From Episodic Treatment
to Chronic Disease Management:
Shifting the Over 65 Population to an Alternative Model of Care.
| Christine Walker Ph D Chronic Illness Alliance Melbourne Australia Donna Southern Department of General Practice University of Melbourne Australia |
Chris Peterson Ph D Faculty of Medicine, Nursing and Allied Health Monash University McMahons Rd, Frankston, 3199, Victoria Melbourne Australia |
- Abstract
- Introduction
- Why target the over 65s?
- Distribution
- Hospitalisation
- How people with chronic disease experience the system
- Current Australian Healthcare
- Conclusion
Abstract
The purpose of this discussion
paper is to outline the need to refocus the health care system in Australia
for the 65+ population to one with a chronic disease emphasis. Like many developed
nations the Australian health care system is focuses on providing acute care,
but with significant increases in growth of the 65+ age group over the past
two decades or so, there is a significant growth in chronic diseases and comorbidities.
The authors present data for the growth in the use of hospital and other services
by the older populations, and identify some of the principles required for an
appropriate system of care.
Introduction
Chronic diseases are those that "...occur across the whole spectrum of illness, mental health problems and injuries. Chronic diseases tend to be complex conditions in how they are caused, are often long-lasting and persistent in their effects and can produce a range of complications" (AIHW 2002). Chronic conditions are those which are long-term (lasting more than 6 months) and can have a significant effect on a person's life. Management to reduce the severity of both the symptoms and the impact is possible in many conditions. Management includes medication and/or lifestyle changes such as diet and exercise, and stress management (Health Insite 2003a). At the same time, it should be noted that chronic diseases may get worse, lead to death, be cured, remain dormant or require continual monitoring.
In Australia today the ageing of the population poses significant problems to the healthcare system, including increased costs, inappropriate modes of service delivery and problems of chronic disease prevention. The challenge is to move from an acute focussed health care system to one that for the 65+ population has a chronic disease focus. So far, measures such as incentives programs for general practitioners, for example Enhanced Primary Care, do not deliver systemic and coordinated programs. Coordinated Care Trials which began in 1997, while providing coordinated services during the trial period in a number of localised areas have not produced sustained or systemic results (Duckett 2000, p212). The Australian health system is struggling to care for this section of the population in an appropriate, cost-effective and timely manner.
Chronic disease management for the 65+ population must produce a system that is financed and organised to provide optimum chronic rather than acute care for those with chronic diseases, co-morbidities and complications. It will need to be integrated between all major providers and be coordinated with a health professional responsible for the coordinated management of care for each patient in the system. It is likely that the system will have elements of a Managed Care model with capitation payments to providers and a managing organisation providing payments and overseeing management. It needs to be focussed at the community level, and if possible administered from the community level, such as local council, with the Commonwealth and states contributing funding through grants. The system will need to provide for public and privately insured patients. Such a system will need reference back to consumer review, and to be guided by consumer involvement and participation.
The major stakeholders in the Australian system are the Commonwealth and State Governments, primary care providers such as GPs and allied health care providers, local government, secondary providers such as specialists, organizations such as aged residential care (eg. nursing homes and hostels), and consumers of these services.
In its report 'Tackling Chronic Disease: Exploration of Key Research Dimensions, Synopsis of Workshop, 5-6 July, 2001', The National Health and Medical Research Council (NHMRC) has identified chronic disease for the ageing population as a particular challenge. First, in financing, where the "supply side" needs to accommodate a more consumer-focussed system; second, there needs to be a shift to continued care from episodic care; third, prevention and health promotion needs to take on a greater role; fourth, there needs to be a national approach to planning and evaluation; fifth, research needs to be translated into practice; and sixth, wider disciplines need to be engaged in the required changes.
The NHMRC 2001 workshop
that developed the above priority areas identified a number of issues for consideration.
These were:
" What are the characteristics of a healthy society?
" What is the role of peer-support groups and/or individuals in chronic
disease management and prevention?
" What are the contributors to risk behaviour during the life course?
" How can a model be developed for an assessment of total economic costs
of chronic disease?
" 'How effective would a new unified system of care be in comparison with
existing arrangements?' ; and
" What types of governance models are most effective in moving research
into practice, regarding sustainability, transferability, management and prevention?
The purpose of this discussion paper is to outline the need to refocus the health care system for the 65+ population to one with a chronic disease emphasis, and to identify the principles required for an appropriate system of care.
Why target the 65+ population?
Significant increases in life expectancy have occurred throughout the twentieth century. From 1947 to 1996, the Australian population doubled. During this same period the population aged 65+ trebled (Duckett 2000, p1). In conjunction with the increase in life expectancy, the expanding proportion of older Australians is experiencing an increase in the frequency of chronic diseases (Duckett, 2000 pp11-13) same The number of Australians aged 65 and older will swell from a current 2.4 million to 4.2 million in 20 years' time. The average life expectancy will grow from around 55 years, to over 75 years for people born now (CFC, 2000).
Fitzgerald and Haebich (2002) maintain that the ratio of older people compared to the working aged population will increase by two and one half times over the next 40 to 60 years. The "baby boomer" section of the population will inflate the aged proportion of the population as an entire group by 2025. Their health care needs will be most crucial between 2020 and 2050. The older population's effect on health care costs will be exacerbated by increasing costs of pharmaceuticals and other inputs.
Musculoskeletal diseases, circulatory diseases, mental illnesses, respiratory diseases, diabetes, cancers and injuries are areas characterised by chronicity and are major expenses to the fee for service health system as well as being major considerations in terms of the burden of disease (Duckett, 2000).
Chronic conditions are not limited to the older age groups. Key population data from the Australian Bureau of Statistics on health status for 1995 indicated that 86% of the population experienced some illness in the two week prior to the survey, or had an ongoing chronic condition (lasting at least 6 months), or both. Young adults (25-34 years) reported high levels (86%) of illness, and over 95% of the population over age 45 reported some form of illness. The most common chronic conditions reported over all were: eyesight problems (51.1%); arthritis (14.6%); hay fever (13.7%); and asthma (11.1%) (AIHW, 2002).
However, aside from mental disorder, most of the National Health Priority Areas (NHPA) disease groups increase in prevalence among the older age groups. Chronic arthritis and other musculoskeletal disorders affect approximately 17% of the Australian population, contributing to about one third (34.4%) of reported disability and ranks third highest in the list of disease groups responsible for most health system expenditure. The high level of diagnoses associated with heart disease reflects the prevalence of cardiovascular problems or conditions in the Australian population. Approximately 15.5% of the Australian population had a cardiovascular problem in 1995. Cardiovascular disease is the leading NHPA, with 40% of all deaths attributable to it. Of particular concern is injury due to falls, accounting for 44.4 deaths per 100,000 population among those aged 65+. A variety of other chronic diseases and conditions increase in prevalence in the older population. For example, hospitalisation rates for chronic obstructive pulmonary diseases increased sharply during 1997-98 particularly for males in the 50-54 years age group.
According to McCallum (2003) the problem with chronic disease in older age groups concerns co-morbidity and substitute morbidity, which represents increased expenditure for the government. In trying to prevent one disease another disease occurs, for example in stopping heart attacks, 25% of people who are saved subsequently develop dementia. This means that savings in one area of care are inadvertently shifted as costs to another area.
Distribution of Chronic Diseases
The following table is derived from Australian Bureau of Statistics (ABS) data and reports the prevalence of NHPA diseases and conditions for 1995. Cardiovascular diseases and conditions and asthma are the leading contributors to the burden of disease. Approximately 40% of the Australian population suffered from an NHPA disease during the survey time period.
Table 1 Prevalence of NHPA diseases, 1995
| NHPA Priority Area | Number ('000) | % Total Population |
| Cardiovascular | 2,795.5 | 15.5 |
| Asthma | 2,041.4 | 11.3 |
| Injury & poisoning | 1,153.9 | 6.4 |
| Mental disorder | 1,047.6 | 5.8 |
| Diabetes | 430.7 | 2.4 |
| Cancer | 379.6 | 2.1 |
Examination of these disease groups by age provides a picture of their distribution across the population. However, this critique is limited because it is not possible to combine the data on the incidence and prevalence for each of the conditions due to differences in data reporting. Also, age group categories vary, preventing direct comparisons of aggregated data.
Cardiovascular disease
Cardiovascular disease is the third highest cause of death among the 25-44 year age bracket. It is the second highest cause of death among the 45-64 year age bracket and the leading cause of death among the 65+ age group. It is Australia's largest health concern, accounting for 39% of all deaths. Stroke is also a leading cause of disability. Around 40,000 Australians annually suffer a stroke, with around 50% of all strokes occurring in the 75+ age bracket.
Asthma
Asthma is highly prevalent in Australia and is a significant cause of disability, impacting greatly on quality of life. Based on self-reports in the 1995 National Health Survey, approximately 11.3% of the population had asthma. It is most prevalent among 5-14 year olds (19.2%) followed by 15-24 year olds (14.9%). It is one of the more common reasons for visits to a casualty or emergency department. In 1999-2000, asthma was the principle diagnosis for 0.8% of all hospital visits and was the most frequent reason for hospitalization among children (0-4 years). After age 14 the hospitalization rates decreased, reaching the lowest rate in the 35-44 age group (<50 per 100,000 population).
Mental Health
Mental health problems and disorders such as depression, anxiety and schizophrenia are common and affect about one million Australians. They account for much disability and contribute to the death of many Australians per year. Information on the national prevalence and types of mental health problems and disorders have limitations due to difficulties surveying high prevalence populations, for example the homeless. There tends to be low response rates and variability in definitions. The National Survey of Mental Health and Wellbeing 1997 estimates 17.7% of adults in Australia had an anxiety, affective or substance use disorder or a combination of these. Data by age groups was not available.
Diabetes
Diabetes is the sixth leading cause of death in Australia and contributes to significant illness, disability, and poor quality of life. It shares several of the risk factors with cardiovascular disease and is itself a risk factor. Approximately 7.5% of the population aged over 25 is estimated to have diabetes (AIHW 2002) This condition increases in prevalence with age from 0.3% among the 25-34 year age group to approximately 24% among those aged 75+. There is a marked difference in the age profile of people with different types of diabetes. Type 1 diabetes is the most common form among children and young adults. Type 2 diabetes is predominant among middle-aged and elderly due to its rapid increase in prevalence after age 45.
Cancer
The overall incidence for cancer is lowest in late childhood. In adult life it increases with age. The age standardised incidence rates are approximately 475 per 100,00 for males and 347 per 100,000 for females. It is expected that 1 in 3 males and 1 in 4 females in Australia would be diagnosed with cancer in the first 75 years of life.
The increase in mortality rate due to cardiovascular disease with age is particularly evident. Death rates from cancer increase with age, from age 15. The older population make up a higher proportion of those dying from cancer, and this proportion is increasing. In 1983 approximately 30% of all cancer deaths occurred in the 75+ age group compared with 45% in 2000.
Hospitalisation
Figures on hospital usage provide one part of the picture of the impact of chronic disease or conditions on the population. Not all people with a chronic disease end up using hospital services. There is little doubt that the highest users of hospital services are the 65+ age group. Figure 1 shows that the largest surge in both hospital separations and patient-days in hospital occurs across the 65-74 age brackets. However, it may be noted that this surge is emergent in the 55-64 age bracket.
Figure 1 Hospital usage by age group for Victorian males
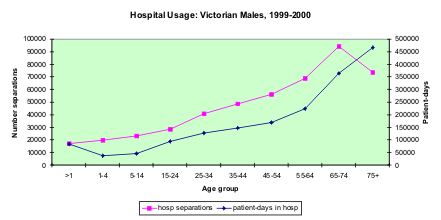
In 1999-2000 there were 1.9 million hospital separations for people in the 65+ age group. The most common principal diagnosis for hospitalisations among the 65+ age group in 1999-2000 were: dialysis (11.9% of separations); followed by other medical care (4.6% separations); and cataracts (3.9% separations). Diagnoses associated with heart disease represented a third of the top 15 principal diagnoses, accounting for 8.0 % of separations. The most commonly reported procedures for older Australians during hospitalisation were generalised allied health interventions (37% separations), followed by operations on blood vessels including haemodialysis (12% separations), and extraction of eye lens (4.9 % separations).
The National Strategy for an Ageing Australia (Office for an Ageing Australia 2002) outlines that 'considerable attention has been given to strengthening Medicare to support the integrated health care for Australians with chronic and complex conditions in the primary care sector. Better coordination and integration in the other sectors and across sectors of the care system would deliver considerable benefits to many older people with multiple complex conditions'. The report cites under-diagnosis of depression in the elderly as problematic, as is the existence of co-morbidities which complicates the type of care older people receive.
The ageing population, which includes Indigenous populations, those from various other ethnic backgrounds, and from rural and remote areas, has a diversity of needs. This diversity and the substantial range of differences in the burden of disease means the population needs to be dealt with by a flexible service delivery. The ageing of the population will affect the demand for health services, such as community care and dementia services. The report (Office for an Ageing Australia, 2002) maintains that 'the strengthening of the primary care sector for example could deliver improved health outcomes' for the 65+ population, 'through the better prevention and management of disease, and the potential reduction in demand for community care and hospital services'.
There are strong arguments for focussing on the 65+age group, although as with the targeting of any particular age group there is some contradictory evidence. In about one third of OECD countries there is a positive relationship between the proportion of the 65+ population and expenditure. In Australia one third exhibits a negative relationship, and one third for which the relationship is not statistically significant, indicating that not all of the aged population will be a burden on the health care system. Duckett (2000 p31) argues that there is a high level of expenditure on the final years of life which is mainly the elderly. While Zweifeld et al. (1999) argue that there is little relationship between ageing and health expenditure. In addition there will be certain groups with a burden of disease, such as Indigenous populations, who would be excluded, and this is an equity issue. However, another solution might be that for Indigenous populations, for example the age be lowered to 45+ years. Nonetheless, 65 years represents a cut-off point at which increases in chronic disease and hospitalisations are combined with increased reliance on pensions, representing considerable costs to the community. It is possible that evaluation of a trial of the 65+ population would reveal other significant at-risk groups which could then participate in future trials.
How people with chronic disease experience the system
When individuals have a chronic disease, whether from birth or contracted in later life, they are likely to engage with the health system to a greater extent than anyone else. This may begin with visits to a general practitioner, followed by diagnostic tests, pharmaceutical prescriptions, consultations with specialists, visits to hospitals and possibly surgery. This may also take place in the context of a reduced earning capacity. For example, the Consumers' Health Forum (1997) researched some of the costs associated with having a chronic disease. The study found that people with chronic disease faced far greater costs than the average population. In 1996 the 7557 households in the sample that reached the general safety net between January and June spent 50 times (if the household reached it in June) to 8 times (if the household reached it in January) more on pharmaceuticals than the average household in the highest income bracket.
At the same time that people with chronic diseases require maximum health services, they are least able to afford them. Those within the 65+ population with a sustained chronic disease are likely to have been on welfare benefits (including WorkCare, TAC etc.) before the usual retirement age of 65 years. People with chronic disease may have also continued to work, though this may have been part time or casually (Ezzy et al 1998). However, the welfare system acts as a disincentive for this. People 65+ years old who have long-term illnesses are less likely to have accumulated sufficient superannuation over their working lives (Berrill, 2002). This may be less an artefact of their illness than one of a health and welfare system not designed to meet their needs (Lubeck and Fries, 1993).
An important aspect of living with a chronic disease is that as people become older they may develop other illnesses. Co-morbidities have a number of impacts; these people have even more expenses, they suffer the effects of polypharmacy (Hopkins et al 2000) and suffer increased effects of the illnesses themselves. While it is true that people with a chronic disease are more at risk of adverse events than are well people simply because they are in more constant contact with the health system, those elderly people with co-morbidities are at even greater risk because of the complexity of their illnesses and their care.
The current Australian health system and the place of chronic disease care
In 1996 Wagner et al (1996 p 520) argued that successful chronic illness programs aimed to meet the needs of people with chronic illnesses. Thus care programs were successful if they took into account the complexities faced by people with chronic illnesses in their daily lives (Wagner et al 1996 p523), rather than create yet more obstacles in the person's daily life.
As a health insurance system, the present state of Medicare presents some obstacles for the 65+ population with chronic disease. The disappearance of bulk-billing general practices in both rural and urban areas creates a disincentive to seek timely medical care (Commonwealth Dept of Health and Ageing 2002). The rising co-payments for the MBS, the PBS and a range of community services are significant obstacles for people with multiple co-morbidities seeking services (CHF 1997). As well, the lack of Medicare support for allied health services means that people with chronic illnesses seek medical intervention that is at least reimbursed at some level, rather than the less expensive and more appropriate allied health services. Nonetheless, despite the reduction in bulk-billing, Medicare does provide a comprehensive coverage of service payments covering a large range of health services. This provides greater access than people would otherwise have. The report from the NHMRC workshop (2001) indicated that access was a problematic idea, and that the issue is about the nature of care itself rather than simple "getting care". Enhanced Primary Care (EPC) payments were introduced to encourage GPs to develop care plans for the elderly with chronic disease so that they could access allied health and nursing services in the community. Recent research demonstrated that GPs considered the extra paperwork was a disincentive to implementing care plans and that case conferencing was impossible to implement (Oldroyd et al 2003 p32).
Increasingly care plans and care teams are seen as the best approach to chronic care for the 65+ age group, in an otherwise fragmented health system (Wagner 2000). Wagner et al (1996, p 520) presaged the need for "practice redesign", where there was a conscious deviation from the usual way care was delivered to the allocation of tasks across a team of health professionals. Practice redesign also means a greater emphasis on new approaches to care by professionals where self-management and self-monitoring become are actively encouraged (Wilson 1999, Wagner et al 1996). (This has been reflected in the demonstration projects of the Australian Sharing Health Care Initiative (2003). For example the Flinders Human Behaviour and Health Research Unit provides a range of education packages to health professionals which aims to educate them on redesigning the way they work with people with chronic illnesses. The emphasis that these demonstrations projects (for example the Whitehorse Division of General Practice project, "The Good Life Club", 2003) now place on chronic disease self-management reflects that planned deviation from the way care was previously delivered.
One of the challenges in Australia, to the delivery of good quality care in multidisciplinary teams to the 65+ group is the divide that currently exists between specialist medical care and generalist medical care. Currently, most care teams and care planning takes place at the primary care level. However, many people with chronic illnesses see medical specialists periodically. Lack of communication between these practitioners, and sometimes conflicting advice, means that older consumers still experience a fragmented system. Similarly, use of tertiary care and the use of specialised allied health services may remain outside the team. Care planning and care teams that overcome these obstacles that are largely the product of the fragmented health system will assist a refocus on the needs of the 65+ person with chronic illnesses.
Conclusion
In conclusion, there are strong arguments for refocussing the health care system for the over 65 age group to one with a chronic disease management emphasis. This age group is growing in number and longevity. The health care needs of this group will eventually represent a significant burden for the Australian health care system, which could be better managed through a chronic illness management approach. Such an approach has potential to reduce both the financial and health impacts of the disease or conditions, and effects of polypharmacy, on the individual.
There is a need for an integrated approach for providing a chronic disease management model, which addresses the current fragmentation between the primary, secondary and tertiary sectors of the health care system. Health promotion and risk promotion initiatives tend to focus on the NHPA illnesses, taking a population health approach. However, some funding to focus on non-NHPA illnesses may also be beneficial in order to provide more comprehensive management strategies.
Whilst a focus on the over 65 age group omits some at risk groups such as Indigenous Australians, and some ethnic groups, a lower age cut-off could be used where appropriate. Generally, the age 65 represents a cut-off point at which increases in chronic disease and hospitalisations are maximised. These increases also correspond with increased reliance on pensions, and considerable cost to the community. Chronic disease management, for the elderly requires even greater integration of all services, including welfare, primary, secondary and tertiary health services through care planning. Only this approach removes reliance on the less appropriate acute medical services.
References
Australian Institute of Health and Welfare, 2002, 'Chronic diseases and associated risk factors in Australia', www.aihw.gov.au/publications/phe/cdarfa01 20, Dec, 2002).
Berrill, J. 2002, Disability
and Superannuation. Submission to the Senate Committee on Superannuation and
Disability on Behalf of the Chronic Illness Alliance Inc., August, Maurice Blackburn
Cashman, Melbourne.
Commonwealth Department of Health and Ageing, 2002, Medicare Statistics June
Quarter, Tables B5 and B7, http://www.health.gov.au/haf/medstats/index.htm
Consumers' Health Forum, 1997, The Costs of Chronic Disease, Consumers' Health Forum, Canberra.
Duckett S. J. 2000, The Australian Health Care System, Oxford University Press, Melbourne.
Ezzy, D., de Visser, R., Bartos, M., McDonald, K., O'Donnell, D. & Rosenthal, D. 1998, HIV Futures Community Report: Health, Relationships, Community and Employment, National Centre in HIV Social Research, Monograph Series no. 4, La Trobe University, Melbourne.
Fitzgerald, V. & Haebich, W. 2002, The Future Costs of Health and Aged Care. A Health Reform Discussion Group Forum: The Australian Health Care System: Directions for Reform, Melbourne Business School, 19 Sept, 2002.
Health Insite 2003a, www.healthinsite.gov.au/content/internal/page.cfm
Health Insite 2003b, www.chronicdisease.health.gov.au/sharing.htm
McCallum J (2003) personal communication January 2003.
Lubeck, D & Fries, J 1993, 'Health status among persons infected with Human Immunodeficiency Virus: A community-based study', Medical Care, vol. 31, pp. 269-276.
National Health and Medical Research Council, 2001, Tackling Chronic Disease: Exploration of Key Research Dimensions, Synopsis of Workshop, 5-6 July, 2001. NHMRC and Commonwealth Department of Health and Aged Care, Canberra.
Office for an Ageing Australia 2002, National Strategy for an Ageing Australia, www.health.gov.au/acc/ofoa/ageing_policy/nsaa/nsaabk9.htm
Oldroyd J,Proudfoot J, Infante F, Powell Davies G, Bubner T, Holton C, Beilby J, Harris M, 2003, Providing healthcare of people with chronic illness: the views of Australian GPs, MJA, vol 179, no 1, pp 30-33.
Wagner E, 2000, The role of patient care teams in chronic disease management, BMJ, vol 320, pp 569-572
Wagner, E., Austin, B. & Von Korff, M. 1996, 'Organizing care for patients with chronic illness', Milbank Quarterly, vol. 74, no. 4, pp. 511-44.
Zweifel, P., Felder, S.
& Meier, M. 1999, 'Ageing of population and health care expenditure: a red
herring?' Health Economics, vol. 8, pp. 485-96.
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages copyright ©Priory Lodge Education Ltd 1994-

