AN ANALYSIS OF DRUG USE INDICATORS IN PRIMARY CARE HEALTH FACILITIES OPERATING IN THE CITY OF KRAGUJEVAC
Irena R. Kostic2, Zoran N. Kovacevic2
AN ANALYSIS OF DRUG USE INDICATORS IN PRIMARY CARE HEALTH FACILITIES OPERATING IN THE CITY OF KRAGUJEVAC |
Slobodan M. Jankovic1, Ljiljana M. Vasic2,
Milan R. Maksimovic2, Vojislav B.Cupurdija2, Irena R. Kostic2, Zoran N. Kovacevic2 |
1 - Center for clinical and experimental pharmacology, Clinical Hospital Center "Kragujevac", Kragujevac.
2 - Students, Medical Faculty, Kragujevac.
Correspondence to: Prof. Dr Slobodan M. Jankovi}, Center for clinical and experimental pharmacology, Clinical Hospital Center "Kragujevac", Ul. Zmaj Jovina 30, P.O.Box 179
34000 Kragujevac, Serbia, Yugoslavia. Tel. ++381 34 370023/ ext. 224. fax. ++381 34 370073. e-mail: slobodan@medicus.medf.kg.ac.yu
The best way to analyze drug use in health facilities is to study universal indicators, which are not dependent either on investigator or time of measurement.
The aim of our study was measurement and analysis of drug use in 5 state pharmacies, 4 general practice outpatient health facilities and 4 specialist outpatient health facilities in Kragujevac, Serbia.
Values of drug use indicators (established in 1995 by WHO) were measured prospectively, from December 1998 to March 1999. In each health facility a sample of 100 patient-visits was investigated. Our study showed that average consultation time had been too short. The average number of drugs per encounter (from 1 to 2.8) was higher than values of the same indicator in other countries. Percentage of drugs prescribed by generic name (from 16% to 39%) was lower than in other countries. Percentage of encounters with an antibiotic prescribed (from 29% to 45%) was similar to values observed in other countries. In health care facilities of Kragujevac injections are prescribed rationally, but percentage of drugs prescribed from essential drugs list (from 21% to 65%) is lower than values observed in other studies. Average dispensing time was about 24 seconds, which is close to minimum value from other studies (12.5 seconds) and too short for proper interaction between pharmacist and a patient.
There are significant variations in percentage of drugs actually dispensed (from 39% to 68%), which points to unbalanced supply of pharmacies. Serious negligence exists when labeling of dispensed drugs is concerned: name of the patient was written on the dispensed drug in only a few cases. Patients' knowledge of correct dosage was observed in high percentages, but validity of this finding is doubtful, since the patients were not willing to fully cooperate with investigators. Very good characteristic of pharmacies in Kragujevac was high availability of key drugs, much higher than in other countries. The results of our study suggest the need for educational intervention in primary care health facilities operating in city of Kragujevac.
Key words: drug use indicators, primary care, health facilities.
The extent of drug use is directly affected by prescribing behavior of physicians, especially in primary care. The best way to investigate drug use in health facilities is usage of indicators created and validated by World Health Organization1,2. There are twelve core drug use indicators sorted in three groups: prescribing indicators (five), patient care indicators (five) and facility indicators (two). Values of indicators are usually measured in one point of time (cross-section), and then periodically, especially after intervention aimed to correct actual practice of drug use. The National Health Service in Serbia is state-run, and divided to primary care (for outpatients) and secondary care (for inpatients). The primary care facilities are of three types: general practice facilities, specialist care facilities and pharmacies. The aim of our study is determination of values of drug use indicators in primary care health facilities operating in city of Kragujevac; measured values could be used later as baseline for further follow-up of quality of drug use.
The values of drug use indicators were measured prospectively, in 4 general practice health facilities, in 4 specialist outpatient health facilities and in 5 pharmacies operating in city of Kragujevac, during the time period between December 1998 and march 1999. The health facilities were chosen randomly, by implementation of random numbers tables; they comprise about 30% of all primary care outpatient health facilities in city of Kragujevac. In each health facility a sample of 100 patient-visits was investigated. The same group of investigators performed all measurements. The values of the indicators were calculated in following way:
I Prescribing indicators
II Patient care indicators
II Health facility indicators
The checklist of key drugs was established before the study and it was limited to 15 products chosen according to their importance and frequency of usage. They are: epinephrine, hydrocortisone, aspirin, morphine, penicillin, diazepam, aminophylline, furosemide, insulin, diclofenac, captopril, aminoglycosides, digoxin, glyceryl trinitrate, intravenous solutions (NaCl 0,9% or glucose 5%).
Values of the indicators determined in our study are shown in figures 1 to 10.
Labeling of drugs was inadequate in all cases of dispensed drugs except in two. The main problem was omission of the patient's name on drug package.
At the end of the study it turned out that in general practice health facilities a copy of essential drugs list (9th edition, issued by World Health Organization) was not available; the same happened in three pharmacies, while in two other pharmacies and in specialist outpatient health facilities the list was available.
Although the highest number of drugs prescribed per encounter was observed in Nigeria (3.8), this is an extreme value, unusual in other countries3-6. In majority of developing countries this value was between 1.3 and 2.2. In our study, even 6 studied health facilities had average number of drugs per encounter two or more (Fig. 1). It means that primary care health facilities suffer from tendency towards prescribing more drugs than absolutely necessary. Appropriate educational intervention would probably result with overall decrease in drug use. The intervention should not be in the form of lectures or one-day seminars, because this mode of education had been shown inefficient; the best way up to now is periodical composing, issuing and distributing adequate educational texts7. Development of national guidelines by some national medical body could be one solution to the problem; there are some successful examples, like guidelines in Scotland produced or supported by the Scottish Intercollegiate Guidelines Network8.
Percentages of drugs prescribed by generic name in our study (Fig. 2) were considerably lower than in majority of developing countries (>59%)3-6. It is caused by the type of the training medical students receive in Serbia. In medical schools they are tought to prescribe drugs by their registered names, not by generic names. In order to change this practice, an institutional intervention by ministries of health and education is necessary.
Percentages of encounters leading to the prescription of an antibiotic in our study were similar to figures observed in other developing countries (except the extremely high value of 63% in Sudan, all other countries had figures between 29% and 43%); yet, psychiatry and gastroenterology outpatient facilities had extremely low values (Fig. 3). The study conducted in Yemen suggested optimal theoretical value of 22.7%5. It seems that prescribing of antibiotics in outpatient facilities operating in city of Kragujevac could be further reduced, without adverse effect on quality of care. Extremely low prescribing of antibiotics observed in psychiatry outpatient facility is not surprising, considering specific pathology they deal with: infections of central nervous system are very rare cause of psychiatric disturbances in Balkan countries. On the other hand, in gastroenterology outpatient facility antibiotics were probably prescribed less than needed. More than 50% of patient encounters were made because of peptic ulcer or gastritis; considering importance of Helicobacter pylori eradication for healing of resistant peptic ulcers8, it is obvious that higher percentage of encounters should have had an antibiotic prescribed.
Our study showed that injections were prescribed optimally in Kragujevac (Fig. 4). Percentage of encounters with an injection prescribed was between 0 and 25%, which is close to optimal theoretical value proposed in Yemen study: 17.2%5. Although the cost of injection therapy is always much higher than the cost of oral therapy, further reduction in parenteral way of drug application is not possible without negative effect on quality of care.
Percentages of drugs prescribed from essential drugs list were much lower than values in developing countries (values in these countries are higher than 80%), especially in one of general practice facilities (Fig. 5). One of the reasons for such wrong practice is unavailability of copies of essential drugs list in all health facilities. Prescribing drugs from the essential drugs list issued by World Health Organization (WHO) means rational prescribing: the drugs from the list are older drugs, already tested in practice, with established clinical use and lower cost than newer drugs2. Ministry of health in Serbia should insist heavily in the future on introduction and following of the essential drugs list in each health facility for primary health care.
The average time, which a physician spends with a patient in studied health facilities, was within the limits of 2.8 to 7 minutes (Fig. 6). Such short time corresponded well with values measured in other developing countries (from 3 to 6.5 minutes)3-6. The opinion of WHO is that this time is too short to conduct complete patient evaluation and prescribe the therapy1. It is difficult to estimate optimal time period needed for the patient encounter, but the author believe that 30 minutes should be the lower limit for proper interaction.
In our study average dispensing time was similar among the pharmacies (between 18.4 and 33 seconds). It is somewhat longer than in Nigerian pharmacies (12.5 seconds), but far shorter than in Nepal pharmacies (86.1 seconds)9. We believe that this time is too short, without possibility for proper interaction between patient and pharmacist. About thirty seconds is far from enough to explain dosage regimen, adverse effects of a drug, all precautions, and to actually label and dispense a drug. It is clear that a patient compliance directly depends on his (or her) knowledge about the drug. We suggest to all pharmacists in city of Kragujevac prolongation of dispensing time as necessary step towards improvement of patient care.
Percentage of drugs actually dispensed significantly varies between pharmacies: the range was from 39% to 68% (Fig. 8). It means that there were differences in drug supply of pharmacies. Considering equal patient populations and equal needs for drugs, some changes in current supply practice should be made. Besides, overall percentages should be higher, like in other developing countries4,6,9, which implies increase in health budget in Serbia.
One major pitfall was found to be drug labelling practice. The WHO recommends that each drug label should contain dose regimen, drug name and patient's name1. In our study names of the patients were not written in the labels (except in two cases), and dose regimens were not written with all necessary details. Omission of patient's name on drug labels is a serious matter, with potentially serious consequences (drug misuse, drug abuse, and overdose).
Controversial results came up after investigation of the patients' knowledge of correct dosage (Fig. 9). The values were relatively high, but this does not reflect reality since the majority of the patients were hostile and not willing to repeat whole dose regimen in front of the investigator. Their responses "I know the dose" was accepted as positive answer, but it remains doubtful whether they really knew their dose regimens.
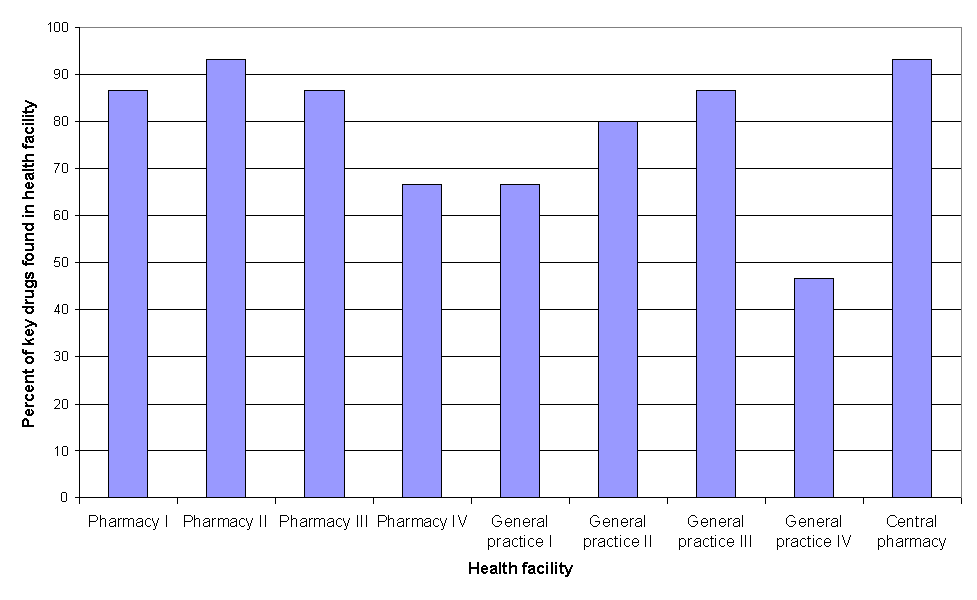
One notable characteristic of pharmacies in city of Kragujevac was their appropriate policy about the priorities in supplying drugs. The availability of key drugs in pharmacies was high (except in one general practice health facility), much higher than in other countries where the percentages were between 38% and 72% (Fig. 10). Such policy guarantees at least a minimum of health care.
Figure 1. Average number of drugs per encounter.
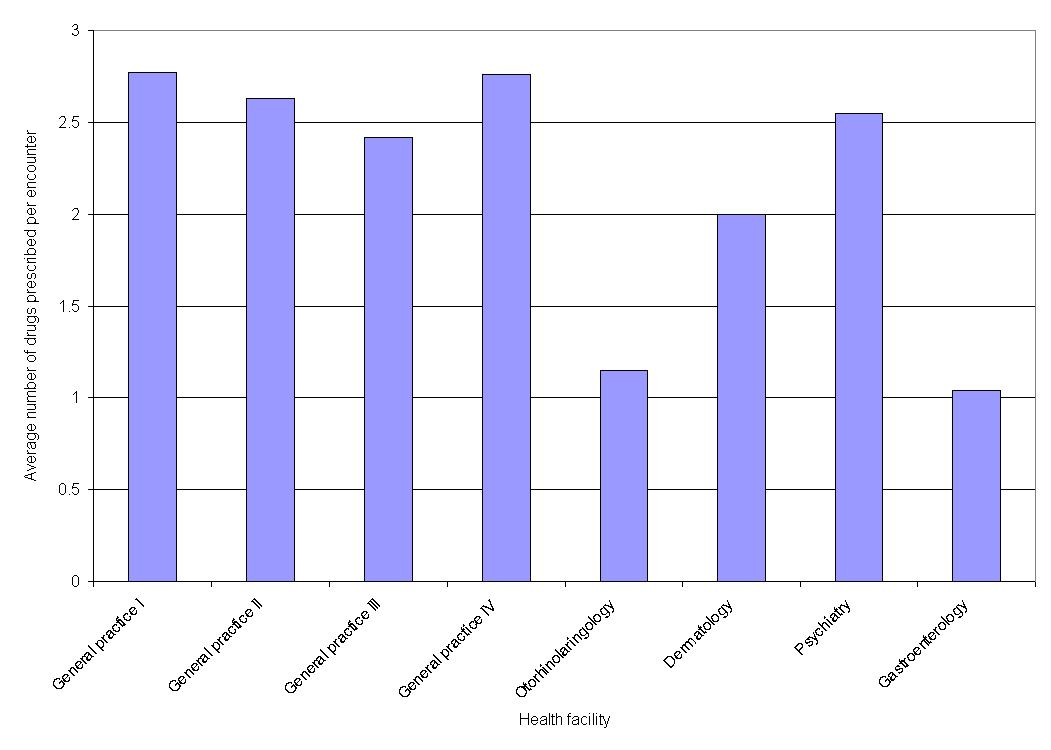
Figure 2. Percentage of drugs prescribed by generic name.
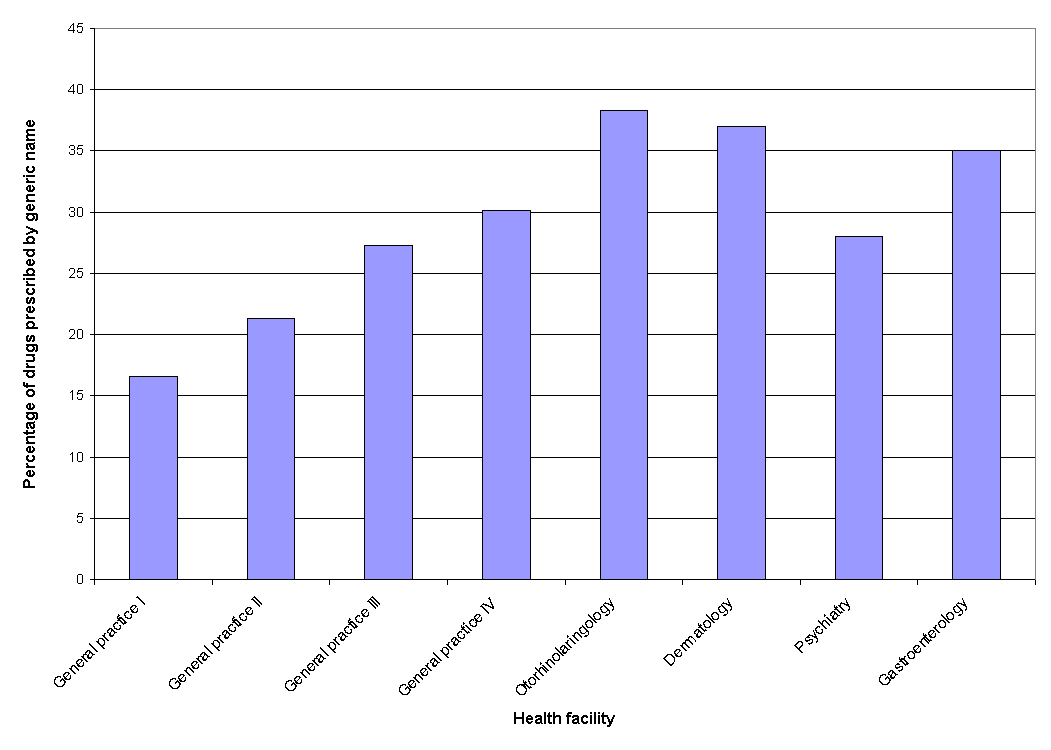
Figure 3. Percentage of encounters with an antibiotic prescribed.
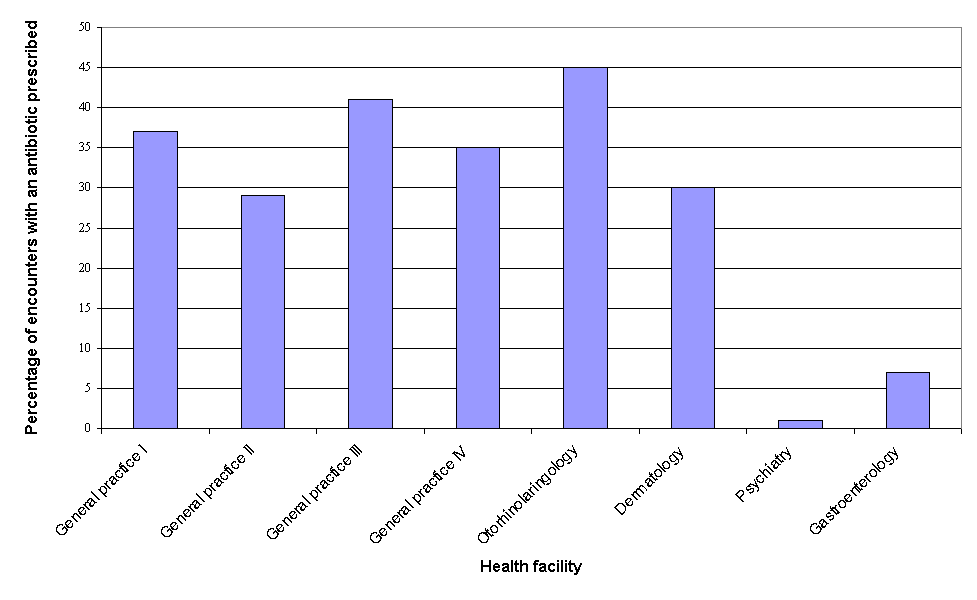
Figure 4. Percentage of encounters with an injection prescribed.
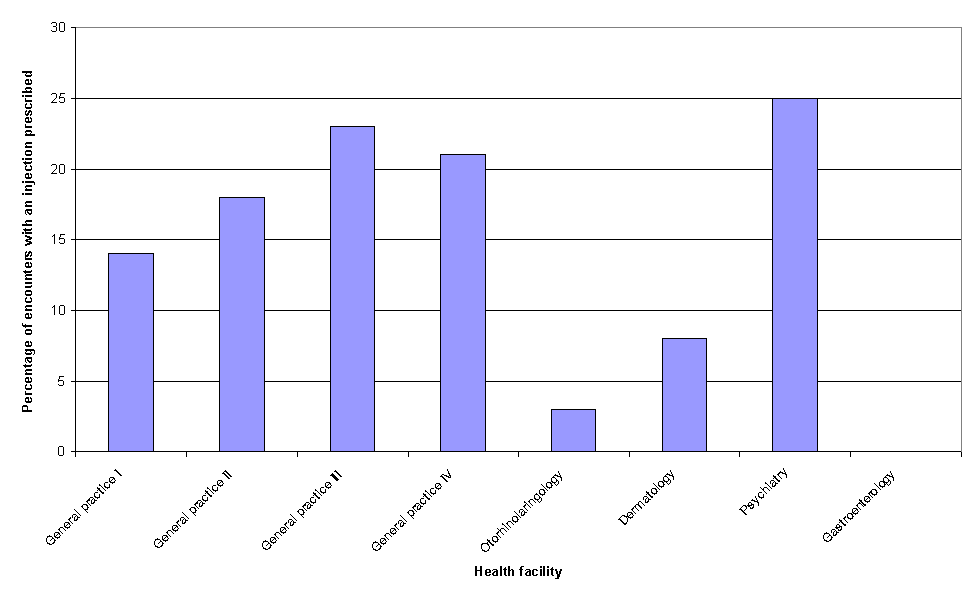
Figure 5. Percentage of drugs prescribed from essential drugs list.
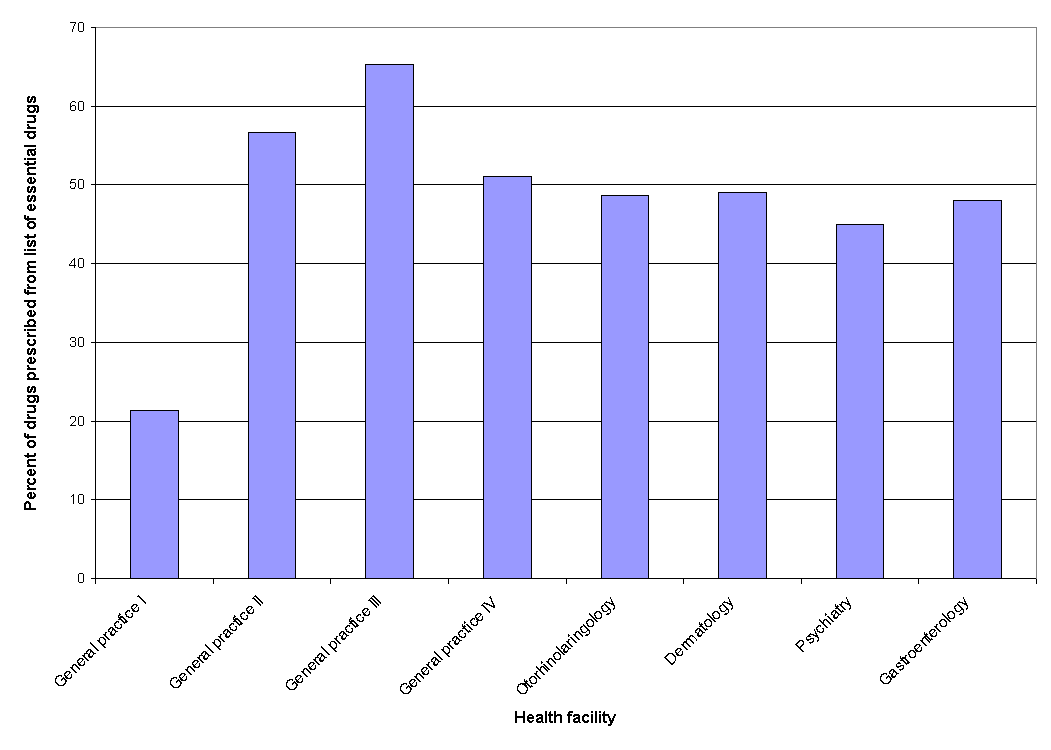
Figure 6. Average consultation time.
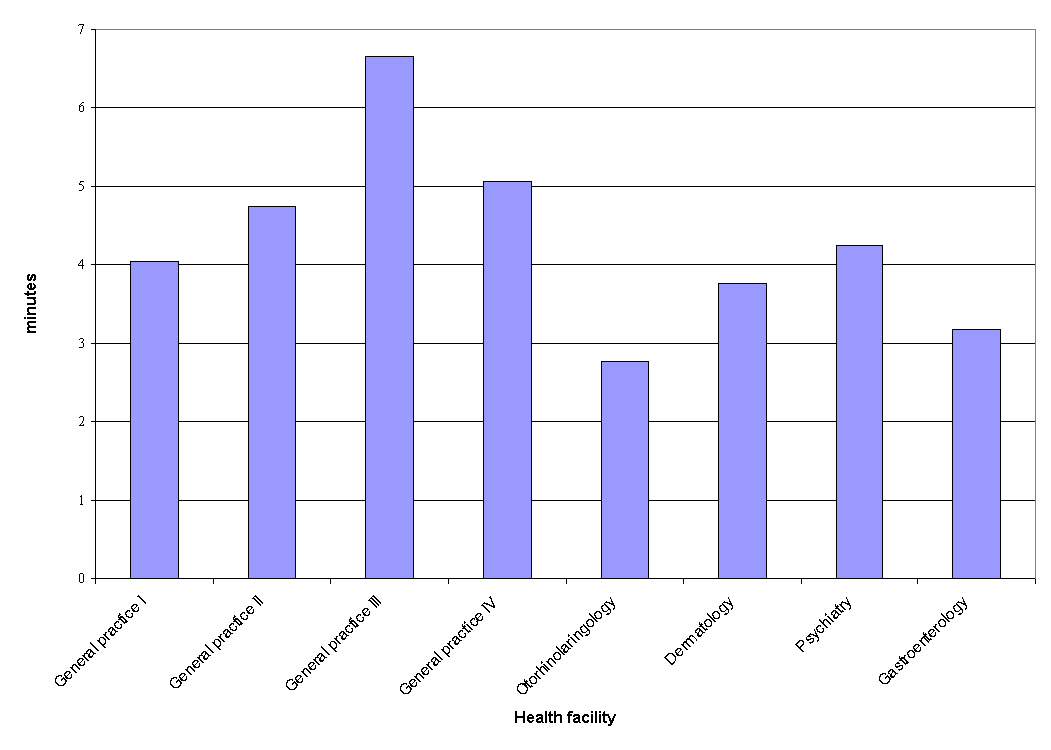
Figure 7. Average dispensing time.
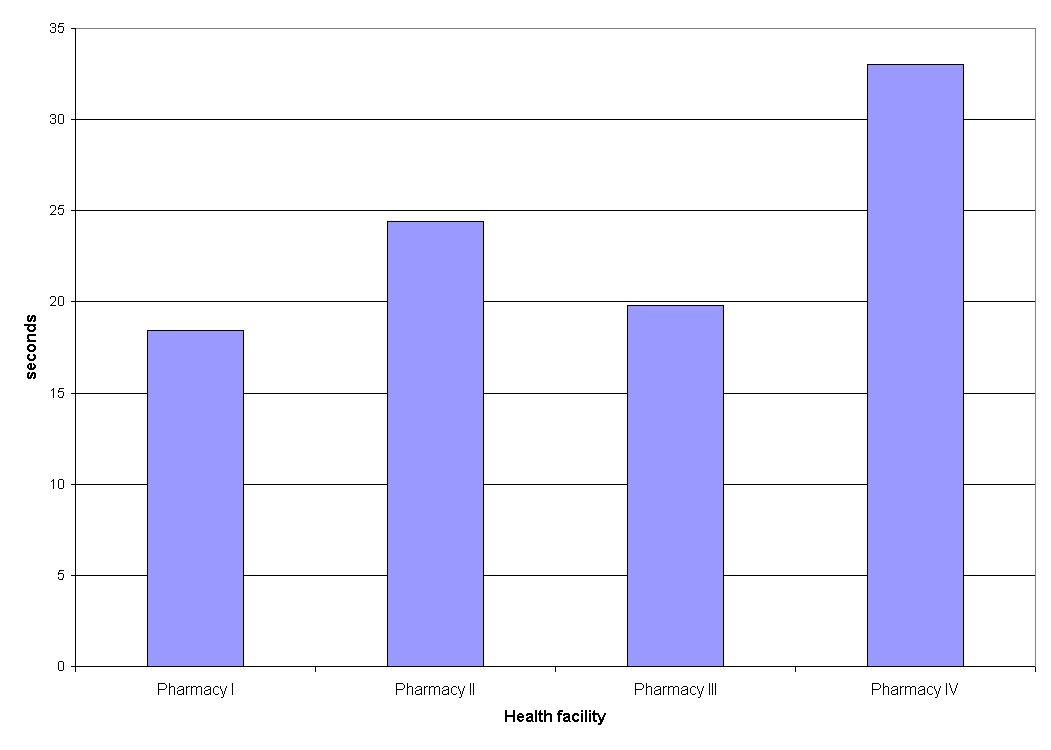
Figure 8. Percentage of drugs actually dispensed.
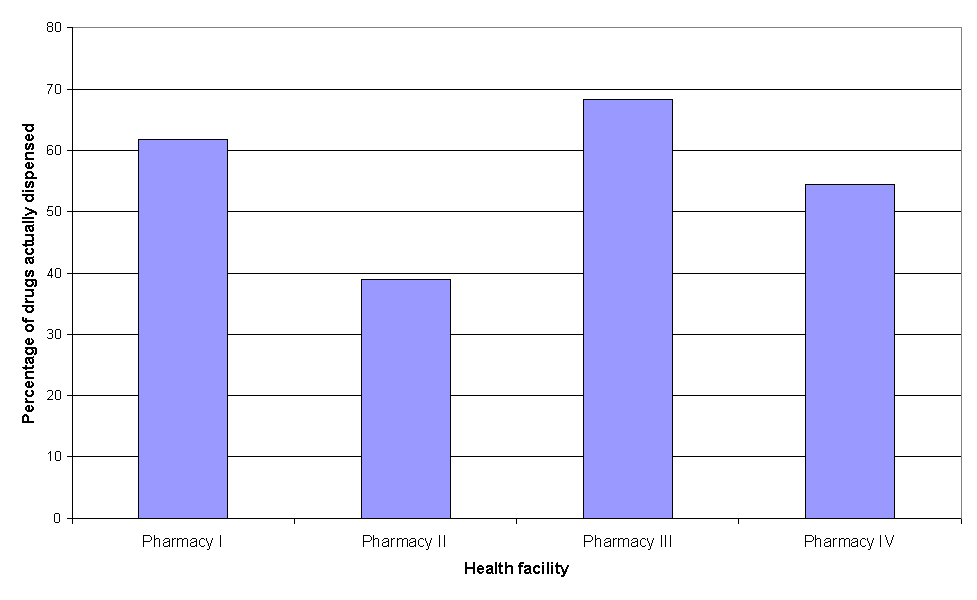
Figure 9. Patients' knowledge of correct dosage.
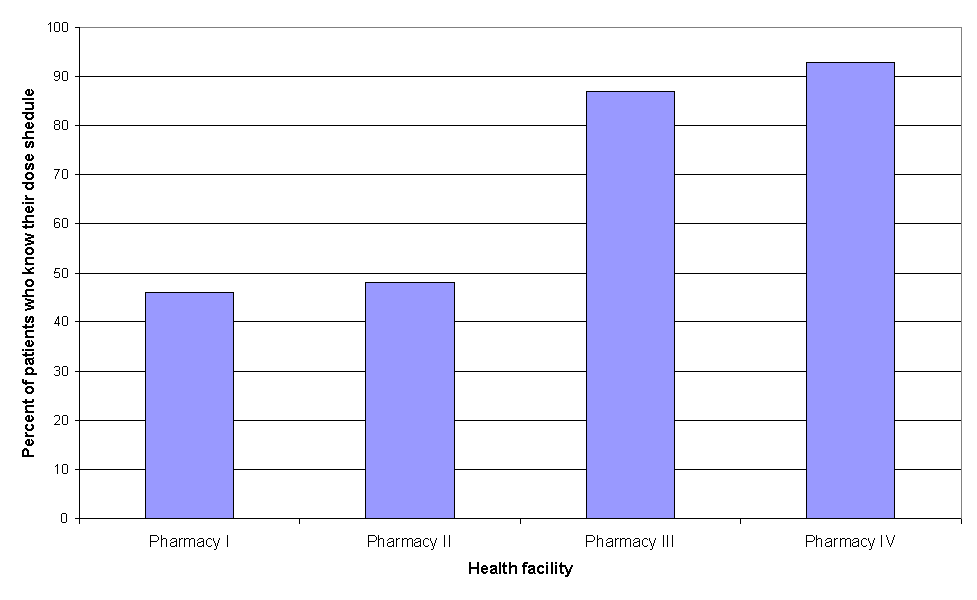
Figure 10. Availability of key drugs.