: Public Health Service, 2000
36. Coleman T. Smoking cessation: integrating recent advances into clinical
practice. Thorax. 2001;56(7):579-582.
37. Senore C, Battista RN, Shapiro SH et al. Predictors of smoking cessation
following physicians' counseling. Prevent Med 1998; 27:412-421.
38. Winders SE, Wilkins DR 2nd , Rushing PA, Dean JE. Effect of nicotine cyclingon
weight loss and regain in male rats. Pharmacology, Biochemistry and Behavior.
1993;46(1):209-213
39. Committee for Diet and Health, Food and Nutrition Board. National Research
Council Diet and Health. Diet and Health: implications for reducing chronic
disease risk. Washington, D.C. : National Academy Press, 1989.
Table 1:
| Smokers (n = 17) | Non-smokers (n = 34) | P value | |
| Age (Yr) | 77.2+/-11 | 79.3+/-12 | 0.29 |
| Admission weight (lbs) | 158+/-27 | 165+/-44 | 0.27 |
| Admission BMI | 24.2+/-3 | 27.4+/-9 | 0.04 |
| Serum albumin (g/dl) | 3.8+/-0.3 | 3.4+/-0.5 | 0.16 |
Values are expressed as means " SEM.
BMI (Wt [kg] / Ht [m2] [accepted normal range: 22 - 27]) 39
Fig 1: Weight trends in smokers and non-smokers six months after admission
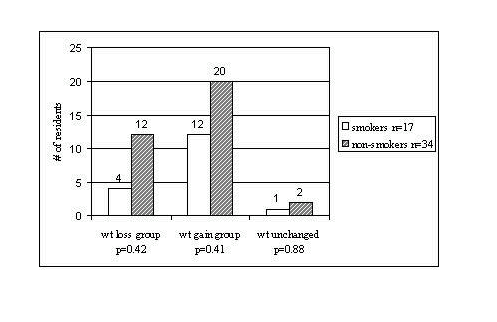
First Published: June 15, 2002
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages copyright ©Priory Lodge Education Ltd 1994-

