Browse through our Journals...
Tactile Hallucinations associated with Clonidine
Hayden, Tiburcio, Cepin, Lanka
Case
A 4 y/old black male with a history of attention deficit-hyperactivity disorder combined type (ADHD) and oppositional defiant disorder (ODD) diagnosed at age and successfully treated with methylphenidate ER (Ritalin LA) 10 mg daily, prescribed by a neurologist in a separate clinic. Due to allegations of physical abuse and emotional difficulties attributed to his mother, he was placed in foster care for 8 months. At this time, he received no medication. According to his mother, he “came back acting worse,” and fears that he had been maltreated in foster care. Upon return to the mother, he was brought to our clinic to resume treatment. His family consisted of the mother and an 8-year old sister. They live in a one bedroom apartment in a public shelter complex.
A complete and careful evaluation consisting of the current psychological milieu and maternal relational pattern was performed before confirming the diagnoses of ADHD and ODD. The patient was noted to have normal development, was verbally precocious, quite bright and well-related. Due to continued (and according to the mother worsening) aggressive, hyperactive and impulsive behavior, he was restarted on methylphenidate extended release 10 mg daily.
Two weeks later, his symptoms worsened markedly, espeically with aggression in the form of scratching, hitting and biting his mother. Methylphenidate was discontinued, and a trial of clonidine 0.05 mg tid was started, with a partial response. The patient was reevaluated 3 days later and clonidine was titrated up to 0.1 mg twice daily and at bedtime.
Eleven days after onset of treatment, the patient began to show signs of early and middle insomnia. He woke up in the middle of the night and told his mother that the television is on. Twenty four hours later he began to have sudden of feeling of fright. Furthermore, he was screaming and crying to his mother that something was biting him in the legs as he frantically tried to remove his clothes. This symptom would last for a few minutes and was intermittent over 48 hours. As a result, his mother brought him back to the clinic.
Shortly after their arrival to the clinic, the treating team witnessed a dramatic scene, as the patient experienced extreme fright and screamed that “the bugs are in my pants!” while gyrating and attempting to pull off his underwear. At this time his mother tried to comfort him while trying to keep his clothes on. He has had no prior episodes of hallucinations. However his mother has a history of mood disorder on medication. She reported that she had faithfully given him his medication as prescribed and not given him methylphenidate since discontinuation. Clonidine was stopped and was placed on risperidone 0.25 daily for four days. Subsequently the dose was increased to 0.5 mg bid with a good response. Three weeks later, the mother stopped risperidone, and noted return of hyperactive and oppositional symptoms but no hallucinations over the following 3 months of follow up.
Discussion
Clonidine, an alpha 2 noradrenergic receptor agonist (See Figure 1), is often used as an adjunctive or second line therapy for the treatment of ADHD. It has been used for ADHD despite the lack of a well-controlled, double blind studies to examine the drug’s efficacy.
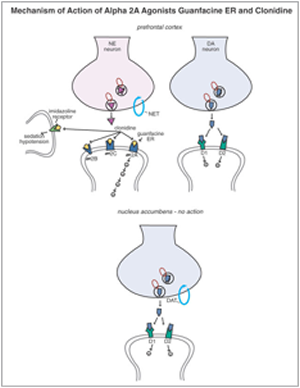
Figure 1: Mechanism of Action of Guanafacine ER and Clonidine7
Although clonidine and its relative guanafacine have not been approved for ADHD, there have been reports and small case studies supporting the role of these two drugs in clinical situations such as high reactivity, impulsivity, aggression, post-traumatic symptoms, insomnia and tics especially in pre-school age patient. A randomized controlled trial adding clonidine to an ongoing psychostimulant therapy for children with ADHD and co morbid ODD or conduct disorder was conducted in 20034. Although statistically not significant, there was an improvement in symptoms. However, its effects wore off in 6 weeks. Clonidine can be considered as an acceptable alternative in cases where psychostimulants have proven ineffective or are not well tolerated.
The most common adverse effects of clonidine include dry mouth, dizziness, fatigue and sedation. One of the rare side effects include atrioventricular block. Rebound hypertension is of concern with sudden discontinuation. Four cases of adverse events including sudden death associated with clonidine being used in combination was reviewed in a case study3. Due to confounding variables it was not possible to determine the role of clonidine in these adverse events. Although there was no previous documentation of tactile hallucinations, auditory and visual hallucinations were listed as side effects in the prescribing information for clonidine5. “Acute organic mental disorder” was also cited but tactile hallucinations were not mentioned1. On the other hand, tactile and other somatic hallucinations are now fairly well-recognized possible side effects of psychostimulant medication even at therapeutic doses which will manifest during upward dose titration6. Guanfacine has also been reported to be associated with hallucinations2.
In our patient, tactile hallucinations started on day 11 of being on clonidine. The time course of symptom onset and prompt resolution of symptoms after discontinuation strongly identified clonidine as the cause of his tactile hallucinations. Other possibilities would include surreptitious administration of a stimulant medication and benign phobic hallucinations. The psychopharmacological mechanism of clonidine leading to this adverse reaction is difficult to determine since its primary mechanism is to dampen the noradrenergic arousal. However, the psychopharmacological effects of methylphenidate and other psychostimulants can be explained by the interactions with the dopamine system. It is possible that there could be an acute rebound of adrenergic tone between doses of clonidine. This in turn can stimulate arousal to a level that could trigger complex sensory phenomena such as tactile hallucinations. Based on this report and other findings, clinicians should be aware of the hallucinatory side effects when prescribing alpha 2 agonists.
Francis Hayden, MD
Psychiatry Attending, Bronx Lebanon Hospital Center
Jose Tiburcio, MD
Family Medicine Attending, Bronx Lebanon Hospital Center
Kayra Cepin, MD
Family Medicine Resident (PGY3), Bronx Lebanon Hospital Center
Himabindu Lanka, Student Doctor
Ross University School of Medicine
References
- Allen RM, Flemenbaum, A. Delirium associated with combined fluphenazineclonidine therapy. J Clin. Psychiatry: Volume 40, Part 5, May 1979, Pages. 236-237. 1979.
- Boreman CD, Arnold LE, Hallucinations associated with initiation of guanfacine. J of Am Acad Child Adolescent Psychiatry: Volume 42, Part 12, December 2003, Page 1387.
- Cantwell DP, Swanson J, Connor DF. Case study: Adverse response to clonidine. J of Am Acad Child Adolescent Psychiatry: Volume 36, Part 4, April 1997, Pages 539-544.
- Hazell PL, Stuart JE. A randomized controlled trial of clonidine added to psychostimulant medication for hyperactive and aggressive children. J of Am Acad Child Adolescent Psychiatry: Volume 42, Part 8, August 2003, Pages 886-894.
- Physicians Desk Reference. 63rd edition Montalve, NJ: Thomson PDR. 2009, (accessed online on 6/9/2009 at http://pdr.net/druginformation/DocumentSearchn_Local.aspx?DocumentID=08600140&DrugName=Catapres%20Tablets
- Rashid J, Mitelman S. Methylphenidate and Somatic Hallucinations. J of Am Acad Child Adolescent Psychiatry: Volume 46, Issue 8, August 2007, Pages 945-946.
Copyright Priory Lodge Education Limited 2010
First Published Novemnber 2010
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


