Assessing the Prevalence, Quantification, and Morphological Composition of Coronary Atherosclerosis in Patients with Type 2 Diabetes and the Metabolic Syndrome via 64-Slice CT Angiography
Jeffrey J. Fine, PhD, MS
Vice President, Research and Education
Cardiovascular Innovations, LLC
63 Lawrin Ct.
Irmo, SC 29063
USA
Ali A. Rizvi, MD
Department of Medicine Division of Endocrinology, Diabetes, and Metabolism University of South Carolina School of Medicine Columbia, SC 29203 USA
Keywords: cardiovascular computed tomography, diabetes, metabolic syndrome, coronary atherosclerosis
Abstract
Background:
We determined the prevalence, morphology, and severity of coronary artery plaque in high-risk patients via 64-slice cardiovascular computed tomography (CVCT).
Methods: Based on chart review, 101 subjects having a 64-slice CVCT were assigned to one of three groups: diabetes, metabolic syndrome, or comparison. Disease severity was classified as: no disease, subclinical disease (lesions <70%), or clinically significant disease (lesions >70%). Plaque morphology was stratified as either vulnerable or stable plaque by Houndsfield units and established American Heart Association criteria. Results: Diabetic subjects had the highest prevalence of CAD (78%), compared to 65% in the metabolic syndrome subjects and 55% in the comparison group (p<.05). Diabetic subjects were also most likely to have both significant CAD (41%), and stable plaque (52%) followed by metabolic syndrome subjects (33% and 25%) and the comparison group (15% and 20%) (p<.05). The metabolic syndrome group was most likely to have vulnerable lesions (36%) potentially placing them at increased risk of acute events. 22% of subjects in the diabetes group, 35% in the metabolic syndrome group, and 45% in the comparison cohort were disease-free. Conclusions: 64-slice CVCT allows non-invasive diagnosis and stratification of subjects with diabetes and the metabolic syndrome, providing relevant information regarding coronary disease prevalence, severity, and plaque composition, which are statistically different among these high risk patient cohorts.Introduction
Over the last 50 years, the incidence and prevalence of coronary artery disease (CAD) have climbed steadily in the majority of westernised countries (Centers for Disease Control and Prevention, 2004). Statistics also reveal that human society is in the midst of an epidemic of obesity-related disorders and type 2 diabetes (King, Aubert, & Herman, 1998). The entities of pre-diabetes and the metabolic syndrome are three times as common (Ford, Giles, & Dietz, 2002), and are believed to increase the risk of progression to type 2 diabetes and cardiovascular disease. The latter remains the primary cause of diabetes-associated morbidity and mortality, as more than two-thirds of people with diabetes die of heart or vascular disease (Centers for Disease Control and Prevention, 2004). The impact of diabetes on cardiovascular disease is further illustrated by the fact that the risk of developing a myocardial infarction in diabetic patients without known heart disease is equivalent to the risk observed in non-diabetic survivors of a prior infarction (Haffner, et al., 1998).
Because of the high incidence of CAD among diabetic patients, the need for accurate and early identification is paramount. CT angiography has received a boost recently with the availability of the 64-slice CT scanner. The latest generation of CT scanners can provide exquisite imaging of cardiac structures, coronary plaque morphology data, and details of atherosclerotic lesions quickly and with minimal patient discomfort or risk.We undertook a retrospective review of patients who underwent Cardiovascular CT (CVCT) angiography at the South Carolina Heart Center from the time of acquisition of the machine in December 2005 to present. The objectives of this study were to determine the prevalence and severity of coronary atherosclerosis between nondiabetic patients, subjects with type 2 diabetes, and those with the metabolic syndrome. We also sought to determine if coronary plaque morphology, composition, and characteristics varied between the three groups.
Methods
One hundred and one adult patients were studied retrospectively. Patients referred to the South Carolina Heart Center (Columbia, SC) by primary care physicians for a diagnostic angiography for suspected CAD were included in this study. Information on body weight, waist circumference, blood pressure, cholesterol, serum creatinine, fasting glucose, and glycosylated hemoglobin (HbA1c) was collected if available.
Patients were assigned to one of three study groups based upon their medical chart: nondiabetic (controls), type 2 diabetes, or the metabolic syndrome. In most cases, the existence of diabetes had already been noted by the patients' primary or referring physician. In other subjects with hyperglycemia, the American Diabetes Association (ADA) criteria for the diagnosis of diabetes (Table 1) were used for confirmation. For the diagnosis of the metabolic syndrome, the National Cholesterol Education Program Adult Treatment Panel lll (NCEP ATP lll) criteria (Table 2) were utilised. Note that an overlap exists between type 2 diabetes and the metabolic syndrome; some individuals satisfy the diagnostic clinical criteria for both conditions. For the purposes of this study, any subject who fulfilled the American Diabetes Association (ADA) criteria for the diagnosis of diabetes was assigned to the type 2 diabetes group. Impaired fasting glucose (IFG) or impaired glucose tolerance (IGT) was used as one of the possible diagnostic features for the metabolic syndrome.
All subjects had CVCT angiography as a part of their normal clinical course. Procedures were performed at the South Carolina Heart Center using the Siemens Sensation Cardiac 64-Slice CT. Using a 64-slice CVCT scanner, a volume data set was acquired (64 x 0.6-mm collimation, gantry rotation time 33 ms, pitch .2 mm, tube voltage of 120 kV), covering the distance from the carina to the diaphragmal face of the heart. Tube current was modulated according to the EKG, with a maximal current of 500 mA during a time period of 330 ms centered around 55% of the cardiac cycle and reduction by 80% during the remaining cardiac cycle, leading to an FDA estimated average effective radiation dose of 4.3 mSv (Jakobs, et al., 2002). Cross-sectional images were reconstructed with a slice thickness of .75 mm in 0.4 mm intervals with the use of an EKG gated half-scan reconstruction algorithm (Flohr, et al., 2002) to obtain an image acquisition window of 164 ms. All vessels > 1.5mm were evaluated.
Patients with a resting heart rate >60 beats per minute were intravenously medicated with Lopressor (Metoprolol) 5 mg to enhance image quality and reduce distortion. A heart rate of 60 beats per minute or less critically influences image quality and is considered a threshold that is desirable to minimize motion artefacts (Schroeder, et al., 2002). The CVCT scans were read by a trained cardiologist through the South Carolina Heart Center.
Subject's disease status were categorised as: no disease, subclinical disease (one or more coronary lesion between 10%-70%), and clinically diseased (one or more lesions >70%). Plaque morphology, as defined by Houndsfield unit definitions was stratified as: unreported/unknown, vulnerable plaque (AHA type IV/Va lipid core plaque), or stable plaque (AHA type Vb (calcific) or Vc (fibrotic) plaques).
Descriptive statistics (frequency distributions and mean values) were completed for each patient cohort. All values are presented as the mean ± standard deviation. Statistical significance was evaluated among the three or cohorts using the one-way ANOVA. Differences were considered to be statistically significant at P value of <.05.
Results
One hundred and one adult subjects were assigned to predefined study cohorts (diabetic, metabolic syndrome, control) for this analysis. The diabetic cohort consisted of 27 subjects, 10 of which were male (37%). The mean age of the diabetic cohort was 62 ±12 years (range 34-82). There were 34 subjects assigned to the metabolic syndrome cohort, 20 of which were male (59%). The mean age of the metabolic syndrome cohort was 59 ±12 years (range 34-74). There were 40 subjects assigned to the control/comparison group, 22 of which were male (55%). The mean age of the control cohort was 59 ±12 years (range 30-81).
All visualised coronary vessels with a diameter greater than 1.5mm were included in this evaluation. Ninety-nine vessels were evaluable in the diabetic cohort with 5% of vessels uninterpretable due to motion artifact, erratic heart rate, or insufficient image quality. Within the metabolic syndrome cohort, 114 vessels were evaluated with 6% of the vessels uninterpretable. Among controls, 165 vessels were evaluated with 5% of vessels uninterpretable.
The prevalence of atherosclerotic heart disease was calculated within each study cohort (Figure 1). There was a distinct and statistically significant (p<.05) linear effect among the study cohorts. Diabetic subjects had the highest prevalence of CAD at 78% (21/27). Those subjects having metabolic syndrome had a CAD prevalence rate of 65% (22/34), while the comparison group had a prevalence rate of 55% (22/40).
The distribution of subjects falling into the three disease stratifications (no disease, subclinical disease, clinical disease) was calculated within each of the study cohorts (Figure 2). A linear relationship exists among subjects having no disease. Forty-five percent of the comparison cohort was found to be absent of CAD, while only 35% of metabolic syndrome subjects and 22% of diabetics were disease-free (p<.05). Subjects with clinically significant disease (one or more coronary vessel at least 70% occluded) also had a statistically significant (p<.05) linear relationship among the study cohorts. Diabetic subjects were most likely to have clinically significant CAD (41%). Metabolic syndrome subjects evidenced clinical disease in 33% of cases, while only 15% of the comparison group was found to have clinically significant CAD. The distribution of subjects having subclinical CAD (one or more lesion between 10%-70% occluded) was fairly comparable among study cohorts: diabetics 37%, metabolic syndrome 32%, and controls 40%.
The distribution of subjects having vulnerable (AHA type IV/Va lipid core) plaque was staggered among the study cohorts (Figure 3). Only 22% of diabetic subjects were found to have lipid core lesions. Those with metabolic syndrome (36%) were most likely to have vulnerable coronary lesions. Thirty-three percent of the comparison group was found to have vulnerable plaque. A graded and statistically significant (p<.05) relationship exists among the study cohorts when analysing the distribution of stable plaque (AHA type Vb (calcific) or Vc (fibrotic). Fifty-two percent of diabetic subjects were found to have stable coronary lesions, while only 25% of metabolic syndrome subjects and 20% of the comparison group evidenced the same lesion morphology.
Discussion
It is imperative that accurate and relatively noninvasive tests be developed to detect CAD early in high-risk individuals, thereby reducing the burden of mortality, morbidity, and cost stemming from these disease states. Additionally, the analysis of the morphological composition of coronary lesions has tremendous implications. Heterogeneous plaque is an independent risk factor for stroke or coronary event regardless of the degree of stenosis (Polak, et al., 1998, and Bluth, 1997, and Sterpetti, Schultz, & Feldhouse, 1998). Atherosclerotic plaque stability is directly related to histological composition (Nair, et al., 2002). The American Heart Association has designated the different types of human atherosclerotic lesions according to their pathology (American Heart Asssociation, 2003). Because of the heterogeneity in the composition of human atherosclerotic plaques, reliable noninvasive imaging that can detect early atherosclerotic disease and characterize the composition of the plaques is clinically desirable (Fayad & Fuster, 2001). Disruption- prone plaques, the so called "vulnerable plaques" (Type IV/Va), tend to have a thin fibrous cap (cap thickness ~ 65 to 150 um), a large lipid core occupying more than 40% of the plaque's volume, increased numbers of macrophages, reduced numbers of smooth muscle cells, and an increased expression of tissue factor (Fayad & Fuster, 2001 and Ihling, 1998). Acute coronary syndromes often result from a disruption of a modestly stenotic vulnerable plaque, and subjects with vulnerable plaques were discovered to have a much higher event risk than those with other types of plaque based on the results of the Tromso study (Taylor, et al., 2000 and Mathiesen, et al., 2001).
The only fully reliable method for plaque classification is histology (Arnold, et al., 1997). Few data exist regarding the morphology of the vulnerable plaques in clinical settings, and as a result, prognostic risk models have had limited success in predicting coronary events (Detrano, et al., 1999 and Yamagishi, et al., 2000). CVCT is an effective and relatively non-invasive method for the detection of atherosclerosis and may accurately classify plaque composition within the arteries (Nieman, et al., 2001, and Kopp, et al., 2002, and Knez, et al., 2001). Investigators have reported a high degree of sensitivity and specificity for detection of coronary stenoses with thin-slice (16-slice) spiral CT (Nieman, et al., 2002) and multiplanar reconstruction(Ropers, et al., 2003), demonstrating excellent correlation with angiography. With the use of 64-slice CVCT scanners promising possibilities await which enable noninvasive coronary imaging, and permit not only plaque detection and quantification, but potentially plaque classification as well, thus improving existing prognostic models. The latest generation of multislice tomography techniques offer an enhanced spatial and temporal resolution Flohr, et al., 2004), thus allowing detailed information about plaque architecture and composition. High-resolution visualization of atherosclerotic plaque morphology and architecture, with respect to thickness and stability of the protective fibrous cap, offered with the 64-slice CVCT could be instrumental for identifying vulnerable coronary plaques that lead to acute events (Yabushita, et al., 2002 and Goldstein, 2002).
Our review is the first to evaluate the increased coronary atheromatous burden in patients with type 2 diabetes and the metabolic syndrome with CVCT, and provides interesting insights into the characteristics of the disease in these high-risk populations.It is to be noted that even our comparison group had a higher risk of CAD because of being a cohort that was referred for cardiac evaluation due to symptoms or clinical features. Nevertheless, the prevalence of CAD was predictably higher in the patients with the metabolic syndrome compared with the comparison group, since by definition the former had a clustering of multiple cardiovascular risk factors. The analysis also reinforces the extremely elevated risk that the majority of patients with diabetes face, since this group had the highest prevalence of CAD.
Figure 2 illustrates an interesting data distribution that may appear deceptively counter-intuitive but makes sense on closer scrutiny. Most of the patients with subclinical (<70% lesions) disease were in the control group, but this was probably because a greater proportion of patients in the metabolic syndrome and diabetes groups fell in the clinical disease category. As expected, the control group had the highest proportion of disease-free subjects, while the diabetes group had the lowest. Finally, patients with diabetes made up the majority of those with significant coronary lesions.
Subjects with diabetes had, by far, the highest frequency of total and stable lesions, reiterating the status of the disorder as a powerful "cardiac risk equivalent". However, vulnerable plaques were more likely to be seen in the other two groups, mainly because the long time-frame of coronary pathology seen in patients with diabetes leads to chronic, fibrotic, more "stable" lesions. Referral patterns may have played a part as well: in a situation where high-risk patients, especially those with pre-existing multiple risk factors as in the metabolic syndrome, are being evaluated, the likelihood of unstable lesions increases. This should not be construed as seemingly minimizing the risk that patients with diabetes face, since they have a much higher prevalence of coronary atherosclerotic plaques overall and are prone to "silent ischemia" that can lead to anatomic chronicity over time.
Patients with type 2 diabetes and the metabolic syndrome may have a higher prevalence of subclinical atherosclerosis and may progress to occlusive disease more rapidly than those without diabetes or metabolic syndrome. Many patients with diabetes already have evidence of early stage cardiovascular disease and it is essential that these patients be treated early with proven therapies to reduce their risk of future cardiovascular events (Fayad, et al., 2002). Insulin resistance in diabetes was linked to carotid intimal thickness and atherosclerosis (Wagenknecht, et al., 2003). The Chest Pain Evaluation by Creatine Kinase-MB, Myoglobin, and Troponin I (CHECKMATE) trial evaluated 30-day clinical outcomes after initial presentation of cardiovascular disease symptoms in both a diabetic and non-diabetic population. The results substantiate the need for early detection of cardiovascular disease within the diabetic population as the overall major acute coronary event (Death/ MI/ Revascularization) rate was three times higher in the diabetic cohort (19%- 6% respectively) (Newby, et al., 2001). Similarly, according to an analysis of 6,200 adults followed for 13.3 years, the presence of the metabolic syndrome significantly increased the risk of death from coronary heart disease and cardiovascular causes (Malik, et al., 2004). Previous studies have failed to provide accurate, inexpensive, and relatively noninvasive imaging techniques to detect early, subclinical, yet potentially unstable, atherosclerotic cardiovascular lesions in at-risk patients (such as those with diabetes and the metabolic syndrome). Since patients with type 2 diabetes and the metabolic syndrome have an increased incidence of coronary artery disease, they constitute a very important group to evaluate using the promising new technology of CVCT.
In conclusion, cardiovascular CT angiography is an emerging technology that carries great potential for delineating the epidemiology and distribution of coronary atherosclerosis in a way never before envisioned. It has the ability to identify subclinical disease, stratify existing lesions, and noninvasively detect critical or advanced disease. The 64-slice CVCT is the latest advance in this field. Our results suggest that CVCT provides clinically relevant information regarding coronary disease prevalence, severity, and plaque composition. It has a promising role for non-invasive detection and stratification of coronary atherosclerosis in diabetes, the metabolic syndrome, and possibly other high-risk patients. It is obvious that further studies are needed in this exciting and important field of cardiovascular imaging and macrovascular disease, especially in individuals with multiple risk factors.
References
- American Heart Association. A definition of advanced types of atherosclerotic lesions and a histological classification of atherosclerosis. Available at: http://216.185.102.50/Scientific/statements/1995/17950005tl-2.html. 2003.
- Arnold JA, Modaresi KB, Thomas N, et al. Ultrasound grading of plaque morphology: Is qualitative assessment a valid approach?, European Journal of Ultrasound 6 (1997), pp. 15-16.
- Bluth EI. Evaluation and characterization of carotid plaque, Ultrasound CT MR 18 (1997), pp. 57-65.
- Centers for Disease Control and Prevention. Preventing Heart Disease and Stroke. Addressing the Nation's Leading Killers, 2004. Atlanta, GA. Available at http://www.cdc.gov/nccdphp/aag/aag_cvd.htm. 2004.
- Detrano RC, Wong ND, Doherty TM, et al. Coronary calcium does not accurately predict near-term future coronary events in high-risk adults, Circulation 99 (1999), pp. 2633-2638.
- Fayad ZA, Fuster V, Nikolaou K, et al. Computed tomography and magnetic resonance imaging for noninvasive coronary angiography and plaque imaging, Circulation 106 (2002), pp. 2026-2034.
- Fayad ZA, Fuster V. Clinical imaging of the high-risk or vulnerable atherosclerotic plaque, Circulation Research 89 (2001), pp. 305-316.
- Flohr T, Stierstorfer K, Raupach R, Ulzheimer S, Bruder H. Performance evaluation of a 64-slice CT system with z-flying focal spot, Fortschr Rontgenstr 176 (2004), pp. 1803-1810.
- Flohr T, Bruder H, Stiersdorfer K, et al. New technical developments in multislice CT, part 2; sub-millimeter 16-slice scanning and increased rotational speed for cardiac imaging. Rofo Fortschr Geb Rontgenstr Neuen Bildgeb Verfahr 174 (2002), pp. 1022-1027.
- Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults. Findings from the Third National Health and Nutrition Examination Survey, Journal of the American Medical Association 287 (2002), pp. 356-359.
- Goldstein JA. Angiographic plaque complexity; the tip of the unstable plaque iceberg, Journal of the American College of Cardiology 39 (2002), pp. 1464-1467.
- Haffner SM, Lehto S, Ronnemaa T, Pyroala K, Laakso M. Mortality from coronary heart disease in subjects with type 2 diabetes and in non-diabetic subjects with and without prior myocardial infarction, New England Journal of Medicine 339 (1998), pp. 229-234.
- Ihling C. Pathomorphologic classification of coronary atherosclerosis, Herz 23 (1998), pp. 69-77.
- Jakobs TF, Becker CR, Ohnesorge B, et al. Multislice helical CT of the heart with retrospective ECG gating; reduction of radiation exposure by ECG-controlled tube current modulation, European Radiolology 12 (2002), pp. 1081-1086.
- King H, Aubert RE, Herman WH. Global burden of diabetes, 1995-2025: Prevalence, numerical estimates, and projections, Diabetes Care 21 (1998), pp. 1414-1431.
- Knez A, Becker CR, Leber A, et al. Usefulness of multislice spiral computed tomography angiography for determination of coronary artery stenoses, American Journal of Cardiology 88 (2001), pp. 1191-1194.
- Kopp AF, Schroeder S, Kuettner A, et al. Noninvasive coronary angiography with high resolution multi-row computed tomography, European Heart Journal 23 (2002), pp. 1714-1725.
- Malik S, Wong ND, Franklin SS, et al. Impact of the metabolic syndrome on mortality from coronary heart disease, cardiovascular disease, and all causes in United States adults, Circulation 110 (2004), pp. 1245-1250.
- Mathiesen EB, Bonaa KH, et al. Echolucent plaques are associated with high-risk cerebrovascular events in carotid stenosis – the Tromso study, Circulation 103 (2001), p. 217.
- Nair A, Kuban B, Tuzca EM, et al. Coronary plaque classification with intravascular ultrasound radiofrequency data analysis, Circulation 106 (2002), pp. 2200-2206.
- Newby LK, Storrow AB, Gibler WB, et al. Bedside multimarker testing for risk-stratification in chest pain units: the chest pain evaluation by creatine Kinase-MB, myoglobin, and Troponin-I (CHECKMATE) study, Circulation 103 (2001), pp. 1832-1837.
- Nieman K, Cademartiri F, Lemos PA et al. Reliable noninvasive coronary angiography with fast submillimeter multislice spiral computed tomography, Circulation 106 (2002), pp. 2051-2054.
- Nieman K, Oudkerk M, Rensing BJ, et al. Coronary Angiography with multi-slice computed tomography, Lancet 357 (2001), pp. 599-603.
- Polak JF, Shemanski L, O'Leary DH, et al. Hypoechoic plaque at US of the carotid artery: an independent risk factor for incident stroke in adults aged 65 years or older, Radiology 208 (1998), pp. 649-654.
- Ropers D, Baum U, Pohle K et al. Detection of coronary artery stenoses with thin-slice multi-detector row spiral computed tomography and multiplanar reconstruction, Circulation 107 (2003), pp. 664-666.
- Shroeder S, Kopp AF, Kuettner A, et al. Influence of heart rate on vessel visibility in noninvasive coronary angiography using new multislice computed tomography: experience in 94 patients, Clinical Imaging 26 (2002), pp. 106-111.
- Sterpetti AV, Schultz RD, Feldhouse RJ. Ultrasonic features of plaque and the risk of subsequent neurologic deficits, Surgery 104 (1998), pp. 652-660.
- Taylor AJ, Burke AP, O'Malley PG, et al. A comparison of the Framingham risk index, coronary artery calcification, and culprit plaque morphology in sudden cardiac death, Circulation 101 (2000), pp. 1243-1248.
- Wagenknecht LE, Zaccaro D, Espeland MA, et al. Diabetes and progression of carotid atherosclerosis: The Insulin Resistance Atherosclerosis Study, Arteriosclerosis Thrombosis and Vascular Biology 23 (2003), pp. 1035-1041.
- Yabushita H, Bouma BE, Houser SL, et al. Characterization of human atherosclerosis by optical coherence tomography, Circulation 106 (2002), pp. 1640-1645.
- Yamagishi M, Terashima M, Awano K, et al. Morphology of vulnerable coronary plaque: insights from follow-up of patients examined by intravascular ultrasound before an acute coronary syndrome, Journal of the American College of Cardiology 35 (2000) pp. 106-111.
Tables
Table I. The American Diabetes Association (ADA) criteria (1997) used for the diagnosis of diabetes mellitus in the present study*
- Classic symptoms of diabetes (polyuria, polydipsia, and unexplained weight loss) plus casual plasma glucose concentration
 200 mg/dl. Casual was defined as any time of day without regard to time since last meal, or
200 mg/dl. Casual was defined as any time of day without regard to time since last meal, or - Fasting Plasma Glucose
 126 mg/dl (7.0 mmol/l). Fasting was defined as no caloric intake for at least 8 hours, or
126 mg/dl (7.0 mmol/l). Fasting was defined as no caloric intake for at least 8 hours, or - Two-hour post-load glucose
 200 mg/dl during an Oral Glucose Tolerance Test, when available.
200 mg/dl during an Oral Glucose Tolerance Test, when available. - Any of the above confirmed on another day
*From: American Diabetes Association: Clinical Practice Recommendations 2004. Standards of medical care in diabetes. Diabetes Care. 2004;27(Suppl 1):S15-S35. www.diabetes.org/diabetescare, accessed on 20 September 2004.
Table II. Clinical diagnosis of the metabolic syndrome (if three or more of the following were present) used in the current analysis, based on the National Cholesterol Education Program (NCEP) Adult Treatment Panel III (ATP III) guidelines.*
RISK FACTOR |
DEFINING LEVEL |
| 1. Waist circumference | |
men |
> 40 inches |
women |
> 35 inches |
| 2. Fasting glucose | = or > 110 mg/dl |
| 3. Blood pressure | |
systolic |
= or > 130 mm Hg |
diastolic |
= or > 85 mm Hg |
| 4. Triglycerides | = or > 150 mg/dl |
| 5. HDL-C | |
men |
< 40 mg/dl |
women |
< 50 mg/dl |
* From: Executive Summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 2001, 285:2486-2497.
Figure I. Coronary artery disease prevalence by study cohort.
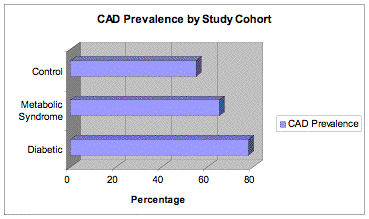
* p <.05
Figure II. Coronary artery disease severity by study cohort.
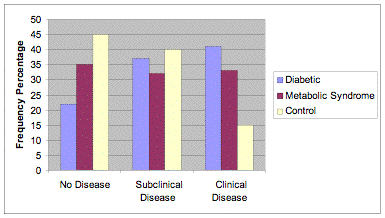
No Disease: p<.05, Clinical Disease p<.05
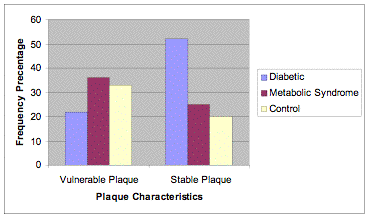
Figure III. Plaque composition by study cohort.
Stable Plaque: p<.05
First Published November 2006
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages copyright ©Priory Lodge Education Ltd 1994-

