BRAIN COMPUTERIZED TOMOGRAPHY UTILIZATION BY PRIMARY CARE PHYSICIANS
Michael Sherf1,2 M.D.,
|
2Kupat Holim Clalit,
|
Address
for Correspondence:
Prof.
Pesach Shvartzman
Chairman,
Division of Community Health
Ben-Gurion
University of the Negev
P.O.
Box 653
Beer-Sheva,
84105
Israel
Tel: 972-7-6477429/30
Fax:
972-7-6477636
Email: spesah@bgumail.bgu.ac.il
ABSTRACT
Objective: To evaluate the indications and results of referrals for brain computerized tomography (CT) by primary care physicians.
Design & Setting: All referral forms and results of CTs ordered by primary care physicians for ambulatory patients between January and June, 1994, in two imaging institutes in the Southern HMO District of Israel, were collected and analyzed.
Main Outcome Measures: Brain CT referral rate, CT indications and results.
Results: 1,238 brain CT scans were performed. Male represented 40% of the population referred. Headache without neurological findings was noted as the main reason for referral (38%). The findings were completely normal in 66% of the CTs, in 39 patients (3.2%) a brain tumor was found, and in 19 patients (1.5%) a cyst. Patients between the ages of 20-49 were diagnosed with an adverse outcome at a higher rate than the other age groups (p<0.00001) and women were diagnosed with a brain tumor at a significantly higher rate than men (p<0.05). The overall annual referral rate was 7.29 CTs per 1000 population.
INTRODUCTION
In recent years we are witnessing a crisis in health care systems around the world as different countries are faced with the need to control health care costs while attempting to provide high quality care. One of the main reasons for the increase in health expenditures is the high cost of medical diagnostic procedures such as computerized tomography (CT) and magnetic resonance imaging (MRI)1. These procedures are some of the more expensive tests ordered by primary care physicians.
Primary care physicians are often required to make a decision regarding referral for CT. This decision is usually based on a mixture of factors: the medical history, the physical exam, a consultant's advice, the patient's request, and other medical considerations. The physician has also to consider the risks of the test, in terms of exposure to radiation, the cost of the test, and the cost of incidental findings resulting at times in over-investigation which can be both expensive and potentially harmful. Moreover, the underlying anxiety of the patient and his family has a clear influence on the physician's decision. As much as brain CT is a good diagnostic test, wide use of this test on every patient with a headache, is expensive and may lead to false positive or false negative results1.
The review of the literature revealed few studies that analyzed specifically the use of brain CT by primary care physicians.
In this study we evaluated the indications and results of referrals for brain CT by primary care physicians, in a single HMO region.
METHODOLOGY
All referral forms and results of brain CTs ordered by primary care physicians for ambulatory patients between January and June 1994, in two imaging institutes serving the Southern District of Israel were examined. The population in this region mounts approximately 400,000, and these are the only centers providing this service in this region. A more detailed investigation was performed on nine clinics in this district in order to calculate the specific referral rate. The data was collected from the referral forms which included demographic information, the type of doctor initiating the referral, the reason for the referral, the postulated diagnosis and the results of the test.
All referral forms for this period were collected, and data entry and analysis were performed using epi info 6.0 and SPSS-PC statistic software, to carry out standard statistical tests (as Chi-Square and t-tests). A p<0.05 was defined as statistically significant.
RESULTS
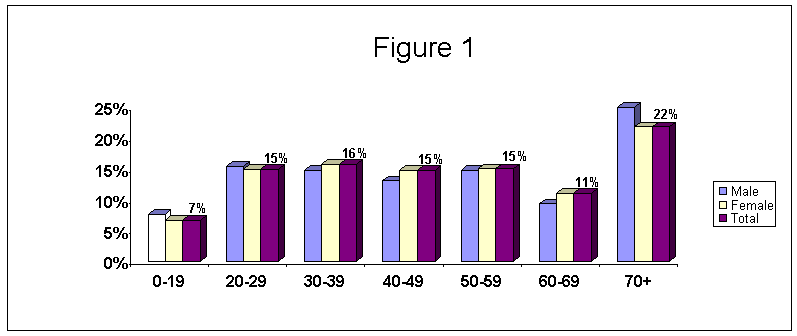
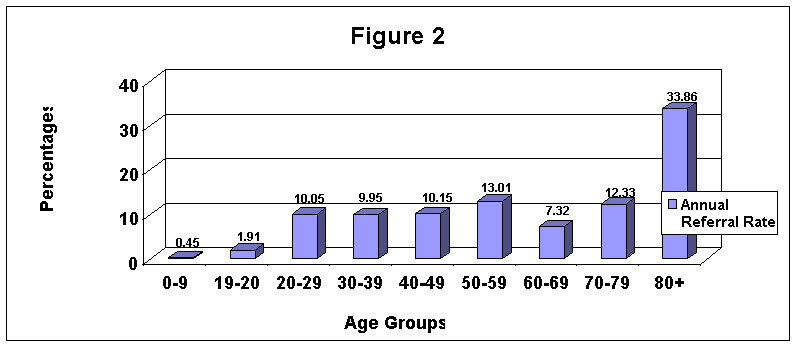
In the six-month-period mentioned above 3,230 CT scans were performed, of them 1,238 (38.3%) were brain CT scans. Of these, male represented 40% (493), female 57% (711), and for 3% (34) gender was not mentioned. Figure 1 depicts the age and sex distribution of these patients (missing data for 92 patients). The initiator of the referral was the primary care physician in 38% of the cases, a consultant in 57% and unknown in 5% of the tests. To calculate the annual referral rate per 1,000 population, population figures for the sample of nine clinics were obtained. The results are depicted by age groups in Figure 2. These clinics, which are distributed in the region, serve a population of approximately 72,500 people. The population in these clinics consists of 29% of the region population. The overall annual referral rate was calculated to be 7.29 per 1000 population. In general, the referral rate for brain CT increases with age to peak at the oldest age group of over 80 with the exception of the 60-69 age group where a drop in the referral rate is noticed. The referral rate of the patients over 80 is 33.86, which is 3-4 times the rate in the previous age groups (20-79). No significant differences in referral rates were noted when comparing board certified family and internal medicine practitioners or non-specialist general practitioners.
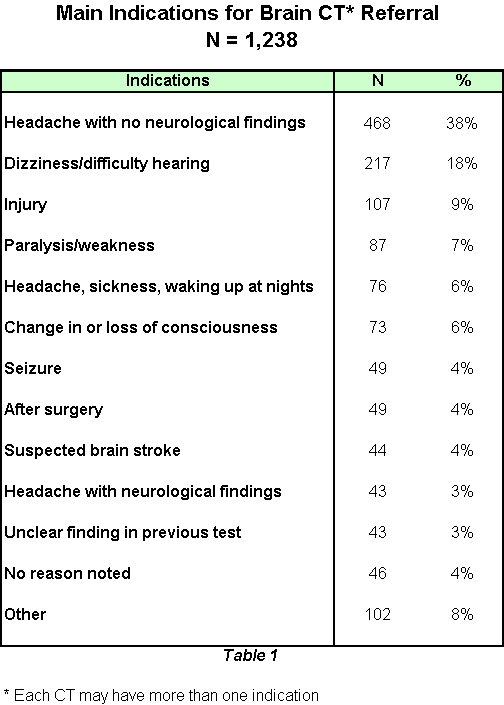
Table 1 denotes the indications leading to the referrals. Headache without neurological findings was noted as the main reason in 468 (38%) of the patients, dizziness in 217 (18%) patients, and trauma in 107 (9%) patients. The majority of the physicians did not indicate any suspected diagnosis (760 patients, 61%). Nevertheless, in 196 patients (16%), the postulated diagnosis was tumor.
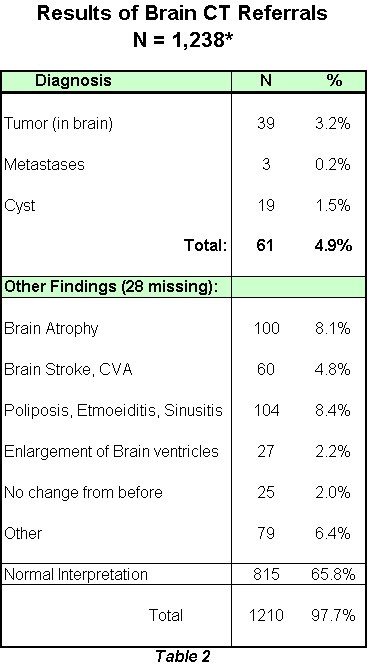
Table 2 shows the main results of the brain CTs performed. In the majority of the patients the CTs were completely normal (815 patients, 65.8%). In 39 patients (3.2%) a brain tumor was observed, and in 19 patients (1.5%) a cyst was found. Other findings included atrophy (100) 8%; brain stroke, CVA (60) 5%; and sinusitis, ethmoiditis and nasal poliposis in (104) 8% of the patients. Women were diagnosed with brain tumor at a significantly higher rate than men (p<0.05) though for other diagnoses the rates were similar. Age was also found to be a significant factor. In most cases the age group of 20-49 year old, were diagnosed with an adverse outcome at a higher rate than the other age groups (p<0.00001). A presumed diagnosis was not indicated in about two thirds of the brain CTs. In only 8 patients who were suspected to have a tumor the diagnosis was confirmed. In 13 (34.2%) of the patients with a headache with no neurological findings a tumor was found, sinusitis was found in 28 (28.9%) patients, and a CVA in 7 (17.5%) patients.
DISCUSSION
A recent survey from Israel assessed the utilization of all radiological exams (personal communication). The referral rate was higher among female physicians and older physicians, but no differences were found between Board Certified family medicine physicians and general practitioners. In the same work, differences were found in the referral rate of different age groups to CT. The rate increased with age from 0.6 per 1000 population per month, in the age group of 0-9, to a rate of 7.2 in the 70-79 year old. The total average CT referral rate per 1000 population was 2.91.
In our study, it is observed that brain CT referral rate, follows the same age pattern mentioned above for all CTs. The rate increases with age, plateaus at age groups 20-79, and then peaks to a monthly rate of 5.64 people per 1,000 at the over 80 age group. We also did not find any differences between the different types of physicians (family physician, internal medicine, general practice or specialists) with regard to brain CT outcomes and referral rates.
Using CT early in the diagnostic stages is claimed by some to be advantageous5,6 as it prevents repeated office visits and unnecessary anxiety suffered by the patients, whereas others believe that CT should be performed only in cases where clear medical history and physical findings are found7. A National Institutes of Health (NIH) consensus development conference on the use of CT scans8 suggested that CT scans be used for only a minority of patients with headaches. The NIH report suggested that the test be considered only for patients whose headaches are "severe, constant, unusual, or associated with abnormal neurological signs". In reality we know that the decision to refer for a brain CT is a complex combination of considering the medical history and exam, patients or family request, consultation advice and doctor-patient relationship.
A few studies focused on the analysis of the cost-effectiveness of CT scans in the investigation of patients with headache6,7,9,10 though none have considered the cost of follow-up of repeated tests or other examinations due to "uncertain clinical significance" noted on the CT report or on the other hand anxiety, depression and loss of work days in those patients not having the test. Some primary care physicians might consider to perform a CT as a treatment tool. Any guideline in the future should take into account consultants and primary care physicians concerns, since 57% of the CTs were ordered by primary care physicians are following a consultant advice.
Our results show that the main indications for referrals were headache, dizziness, injury, and paralysis/weakness. Of these, the first three are common reasons for a visit in primary care. Patients' expectations or medicolegal reasons were not included as indications, probably since Israeli primary care physician did not consider these as legitimate indications. The outcomes of the CT show that out of 196 patients who were referred with a presumed diagnosis of tumor only 39 (19.9%) were found to have one and, in general, a pathological finding existed in 4.9% of the patients. No pathological finding was true for the majority of the patients (66%).
In a wide ranging study of 58 primary clinics in the US and Canada examining referrals of brain CT, it was found that 3% of those suffering from headaches were referred for a brain scan. It was also found that out of 339 brain scans, approximately 50% were referred due to suspected tumor (compared with 16% in our study), 12% due to patients expectations, 9% due to suspected subarachnoid hemorrhage, 5% were referred by a specialist, 5% for medicolegal reasons, and 20% for other reasons. For 15% of the patients there were neurological findings in the physical exams and in the scans: 14 patients (5%) had tumor (compared with 3% in our study), subarachnoid hemorrhage or subdural hematoma; and in 44 patients (15%) incidental findings (such as atrophy, anatomical variants) of no great significance were detected3.
In another study examining positive finding of brain CT of 164 people in a private neurological practice, results were pathological in 19% of the cases (compared with only 4.9% found in our study). The common symptoms and the indications for the referrals were headache (in 51 people) and seizures (in 36 people), and the majority of the study population were over 40 years of age2. Headaches and dizziness were the most common indication in our study although the study populations here are not comparable. A poor correlation was found between the presumed diagnosis and the results of the CT. It seems that sinusitis is a common incidental finding in brain CTs.
In this study, sinusitis was also found to be a common incidental finding. In general there was poor correlation between the presumed diagnosis noted and the actual result of the CT as in other previous studies.
As clear guidelines are not available the physician has to use his best clinical judgment, taking into account the patient-physician relationship, cost-effective calculations and the outcomes of false-positive and false-negative results. In one study examining the physician's ability, indications for body CT were examined in order to identify those groups with no "clinical justification". The conclusion of the research team was that the number of patients who had undergone CT without justified medical cause was not significant4.
REFERENCES
1. Oppenheimer J, Avni Y. Population characteristics as a predominant factor in radiology utilization (personal communication).
2. Rentens, D C, Stewart-Wynne, E G. (1989) Factors influencing the yield of cranial CT scanning in a private neurological practice. Clin Exp Neurol. 26, 169-175.
3. Becker, L A, Green, L A, Beaufait, D, Kirk, J, Froom, J, Freeman, W L. (1993) Use of CT scans for the investigation of headache: a report from ASPN, Part I. J Fam Pract. 7, 129-34.
4. Naik, K S, Ness, L M, Bowker, A M, Robinson, P J. (1996) Is computed tomography of the body overused? An audit of 2068 attendances in a large acute hospital. Br J Radio. 69, 126-131.
5. Bohmfalk, G L. (1980) Computerized tomographic scans for headache [letter]. JAMA. 244, 133-4.
6. Knaus, W A, Wagner, D P, Davis, D O. (1981) CT for headache: cost/benefit for subarachnoid hemorrhage. Am J Roentgenol. 136, 537-542.
7. Larson, E B, Omenn, G S, Lewis, H. (1980) Diagnostic evaluation of headache: impact of computerized tomography and cost effectiveness. JAMA. 243, 359-362.
8. NIH Consensus Development Panel. (1982) Computed tomographic scanning of the brain. JAMA. 247, 1955-1958.
9. Baker, H L. (1983) Cranial CT in the investigation of headache: cost effectiveness for brain tumors. J Neuroradiol. 136, 91-96.
10. Carrera, G F, Gerson, D E, Schnur, J, McNeil, B J. (1977) Computed tomography of the brain in patients with headache or temporal lobe epilepsy: findings and cost effectiveness. J Comput Assist Tomogr. 2, 200-203.
Legend Figure 1:
Age and Gender Distribution of Patients Referred for Brain CT (n=1,238)
Legend Figure 2:
Annual Referral Rate per 1000 population for a sample of selected clinics (72,500 patients)
BIOGRAPHIC SKETCHES OF AUTHORS:
1. Dr. Michael Sherf - Medical Director of Kupat Holim Clalit (HMO) Southern Region; Family Medicine Specialist, Instructor at the Family Medicine Department of Ben-Gurion University of the Negev.
2. Dr. Michael Friger - PhD in Mathematics; Senior Researcher at the Epidemiology Department, Ben-Gurion University of the Negev.
3. Dr. Hava Tabenkin - Family Medicine Specialist, Senior Lecturer and Head of the Department of Family Medicine, Ha'emek Medical Center, Ben-Gurion University of the Negev.
4. Anat Neville - MBA in Health Administration, Research Coordinator, Research Center for Primary Care and Family Medicine, Family Medicine Department Ben-Gurion University of the Negev.
5. Prof. Pesach Shvartzman - Family Medicine Specialist, Chairman, Division of Community Health, Head of the Department of Family Medicine, Ben-Gurion University of the Negev. Chairman of the Israeli Palliative Association.
[1]Support for this study was granted by the Israeli Ministry of Health
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages copyright ©Priory Lodge Education Ltd 1994-

