Browse through our Journals...
Spontaneous Intracranial Hypotension – case report
Dr. Mark L. Ansdell MBChB B.S.
Dr. Jason Ramtahal, MBBS PGTLCP MA MRCP
A 54 year old female with a 15-year history of recurrent left tibia osteomyelitis following a road traffic accident was admitted for elective debridement. She had mechanical aortic heart valve and was on lifelong Warfarin. Prior to surgery the patient’s Warfarin was stopped and a heparin infusion was initiated.
Day one post-operatively, she developed an acute severe headache, which she described as 10/10 in severity with associated nausea. The headache was constant, exacerbated on movement, which was progressively worse on sitting and standing. The patient could only gain relief by lying flat and staying completely still. She was photophobic but did not elicit any symptoms of meningeal irritation or signs of raised Intracranial pressure. The patient also described dizziness, and occasional diplopia.
She was afebrile and both systemic and neurological examinations were normal including no rash, no neurological deficit and no papilloedema. CT Head suggested some thickening of the meninges and MRI Brain showed meningeal enhancement with dilated lateral ventricles. The Neurology team agreed that the history and MRI changes were consistent with a diagnosis of spontaneous intracranial hypotension (see Figure 1).
Figure 1: Spontaneous Intracranial Hypotension
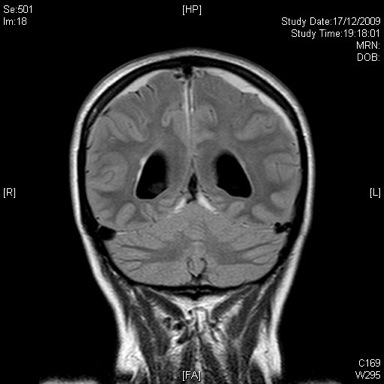
The repeat MRI eight weeks later did not show any change, however the patient’s symptoms had completely resolved after three weeks with conservative management.
Discussion:
Spontaneous intracranial hypotension (SIH) was first described by Schaltenbrand in 1938 (1). It is increasingly recognized as a noteworthy cause of new daily persistent, mainly postural headaches, although its initial misdiagnosis remains common (2). In addition to the typical orthostatic headache, patients may experience nausea, vomiting, anorexia, neck pain, dizziness, horizontal diplopia, changes in hearing, galactorrhea, facial numbness or weakness, or radicular symptoms involving the upper limb, all of which are orthostatic in nature (3).
MRI abnormalities include pachymeningeal gadolinium enhancement, subdural fluid collections, downward displacement of the cranial contents and pituitary hyperemia (4). In the investigation of SIH, a low opening pressure is typically found on lumbar puncture≤6 cmH2O, frequently with an elevated protein level. However the role of LP to demonstrate low CSF pressure and the timing of further investigations to identify a leak are recently debated, because they require a dural puncture that may worsen the patient’s condition (4).
Most cases of SIH are self-limiting and respond well to bed rest and aggressive oral hydration. If conservative measures fail to resolve symptoms, extradural saline infusions, or an epidural blood patch could be effective even if the source of the CSF fistula has not been demonstrated (5). Occasionally, open surgical procedures are required (6).
In this case, radiological investigations were contradictory to the clinical picture, and could have been detrimental. Due to the rash, our team avoided undertaking a lumbar puncture, which in hindsight could have worsened her symptoms. Once again, the clinical picture must be paramount, and investigations viewed with a healthy skepticism.
Reference:
1. Schaltenbrand G. Neuere Anschauungen zur Pathophysiologie der Liquorzirkulation. Zentralbl Neurochir 1938;3:290–9.
2. Schievink WI. Misdiagnosis of spontaneous intracranial hypotension. Arch Neurol 2003;60:1713–8.
3. Mokri B, Posner JB. Spontaneous intracranial hypotension: the broadening clinical and imaging spectrum of CSF leaks. Neurology 55:1771-1772, 2000
4. Berroir S, Loisel B, Ducros A, Boukobza M, Tzourio C, Valade D, Bousser MG. Early epidural blood patch in spontaneous intracranial hypotension. Neurology 2004;63:1950–1.
5. Benzon HT, Nemickas R, Molloy RE, Ahmad S, Melen O, Cohen B. Lumbar and thoracic epidural blood injections to treat spontaneous intracranial hypotension. Anesthesiology 1996;85:920–2.
6. Schievink WI, Morreale VM, Atkinson JL, Meyer FB, Piepgras DG, Ebersold MJ. Surgical treatment of spontaneous spinal cerebrospinal fluid leaks. J Neurosurg 1998;88:243–6.
First Published Sepetmber 2010
Copyright Priory Lodge Education Ltd. 2010 -
Click
on these links to visit our Journals:
Psychiatry
On-Line
Dentistry On-Line | Vet
On-Line | Chest Medicine
On-Line
GP
On-Line | Pharmacy
On-Line | Anaesthesia
On-Line | Medicine
On-Line
Family Medical
Practice On-Line
Home • Journals • Search • Rules for Authors • Submit a Paper • Sponsor us
All pages in this site copyright ©Priory Lodge Education Ltd 1994-


