Browse through our Journals...
SURGICAL MANAGEMENT OF CONGENITAL MALFORMATIONS IN RUMINANTS
MAGDA M. ALI & H.A. YOUSSEF
Department of Surgery, Faculty of Veterinary Medicine, Assiut University
Assiut, Egypt
SUMMARY
Congenital malformations recorded in 71 ruminants, including calves, lambs and kids, were retrospectively reviewed. There were 15 atresia ani, 10 atresia ani et recti, 2 atresia ani with vaginal and bladder agenesis, 11 anus vaginalis, 3 persistent cloaca, one persistent cloaca with spinal agenesis, 11 persistent urachus, 7 urethral diverticulum, 8 omphalocele and 3 meningoceles. Surgical treatment for such conditions was carried out after the differential diagnosis. The development of these congenital malformations, their effect on the animal life and the different surgical interventions were discussed
INTRODUCTION
Congenital defects, abnormalities of structure or function present at birth, may be caused by genetic or environmental factors, or a combination of both; in many cases, the causes are unknown. Developmental defects may be lethal, semi-lethal, or compatible with life causing aesthetic defects or having no effect on the animal (Johnson et al, 1985). Susceptibility to agents that affect development varies with fetal stages, but in general decreases with gestational age. Before day 14 of gestation in cattle (period of pre-attachment), the zygote or embryo is resistant to agents that can cause congenital malformations (teratogens) but is susceptible to genetic mutations. During the embryonic period (day 14-42), the embryo is highly susceptible to teratogens, but this decreases with embryonic age, as the critical periods for the formation of various organs are passed. The fetus (Day 42) becomes increasingly resistant to teratogenic agents with age, except for the late differentiating structures, e.g. cerebellum, palate and urogenital system (Johnson et al.; 1985 and Aiello 1998).
A concise description of congenital malformations observed in this study is reported here:
Atresia ani, (imperforated anus), is the failure of the anal membrane to break down. The rectum is intact and attached to the membrane. Atresia ani is most frequently encountered in calves and pigs. If the rectum ends blindly as a cul- de sac a short distance cranial to the anal membrane, the condition is called rectal atresia (Noden and Lahunta 1985).
Anus vaginalis is the anomaly in which an abnormal opening exists between the terminal rectum and the vagina. The anus may be partially developed or lacking and feces are evacuated through the vulva. Lack of the anus, rectum or small colon is an inherited lethal abnormality. It appears uncommon in the general population but with a relatively high incidence in certain cross-breeds (Oehme and Perier 1974).
Atresia ani with vaginal and urinary bladder agenesis. In the literature available to these authors there is a lack of record regarding this anomaly with the exception of experimentally induced anomalies in animal models. Bladder agenesis was an important feature in the adriamycin animal model. Bilateral hydro-nephrosis resulted from blind-ending ureters (Merei et al. 2001).
Persistent cloaca and caudal spinal agenesis in calves were described by Dean et al. (1996). The persistent cloaca results from failure of the urorectal septum to develop. It is lined by a mixture of transitional and colonic epithelium. The association of persistent cloaca and caudal spinal anomalies is thought to be related to cell loss in the caudal cell mass, which affects caudal spinal column formation and cleavage of the cloaca by the urognital septum.
Persistent (pervious, patent) urachus is often conceived to be the result of a failed occlusion due to some congenital defects of the urachus or of the umbilical ring. Navel infection was reported to be interpreted as either the cause or the effect of the open urachus (Oehme and Perier 1974). Normally the urachus closes and degenerates along the border of the median ligament of the bladder. If it remains open, urine will be excreted from this tube at the umbilicus and the condition will be called persistent urachus or urachal fistula. This fistula is a source of infection to the bladder. Persistence of only the distal end of the embryonic allantoic stalk at the umbilicus creates an urachal umbilical sinus. Persistence of the proximal urachus at its union with the bladder creates a vesicourachal diverticulum that may be a site of chronic cystitis (Noden and Lahunta 1985).
Omphalocele is a congenital defect in the body wall in which eviscerated abdominal organs are covered by amnion rather than skin (Baird 1993).
Meningocele is the protrusion of the membranes of the brain or spinal cord through a defect in the skull or spinal column. The sac of the meningocele is composed of more or less complete outer layer of skin over an irregular layer of dense collagenous tissue mixed with various amounts of fat. The inner lining of the meningocele is a thin, smooth layer of flattened cells (Rosai 1981). Meningocele was described in calves by Jeffry et al., (1990), in foals by Van Hoogmoed et al., (1999), in dogs by Samuelson and Dennis (1979) , in cats by Sponenberg and Webster (1986) and in swines by Vogt et al., (1986).
The present study aimed to discuss the differential diagnosis and surgical management of the prevalent surgical malformations in farm animals
MATERIALS AND METHODS
Differential diagnosis was followed by surgical treatments in some congenital malformations of calves, lambs and kids. Surgeries were performed under locally infiltrated analgesia using Lidocaine Hcl 2%. Rompun (Bayer) was used intramuscularly for pre-operative tranquillization at doses of 0.1 mg/kg in calves and lambs and 0.05 mg/kg in kids.
Atresia ani was treated by excision of a circular piece of skin. The blind end of the rectum was stitched to the circular skin opening by four stitches (dorsally, ventrally and on both sides). The tip of the blind end of the rectum was snipped to evacuate the contents. The circumference of the rectal opening was sutured to the skin opening.
Atresia ani et recti was treated by making an anus preternaturalis. A midventral prepubic laparotomy was performed and the colon was sutured to the caudal part of the laparotomy wound. The bowel wall was opened after completion of suturing.
Anus vaginalis was treated by performing an artificial opening at the site of the normal anus. The index finger of the left hand was introduced into the blind rectal end through the rectovaginal opening and was directed caudally to make a skin bulge to mark the opening site. An artificial anus was then performed. The rectovaginal opening was closed through the anal opening. Its brim was incised circumferentially and the opening was closed transversally using No. 0 chromic catgut in an interrupted pattern. The sutures did not include the rectal mucosa.
Atresia ani with vaginal and urinary bladder agensis was diagnosed in a female buffalo calf.
Persistent cloaca was treated in two cases, the swelling was incised longitudinally and the contents were evacuated. The redundant wall of the cloacal swelling was excised leaving a part sufficient to make anal and vulval openings.
The mucosa between the anal and vaginal openings was incised transversally and dissected up and down to make a floor for the rectal opening and a roof for the vaginal opening. The skin from both sides was sutured to cover the bared area between the two openings.
In one case of persistent cloaca with caudal spinal agenesis, the redundant wall of the swelling was excised and the mucosa was sutured to the skin making a common opening for both the rectal and vaginal openings.
Persistant urachus was treated by a fusiform laparotomy incision around the umbilicus which was resected along with the urachus. In two cases the urachus was double ligated and excised close to the bladder. The stump was inverted by sutures in the other cases the urachal wall was excised as much caudad as possible. The aperture was closed by double raw of inverting lembert's sutures.
Urethral diverticulum was treated in seven kids. Free drainage of urine was performed by a considerable incision of the swelling ventrally in the dependent part.
Omphaloceles were treated by excision of their wall. The abdominal wall was trimmed and closed by sutures. The cases of ruptured omphalocele with severe gross contamination of the abdominal cavity and/or intestinal strangulation were euthanized
The meningocele was excised by a fusiform skin incision. Dissection was continued to the base of the meningocele. It was ligated and the swelling was excised. The subcutaneous tissue was closed with simple continuous catgut sutures and skin with simple interrupted silk sutures.
RESULTS
Seventy-one congenital malformations were recorded: 15 atresia ani, 10 atresia ani et recti, 2 atresia ani with vaginal-urinary bladder agenesis, 11 anus vaginalis, 3 persistent cloaca, 1 persistent cloaca-caudal spinal agenesis, 11 persistent urachus, 7 urethral diverticulum, 8 omphaloceles and 3 meningocele (Table 1).
|
Affliction |
Calves |
Lambs |
Kids
|
Total |
|||
male |
female |
male |
female |
male |
female |
||
Atresia ani |
7 |
1 |
4 |
___ |
3 |
___ |
15 |
Atresia ani et recti |
10 |
___ |
___ |
___ |
___ |
___ |
10 |
Atresia ani with vaginal and bladder agenesis |
___ |
1 |
___ |
____ |
___ |
1 |
2 |
Anus vaginalis |
___ |
5 |
___ |
6 |
___ |
___ |
11 |
Persistant cloaca |
___ |
3 |
___ |
___ |
___ |
___ |
2 |
Persistant cloaca with spinal agenesis |
1 |
___ |
___ |
____ |
___ |
___ |
1 |
Persistant urachus |
5 |
6 |
___ |
___ |
|
___ |
11 |
Urethral diverticulum |
___ |
___ |
___ |
___ |
7 |
___ |
7 |
Omphalocele |
___ |
___ |
1 |
2 |
|
5 |
8 |
Meningeocele |
2 |
___ |
___ |
1 |
___ |
___ |
3 |
Summation |
25 |
16 |
5 |
9 |
10 |
5 |
71 |
Atresia ani was recorded in 15 males (7 cattle calves, 4 lambs, 3 kids) and 1 female cattle calf. There was no anal opening, but a bulge at its site. The size of the bulge increased with induced distension of the abdomen by hand pressure on the abdomen (Fig. 1). Excision of a circular piece of skin about two cm. in diameter in calves and about one cm. in diameter in lambs and kids facilitated undermining of the blind end of the rectum. Stitching of the blind end of the rectum before its opening by four stitches (dorsally, ventrally and on both sides), minimized the subcutaneous contamination. The circular skin opening promoted free evacuation (Fig. 2).
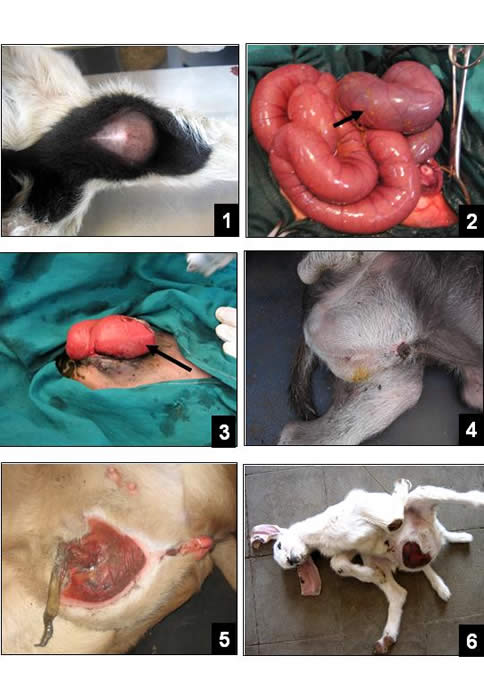
LEGENDS OF FIGURES
Fig. 1: A bulge at the anal site indicating the imperforated anus in a lamb
Fig. 2: The evacuation of the intestinal contents after incising the anal membrane
Fig. 3: The distal part of the colon which will be sutured to the laparotomy wound in a cattle calf with atresia ani et recti (black arrow)
Fig. 4: Atresia ani with vaginal and urinary bladder agenesis in a cattle calf
Fig. 5: Anus vaginalis in a lamb
Fig. 6&7: Persistent cloaca in a kid, and the contents inside the swelling
Fig. 8: Persistent cloaca with caudal spinal agenesis in a cattle calf
Fig. 9: The fusiform appearance of the persistent urachus (white arrow)
Fig. 10: Double ligature of the persistent urachus to separate it from the bladder
Fig. 11: urethral diverticulum with several swellings in a kid
Fig. 12: Evacuation of the urethral diverticulum contents
Atresia ani et recti was recorded in 8 male cattle calves. There was neither anal opening nor bulge at the anal site even with hand pressure on the distended abdomen. The distal part of the colon could be lodged via a mid ventral prepubic laparotomy (Fig. 3). A segment was confined toward the end of the laparotomy incision. The incision was closed leaving a part for the colon segment which was sutured circumferentially with seromuscular sutures to the left. The colon was incised and the edges were sutured to the skin to develop an anus preternaturalis. The intestinal contents were mostly gaseous in three cases. These three cases died within two days postoperatively. The other five cases were followed up for three months. Only one case returned 45 days postoperatively with partial colon prolapse (Fig. 4). It was treated by narrowing of the anus pernaturalis. The other cases had no complains.
Atresia ani with vaginal and urinary bladder agenesis was diagnosed in a newly born buffalo calf (Fig. 5) and a newly born kid (Fig. 6). The calf had a massive congenital ventral abdominal hernia. The vulva was absent where a skin ridge was noticed instead of it. The blind end of the rectum was lodged about 2 cm from the skin surface. Ventral laparotomy revealed absence of the vagina, the urinary bladder and the urachus. The uterus and the ovaries were evident and appeared enlarged and hyperaemic. The kid had a massive congenital ventral abdominal hernia. It had two abnormal hind legs in addition to the normal ones (Fig. 6). Euthanasia was advised.
Anus vaginalis was diagnosed in 11 females (5 cattle calves and 6 lambs). Incomplete evacuation and abdominal distension rather than the absence of the anal opening were the signs which drawn the attention of the owner to seek the surgical treatment. The abnormal opening between the terminal rectum and vagina was about 2 cm from the perineal skin and with a diameter that could permit the passage of only the index finger (Fig.7).
The vaginal diameter was too small to enable suturing of the recto-vaginal opening. It was sutured through the induced anal opening. The rectal mucosa was dissected and elevated along the brim of the opening of the fistula. The opening was closed by inverting sutures which did not include the rectal mucosa. After closure, the rectal mucosa appeared as a covering non-sutured protecting layer.
Persistent cloaca was recorded in three cattle calves. There was an oval swelling filled with a mixture of urinary and fecal excreta (Figg. 8 & 9). Incision of the swelling and evacuation of the content revealed separate rectal and vaginal openings in two cases. The redundant tissues were excised to form separate anal and vulva openings. After construction of the two openings, the bared area between them was then covered by a skin from both sides. The third case had a common opening for the urinary and digestive excreta (Fig. 10).
Persistent cloaca and caudal spinal agenesis was recorded in one cattle calf (Fig. 11). There was a common channel for the rectal and urogenital passages. The redundant wall of the cloacal swelling was excised and the mucosal lining was sutured to the skin around the common opening.
Persistent urachus was diagnosed in 11 cattle calves (5 males and 6 females). Edema, suppuration and inflammatory signs of the umbilical region were evident in 3 cases. The signs were intermittent dribbling of urine and wetness of the hairs in the umbilical area. Inversion of the skin around the urachal opening by a continuous inverting suture offered protection against contamination especially in infected cases. The narrow fusiform incision around the umbilicus enabled safe dissection, isolation and excision of the infected umbilicus along with the urachus.
The index finger of the left hand gave a protective guide for the laparotomic incision around and caudal to the umbilicus. The persistent urachus was about the size of the index finger in four cases (Fig. 12). It was resected after double legation closer to the bladder wall. The stump was inverted by one raw of Lembert's inverting chromic catgut sutures. In the 7 remaining cases, the enlarged urachus was in the shape of a cone where its base merged with no definite demarcation with the bladder wall. The urinary bladder appeared elongated to attach the umbilicus (Fig. 13).
Fig. 13: An omphalocele in a kid
Fig. 14: the omphalocele contained only a fibrosed umbilical cord
Fig. 15: Meningocele in a cattle calf
Fig. 16: Opening of the meningocele and evacuation of its content
Fig. 17: An opened omphalocele (the prolapsed viscera was strangulated and massively contaminated)
Fig. 18: A meningocele in a cattle calf
Amputation was done as caudal as possible, after placing sutures to hold the bladder and packing the abdominal cavity with moist towels to protect the viscera. Watertight closure of the bladder wall was done by double raw of inverting Cushing sutures using catgut size zero.
Urethral diverticulum was detected in 7 kids. The penile urethral diverticular extension was ovoid in four cases and ovoid with multiple swellings pre and post scrotal in two cases (Fig. 14). Exploratory puncture gave urine. It was tender when the diverticular swelling was pressed where urine came from the normal urethral opening. Free drainage of urine was obtained, by a considerable incision of the swelling ventrally leaving no gap distally (Fig.15).
Omphalocele was recorded in 8 cases; 5 female kids and 3 lambs (one male and two females). It was closed in 5 cases (Fig. 16). Excision of the wall of closed omphalocele sac and exploration of the herniated viscera could be done through a narrow fusiform abdominal incision. The left index finger offered a protective guide to complete the incision. In one case, the omphalocele contained only the umbilical cord (Fig. 17). The omphalocele was opened and the prolapsed viscera were fresh without detectable gross contamination in one case. The abdominal opening was trimmed and excised with the omphalocele sac and the prolapsed viscera was flushed with warm saline solution and reduced into the abdomen. The abdomen was closed after topical application of penicillin. Two cases were euthanized because the prolapsed viscera were strangulated and massively contaminated.
Meningocele was diagnosed in 3 animals (a lamb and two cattle calves) in the occipito-cervical region (Fig. 18). Gentle palpation and exploratory puncture revealed that the prolapsed part contained a cerebrospinal fluid. Dissection of the swelling through a narrow fusiform skin incision revealed that the base was connected to the neural canal. The catgut ligature around the base of the meningocele provided a safe protective measure for the neural canal before excision of the meningocele. Median section of the excised swelling showed that the cerebrospinal fluid was filling half of the swelling. The subcutaneous tissue was closed with simple continuous patterns using chromic catgut sutures and the skin with simple interrupted patterns using silk sutures.
DISCUSSION
Congenital defects and abnormalities presented in this study were recorded as sporadic cases originating from different geographic sites in Egypt. Therefore these animals probably might be subject to different genetic and/or environmental factors. Most congenital malformations were recorded with variable frequencies, in farm animals. Atresia ani and persistent urachus were recorded only in calves whereas urethral diverticulum was diagnosed only in kids. Atresia ani was most frequent in males. Atresia ani et recti was recorded only in males. Atresia ani with vaginal-urinary bladder agenesis may be considered the first naturally occurring case recorded in buffaloes and in the domestic animals as well. Only experimentally induced cases are recorded in rats (Merei et al, 2001).
Treatment of atresia ani by excision of a circular piece of skin facilitates dissection of the blind end of the rectum, and its fixation by stay sutures to the skin opening minimizes contamination of the subcutaneous tissue.
Ventral colostomy was an effective treatment for atresia ani et recti. The sero-muscular sutures of the colon segment to the abdominal wound provided a safe measure against contamination of the peritoneal cavity in such cases. However, when the intestinal contents are gaseous the prognosis is usually fatal. The cause may be an undetected occlusion hindering the passage of the intestinal contents.
No treatment was tried for atresia ani with vaginal and urinary bladder agenesis.
Closure of the recto-vaginal fistula in cases of anus vaginalis may be easier by accessing through the anal opening. The transverse closure was preferred in order to avoid the effect of the transverse tension on the sutures due to rectal distension during defecation. The circumferential dissection of the mucosa provided a raw sub-mucosal surface for effective closure. The non sutured mucosa provided a protective covering layer for the suture line. This technique is simple and avoids the more invasive transverse perineal approach.
Cases of persistent cloaca without caudal spinal agenesis are accompanied by two separate channels for fecal and urinary excreta. On the contrary, In this study only one channel was found in a similar case. It was difficult and uneconomic to separate the two channels. Pena and Levitt (2003) and Pena et al. (2004) discussed the technique, risks and complications of the surgical management of cloacal malformations in infants.
Most cases of persistent urachus have a wide lumen with no obvious demarcation between the urinary bladder and urachal tissues. Therefore, the surgical excision was the appropriate treatment. Cauterization of the umbilical opening of the urachus (Oehme and Perier 1974) might be considered as unsuitable approach.
Urethral diverticulum was found only in kids in this study. Generally, it was large in size affecting most of the penile urethra. Performing a wide urethral fistula was an acceptable treatment for these animals in order to obtain a longer survival time.
Omphalocele was described in a male Arabian foal at birth. The mass contained was the small intestine. On the outside there was a hairless pink membrane. The internal part contained also the umbilical artery and vein and a large urachus that extended from the bladder to the opening at the extremity of the mass (Steinman 2000). Excision of the omphalocele sac and exploration of the viscera may be necessary before closure of the abdomen. Massive gross contamination and/or severe visceral strangulations may be an indication for euthanasia of the animals.
REFERENCES
Oehme FW, and Prier JE Text book of large animal surgery: Williams & Wilkings, Baltimore/ London, 1974; 425-509
Noden DM, Lahunta A the embryology of domestic animals, developmental mechanisms and malformations: Williams & Wilkins, London, 1985; 306-315
Adamu SS, Mohammed A, Egwu GO, et al. Patent urachus with a perforated urethra in Nigerian balami Lamb. Vet. Rec 1991; 12, 129 (15): 338-340
Suess Rp, Martin RA, Moon ML, et al. Rectovaginal fistula with atresia ani in three kitten, Cornell Vet., 1992; 82 (2): 141-153
Barid AN, Omphalocele in two calves, J. Am. Vet. Med. Assoc. 1993; 1, 202 (9): 1481-1482
Saperstein G, Congenital abnormalities in internal organs and body cavities, Vet. Clinic. North. Am. Food animal. Pract. 1993; 9 (1): 115-125
Dean CE, Cebra CK, Frank AA, Persistent cloaca and caudal spinal agenesis in calves: Three cases. Vet. Pathol. 1996; 33 (6): 711-712
Steinman A, Kelmer G, Avin G Omphalocele in a foal. Vet. Rec. 2000; 18, 146 (12); 341-343
Flock M, Ultrasonic diagnosis of inflammation of the umbilical cord structures, persistent urachus and umbilical hernia in calves. Berl. Munch. Tierarzt Wochenschr. 2003; 116 (1-20):2-11
Noh DH, Jeong WI, Lee CS, et al. Multiple congenital malformations in a Holstein calf. J. Comp. Pathol. 2003; 129 (4): 313-315
Ghanem M, Yoshida C, Isobe N, et al. Atresia ania with diaphallus and separate scrota in a calf: A case report. Theriogenology 2004;16 (7-8): 1205-1213
Corbera JA, Arencibia A, Morales I, et al. Congenital duplication of the caudal region (monocephalus dipygus) in a kid goat, Anat. Histol. Embryol. 2005;4 (1) 61-63
Weaver ME, Persistent urachus, an observation in miniature swine. The anatomical record 2005; 154 (3): 701-703
Merei J, batiha A, Hani IB, et al. Renal anomalies in the VATER animals. J. Pediatr. Surg. 2001; 36 (11): 1693-1697
Rosai MD Surgical pathology, Vol. 2. The C. V. Mosby Company, London, 1981; 1556-1557
Jeffrey M, Preece BE, Holliman A, Dandy- Walker malformation in two calves, Vet. Rec. 1990; 19, 126, (20) 499-501
Van Hoogmoed L, Yarbrough TB, Hornof WJ Surgical repair of a thoracic meningeocele in a Foal. Vet. Surg. 1999; 28 (6): 496-500
Samuelson ML, Dennis SM Cleft palate associated with meningocele in a pup. Vet. Rec. 1979; 12, 104 (19): 436-440
Sponenberg DP, Graf-Webstr E Hereditary mening-encphalocele in Burmese cats. J. Hered 1998; 77 (1): 60-65
Vogt DW, Ellersieck MR, Deutsch WE, et al. Congenital meningeocele-encephalocele in an experimental swine herd. J. Am. Vet. Res. 1986; 47 (1): 188-191
Johnson JL, Leipold TT, and Hudson DB Prominent congenital defects in Nebraska beef cattle. Breeding and reproduction, 1985; 4 (7): 1-8
Aiello SE, Congenital and inherited anomalies; The Merk veterinary manual, 8th ed, New Jersy, USA, Merk & Co., Inc., Whitehouse station, 1998; 449- 455
Pena A, Levitt A, Surgical management of cloacal malformations. Semin Neonatol, 2003; 8 (3): 249-257
Pena A, Levitt A, Hong A, et al. Surgical management of cloacal malformations: a review of 339 patients, J. Pediatr. Surg. 2004; 39 (3): 470-479
Copyright © Priory Lodge Education Limited 2007
First Published July 2007
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


